Cerebral hypoxia, a condition characterized by a reduced supply of oxygen to the brain, is a medical emergency that can lead to severe and lasting neurological damage if not promptly addressed. In an era defined by rapid technological advancement, our understanding, diagnosis, and management of cerebral hypoxia are increasingly intertwined with cutting-edge innovations. From advanced imaging techniques that visualize oxygen deprivation in real-time to AI-powered algorithms that predict outcomes and guide treatment, technology has become an indispensable ally in the fight against this debilitating condition. This article delves into cerebral hypoxia, framed through the lens of the technological tools and systems that empower medical professionals and offer hope for patients.
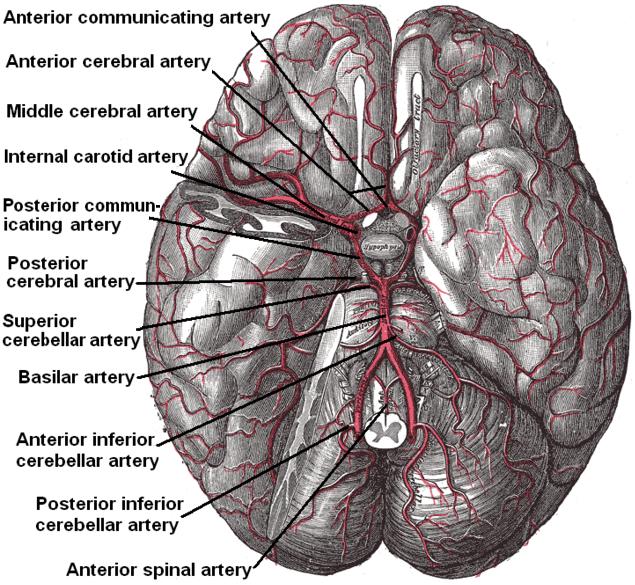
Unpacking Cerebral Hypoxia: A Technological Perspective on Brain Oxygen Deprivation
At its core, cerebral hypoxia is a simple concept with profound implications: the brain, a voracious consumer of oxygen, is deprived of its vital fuel. However, understanding the nuances of this deprivation – its causes, severity, and potential impact – relies heavily on sophisticated technological instruments.
The Brain’s Critical Need for Oxygen: Baseline Understanding via Neuroimaging and Monitoring Tech
The human brain, though only about 2% of body weight, demands roughly 20% of the body’s total oxygen supply. This continuous oxygen flow is essential for generating adenosine triphosphate (ATP), the energy currency that powers neuronal activity. When oxygen supply dwindles, even for a few minutes, neurons begin to suffer and die. Our fundamental understanding of this process has been greatly enhanced by technologies like functional magnetic resonance imaging (fMRI), which allows researchers to observe brain activity and blood flow changes in response to varying oxygen levels, and near-infrared spectroscopy (NIRS), which non-invasively measures cerebral oxygen saturation, providing crucial baseline data on healthy brain function. These technologies not only help us understand “normal” but also provide benchmarks against which hypoxic states can be measured.
Causes and Classifications: Identifying Hypoxic Events with Advanced Diagnostics
Cerebral hypoxia can stem from a variety of causes, broadly categorized by the degree and mechanism of oxygen deprivation. These include:
- Hypoxemic Hypoxia: Insufficient oxygen in the blood itself, often due to respiratory failure (e.g., severe asthma, drowning), high altitudes, or carbon monoxide poisoning. Modern pulse oximeters, smart spirometers, and blood gas analyzers (often integrated into hospital monitoring systems) are critical technologies for identifying and quantifying this type of hypoxia.
- Ischemic Hypoxia (Cerebral Ischemia): Reduced blood flow to the brain, meaning oxygenated blood isn’t reaching its target, even if blood oxygen levels are normal. This can result from strokes, cardiac arrest, or severe hypotension. Advanced cardiovascular monitoring systems, Doppler ultrasound for assessing cerebral blood flow, and specialized intracranial pressure (ICP) monitors are vital in detecting these circulatory disruptions.
