In the rapidly evolving landscape of medical technology, the bridge between biological signals and digital interpretation is becoming increasingly seamless. At the heart of this intersection—literally and figuratively—lies the concept of atrial depolarization. While a physician might view this as a clinical milestone in a cardiac cycle, the tech industry views it as a critical data point, a bio-electrical signal that must be captured, filtered, and analyzed by sophisticated algorithms.
Understanding what atrial depolarization means in the context of modern technology requires looking beyond the anatomy of the heart. It involves exploring how sensors, artificial intelligence (AI), and wearable devices translate the microscopic movement of ions into actionable health insights. For tech professionals, software developers, and hardware engineers, atrial depolarization is the “input signal” that powers the next generation of preventative healthcare.
The Intersection of Biology and Bits: Understanding Atrial Depolarization
At its most fundamental level, atrial depolarization is the electrical trigger that causes the upper chambers of the heart (the atria) to contract. In the world of technology, this is viewed as a discrete electrical event. Before a muscle can move, there must be a change in electrical potential. This process involves the movement of sodium and potassium ions across cell membranes, creating a wave of electricity that can be measured on the surface of the skin.
The Bio-Electrical Signal: Defining the Basics
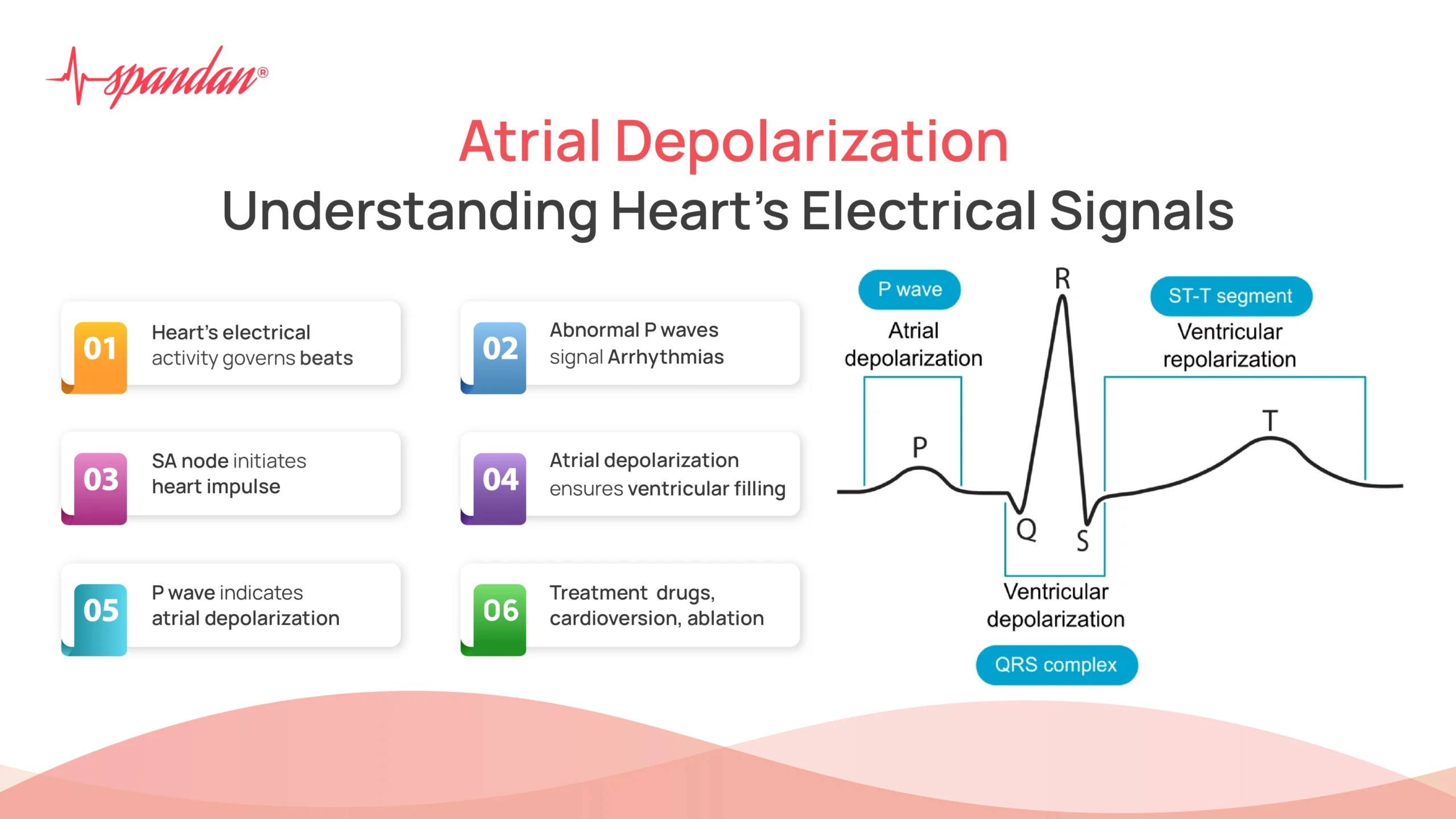
For a technologist, the heart is an autonomous biological circuit. The sinoatrial (SA) node acts as the natural pacemaker, sending out an electrical pulse. When we talk about atrial depolarization, we are describing the spread of this impulse through the atrial tissue. On an electrocardiogram (EKG or ECG), this is represented by the “P-wave.” This signal is the first major spike in a cardiac cycle, marking the beginning of a complex data sequence that high-tech monitors are designed to track with millisecond precision.