- Anemic Hypoxia: Reduced oxygen-carrying capacity of the blood, typically due to severe anemia where there aren’t enough red blood cells. Automated hematology analyzers swiftly count and characterize blood cells, providing quick diagnostic insights.
- Histotoxic Hypoxia: Tissues are unable to utilize oxygen effectively, even if supply is adequate, often due to metabolic poisons like cyanide. While less direct, advanced toxicology screening technologies help confirm such causes.
Each classification requires specific diagnostic pathways, increasingly aided by integrated digital health platforms that correlate patient data from various monitoring devices to present a holistic picture to clinicians.
Recognizing the Signs: Leveraging Digital Tools for Early Detection
The symptoms of cerebral hypoxia vary depending on severity and duration, ranging from mild confusion and impaired judgment to seizures, coma, and brain death. Early recognition is paramount for intervention. While clinical observation remains vital, technology augments this significantly. Continuous EEG (electroencephalogram) monitoring systems, often connected to central nursing stations or even remote monitoring facilities, can detect subtle changes in brain electrical activity indicative of hypoxia before overt clinical signs appear. Furthermore, digital symptom checkers and AI-powered diagnostic support systems, while not replacing professional medical advice, can help individuals or first responders identify potential signs of severe oxygen deprivation, prompting faster emergency response. Wearable devices capable of tracking heart rate variability, blood oxygen saturation (SpO2), and even sleep patterns can provide pre-symptomatic or early warning indicators, especially in at-risk populations.
Technological Frontiers in Diagnosing Cerebral Hypoxia
The rapid evolution of medical technology has revolutionized our ability to diagnose cerebral hypoxia with unprecedented precision, speed, and non-invasiveness. These advancements are crucial for tailoring effective treatment strategies.
Advanced Neuroimaging: MRI, CT, and PET Scans for Brain Assessment
Neuroimaging plays a pivotal role in visualizing the structural and functional consequences of cerebral hypoxia.
- Magnetic Resonance Imaging (MRI): Particularly diffusion-weighted imaging (DWI) and perfusion imaging, can detect areas of restricted water movement (indicating cellular swelling and early brain injury) and reduced blood flow minutes after an acute hypoxic event. Advanced MRI sequences can also quantify metabolic changes and identify long-term damage, such as white matter lesions.
- Computed Tomography (CT) Scans: While less sensitive than MRI for early hypoxic changes, CT is widely available and rapid, making it crucial for initial assessment in emergency settings to rule out other causes of neurological impairment (e.g., hemorrhage) and to identify gross structural changes as hypoxia progresses. Newer CT perfusion techniques can also provide insights into cerebral blood flow.
- Positron Emission Tomography (PET) Scans: While not a first-line diagnostic for acute hypoxia, PET scans offer unique insights into cerebral metabolism and receptor function, invaluable for understanding the long-term metabolic impact of hypoxia and for research into recovery mechanisms. The fusion of PET with CT or MRI data creates even more comprehensive spatial and metabolic maps of the affected brain.
These imaging modalities are powered by sophisticated software for image acquisition, reconstruction, and analysis, often incorporating AI algorithms for automated lesion detection and quantitative assessment.
Non-Invasive Monitoring: Wearable Sensors and IoT for Continuous Oxygen Tracking
The ability to continuously monitor brain oxygenation and overall physiological status outside the confines of an ICU is a game-changer.
- Near-Infrared Spectroscopy (NIRS): As mentioned, NIRS devices, which can be affixed to the forehead, provide real-time, non-invasive measurements of regional cerebral oxygen saturation (rSO2). These compact devices, often integrated into multi-modal patient monitors or even standalone wearables, are crucial in critical care, surgery, and even in sports medicine to prevent hypoxia.
- Pulse Oximetry: Standard pulse oximeters, now widely available as consumer wearables (e.g., smartwatches, fitness trackers) alongside medical-grade devices, continuously measure peripheral blood oxygen saturation (SpO2). While not directly measuring brain oxygen, a drop in SpO2 is a critical indicator of systemic hypoxia that will inevitably affect the brain.
- Internet of Things (IoT) in Healthcare: The integration of various sensors (SpO2, heart rate, blood pressure, EEG) into an interconnected network allows for continuous, remote monitoring of at-risk patients. Data collected from these devices can be transmitted to cloud platforms, analyzed by algorithms for early warning signs, and reviewed by clinicians via telemedicine interfaces, enabling proactive interventions.
AI and Machine Learning in Diagnostic Accuracy and Predictive Analytics
Artificial intelligence (AI) and machine learning (ML) are rapidly transforming the diagnostic landscape for cerebral hypoxia.
- Image Analysis: AI algorithms can be trained on vast datasets of neuroimaging scans to detect subtle patterns indicative of hypoxic injury that might be missed by the human eye. They can segment brain regions, quantify lesion volumes, and even predict the likelihood of recovery based on initial scan features.
- Predictive Analytics: By integrating data from multiple sources – patient demographics, clinical history, vital signs from monitoring devices, laboratory results, and imaging findings – ML models can develop predictive scores for the risk of developing hypoxia, the severity of brain injury, and long-term neurological outcomes. This allows clinicians to stratify patients, allocate resources more effectively, and personalize treatment plans.
- Clinical Decision Support Systems (CDSS): AI-powered CDSS integrate guidelines, patient data, and real-time monitoring to provide recommendations to clinicians, helping them make faster, more informed decisions about diagnosis and immediate management of hypoxic events.
Mitigating Damage and Supporting Recovery: The Role of Medical Technology
Once cerebral hypoxia is diagnosed, the focus shifts to minimizing brain damage and supporting recovery. Here too, technology provides a powerful arsenal of tools and therapies.
Therapeutic Hypothermia and Targeted Temperature Management Systems
One of the most significant advances in managing post-hypoxic brain injury is therapeutic hypothermia, also known as Targeted Temperature Management (TTM). This involves deliberately lowering a patient’s core body temperature to 32-36°C (89.6-96.8°F) for 12-24 hours. The precise control of body temperature is achieved through sophisticated medical devices:
- External Cooling Devices: Specialized blankets, pads, or vests circulate cold water or air around the patient’s body. These systems include integrated sensors for continuous core temperature monitoring and feedback loops to maintain the target temperature within a very narrow range.
- Internal Cooling Devices: Catheters inserted into large blood vessels (e.g., femoral vein) circulate cold saline or use heat exchange balloons to cool the blood directly. These devices offer very precise and rapid temperature control.
TTM works by reducing the brain’s metabolic demand for oxygen, slowing down damaging biochemical processes, and mitigating inflammation and cell death pathways triggered by reperfusion injury.
Respiratory Support Devices: Ventilators and Oxygen Delivery Systems
Maintaining adequate oxygenation is fundamental.
- Mechanical Ventilators: For patients with severe respiratory compromise or altered consciousness, mechanical ventilators are critical life support devices. Modern ventilators are highly sophisticated, capable of delivering precise volumes and pressures of oxygen-enriched air, adapting to patient breathing patterns, and providing various modes of ventilation (e.g., pressure support, volume control). Integrated monitoring displays track lung mechanics, gas exchange, and alarm parameters.
- High-Flow Nasal Cannula (HFNC) and Non-Invasive Ventilation (NIV) Systems: These devices provide high concentrations of oxygen and some degree of positive airway pressure without the need for intubation, often used in less severe cases or during weaning from mechanical ventilation.
- Extracorporeal Membrane Oxygenation (ECMO): In the most severe cases of respiratory or cardiac failure leading to profound hypoxia, ECMO technology acts as an artificial lung and/or heart, oxygenating the blood outside the body and returning it, buying critical time for the patient’s own organs to recover.
Neurorehabilitation Technologies: VR, Robotics, and Brain-Computer Interfaces (BCIs)
Recovery from cerebral hypoxia can be a long and challenging journey, often involving extensive neurorehabilitation. Technology offers innovative approaches to maximize functional recovery.
- Robotic Rehabilitation: Robotic devices assist patients with motor deficits in performing repetitive, high-intensity movements of the limbs, improving strength, coordination, and range of motion. These devices can adapt to patient effort and provide objective feedback on progress.