From Myocytes to Microchips: How Sensors Capture the Pulse
Capturing the P-wave is a significant engineering challenge. Because the atria are smaller than the ventricles, the electrical signal produced during atrial depolarization is relatively weak—often measuring in the range of microvolts. Tech companies must develop high-fidelity sensors with exceptional signal-to-noise ratios to distinguish this biological “whisper” from the background “noise” of other muscles or electronic interference. Modern MedTech utilizes silver/silver-chloride electrodes or, in the case of wearables, dry-contact stainless steel or titanium sensors to ensure that the subtle nuances of atrial depolarization are not lost in transmission.
The Evolution of EKG Technology: From Bedside Monitors to Wearables
For decades, monitoring atrial depolarization was a task reserved for heavy, stationary machines in clinical settings. Today, the digital transformation of electrocardiography has miniaturized this technology, placing the power of a 12-lead EKG lab onto the wrist of a consumer. This shift represents a monumental leap in hardware engineering and digital signal processing (DSP).
The Digital Transformation of Electrocardiography
Traditional EKGs rely on multiple leads to create a 3D view of the heart’s electrical activity. However, the tech industry has pioneered “single-lead” technology that focuses on the most critical vectors of the cardiac cycle. By utilizing advanced DSP, these devices can isolate the P-wave (the marker of atrial depolarization) even when the user is moving. This involves complex filtering algorithms that remove motion artifacts—the “noise” created by swinging arms or walking—allowing the clean electrical signal of the heart to emerge.
Wearable Integration: The Apple Watch and Beyond
The integration of EKG capabilities into consumer electronics like the Apple Watch, Fitbit, and Samsung Galaxy Watch has democratized access to cardiac data. These devices use a technique called photoplethysmography (PPG) for general heart rate monitoring, but for detecting the nuances of atrial depolarization, they switch to electrical sensors. When a user touches the “Digital Crown” or a side button, they complete a circuit that allows the device to measure the potential difference across the chest. This tech-driven approach has shifted the focus from reactive medicine to proactive monitoring, where the device “watches” for irregularities in depolarization patterns that the human user cannot feel.

AI and Machine Learning: Interpreting Depolarization Patterns
The true value of capturing atrial depolarization data lies not in the raw signal, but in the interpretation. This is where Artificial Intelligence and Machine Learning (ML) have become the most significant disruptors in the MedTech space. Once the hardware captures the P-wave, software must determine if that wave is “normal” or indicative of a pathology like Atrial Fibrillation (AFib).
Algorithmic Diagnosis: Beyond Human Pattern Recognition
In a clinical setting, a cardiologist looks at the shape, height, and timing of the P-wave to assess heart health. AI does this at a scale and speed that humans cannot match. Machine learning models are trained on millions of EKG strips to recognize the “signature” of healthy atrial depolarization. If the P-wave is absent, disorganized, or occurs at irregular intervals, the algorithm flags it. This automated interpretation is the backbone of “smart” alerts that notify users of potential heart issues before they become emergencies.
Predictive Analytics in Cardiac Health
The next frontier for tech in this niche is predictive analytics. By analyzing subtle changes in the morphology of atrial depolarization over weeks or months, AI can identify trends that might escape a one-time clinical checkup. For instance, if the duration of the P-wave is slowly increasing—a sign of atrial enlargement or conduction delays—an algorithm can alert the user to consult a specialist. This is “Software as a Medical Device” (SaMD) in action, turning raw biological data into a long-term wellness forecast.
Security and Data Privacy in Cardiac Monitoring Tech
As we transition to a world where our atrial depolarization patterns are constantly being uploaded to the cloud, the conversation must shift to digital security. Heart data is among the most sensitive forms of Personal Health Information (PHI). Protecting this data is a paramount concern for tech developers and cybersecurity experts.
Protecting Sensitive Bio-Data
Every time a wearable device records a P-wave, that data is usually synced to a smartphone and often to a cloud server. In the United States, this triggers the necessity for HIPAA (Health Insurance Portability and Accountability Act) compliance. Tech companies must implement end-to-end encryption to ensure that a user’s cardiac rhythm cannot be intercepted. The “unique” nature of a heartbeat—often referred to as a “cardiac signature”—means that this data could theoretically be used for biometric identification, making its protection even more critical.
The Cloud-Connected Heart: Risks and Rewards
The “Internet of Medical Things” (IoMT) allows for seamless sharing of data between patients and doctors. However, this connectivity introduces vulnerabilities. Firmware security for cardiac monitors is a specialized field of digital security. Ensuring that a device cannot be “spoofed” or that the data cannot be altered is essential for maintaining the integrity of medical diagnoses. As tech continues to evolve, we are seeing the rise of blockchain-based health records to provide immutable and secure logs of cardiac events like atrial depolarization.

The Future of Cardiac Tech: Beyond the Standard EKG
The future of understanding atrial depolarization lies in even more non-invasive and integrated technologies. We are moving toward a world where the environment around us monitors our biological signals without the need for wearable contact.
Innovations in “Contactless EKG” use ultra-wideband (UWB) radar and infrared sensors to detect the mechanical ripples caused by the heart’s electrical activity through clothing or even from across a room. This requires staggering amounts of compute power to filter out environmental noise. Furthermore, the development of “smart textiles”—clothing with conductive fibers woven directly into the fabric—will allow for 24/7 monitoring of atrial depolarization without the discomfort of a wristband or chest strap.
Ultimately, atrial depolarization is more than just a biological event; it is a fundamental unit of data in the digital health revolution. As technology continues to refine our ability to capture, analyze, and secure this signal, we move closer to a future where cardiac failure is not an unexpected tragedy, but a preventable technical anomaly. The “P-wave” is the start of the heartbeat, and in the world of Tech, it is the start of a data journey that is saving lives globally.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.