- Virtual Reality (VR) and Augmented Reality (AR): VR environments create immersive, engaging, and customizable training scenarios for cognitive, motor, and balance rehabilitation. Patients can practice daily activities, navigate complex environments, and perform therapeutic exercises in a safe, controlled virtual space. AR overlays digital information onto the real world, assisting with visual perception, spatial awareness, and task performance.
- Brain-Computer Interfaces (BCIs): While still largely in research phases for cerebral hypoxia, BCIs hold immense promise. These technologies allow individuals to control external devices (e.g., prosthetics, computers) or even modulate their own brain activity (neurofeedback) directly using their thoughts, bypassing damaged neural pathways. For patients with severe motor impairments due to hypoxic injury, BCIs could offer new avenues for communication and functional independence.
- Functional Electrical Stimulation (FES): FES devices use electrical impulses to stimulate nerves and muscles, triggering movements in weakened or paralyzed limbs, thereby promoting muscle re-education and preventing atrophy.
Digital Health and Future Innovations in Hypoxia Management
The future of managing cerebral hypoxia is deeply rooted in the continued expansion of digital health paradigms and innovative biomedical research.
Telemedicine and Remote Patient Monitoring for Post-Hypoxia Care
As patients transition from acute care to long-term recovery, telemedicine and remote monitoring technologies ensure continuity of care.
- Virtual Consultations: Telemedicine platforms allow patients to consult with neurologists, rehabilitation specialists, and mental health professionals from their homes, reducing travel burden and improving access to specialized care, especially in rural areas.
- Remote Monitoring: Wearable sensors and smart home devices can continuously track vital signs, activity levels, sleep patterns, and adherence to medication for patients recovering at home. Data is securely transmitted to healthcare providers, who can intervene proactively if concerning trends emerge, preventing readmissions or complications.
- Digital Therapeutics: Apps and software programs designed to deliver evidence-based therapeutic interventions for cognitive rehabilitation, mood management, and medication adherence are becoming increasingly prevalent, providing scalable and personalized support.
Personalized Medicine through Genomic Data and AI-driven Treatment Plans
The ultimate frontier is personalized medicine, leveraging individual genetic makeup and AI to tailor interventions.
- Genomic Profiling: Understanding an individual’s genetic predispositions can help identify those at higher risk for certain types of hypoxic events or predict their response to specific treatments. Genomic data can inform the development of more targeted neuroprotective strategies.
- AI-driven Treatment Paths: By integrating genomic data with clinical profiles, real-time physiological measurements, and historical patient outcomes, AI can recommend highly personalized treatment plans. This could include precise drug dosages, optimized timing for therapeutic hypothermia, or tailored rehabilitation protocols designed to maximize individual recovery potential.

The Promise of Neuroprotective Drugs and Gene Therapies
While largely still in research, technological advancements are accelerating the discovery and development of novel therapies:
- Neuroprotective Drugs: High-throughput screening technologies and advanced computational modeling are identifying new compounds that can protect brain cells from damage during and after hypoxia. These drugs aim to mitigate excitotoxicity, oxidative stress, and inflammation.
- Gene Therapies: Gene editing technologies like CRISPR-Cas9 hold the potential to modify genes that influence the brain’s vulnerability to hypoxia or enhance its repair mechanisms, offering a long-term solution by addressing underlying genetic factors.
- Stem Cell Therapies: Research into using stem cells to replace damaged neurons or promote endogenous repair mechanisms is showing promise, with advanced cell culture techniques and delivery systems being critical technological enablers.
In conclusion, cerebral hypoxia, a grave threat to brain health, is being increasingly demystified and combated through the relentless march of technology. From the diagnostic precision offered by advanced imaging and AI to the therapeutic efficacy of sophisticated medical devices and the rehabilitative power of digital tools, technology stands as the bedrock of modern care for this challenging condition. As innovations continue to emerge, the outlook for patients affected by cerebral hypoxia will undoubtedly continue to improve, promising earlier detection, more effective treatments, and better quality of life.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.