In the traditional medical landscape, the question “what is bed sores?” usually elicits a clinical definition: localized injuries to the skin and underlying tissue, primarily caused by prolonged pressure. However, in the modern era of Digital Health and MedTech, the answer is evolving. Today, bed sores—or pressure ulcers—are increasingly viewed as a data-driven challenge that requires sophisticated technological interventions. As we move away from manual, labor-intensive care models, a new wave of software, AI tools, and smart hardware is redefining how we predict, prevent, and treat these complex injuries.
The Anatomy of a Medical Challenge: Why Bed Sores Demand High-Tech Solutions
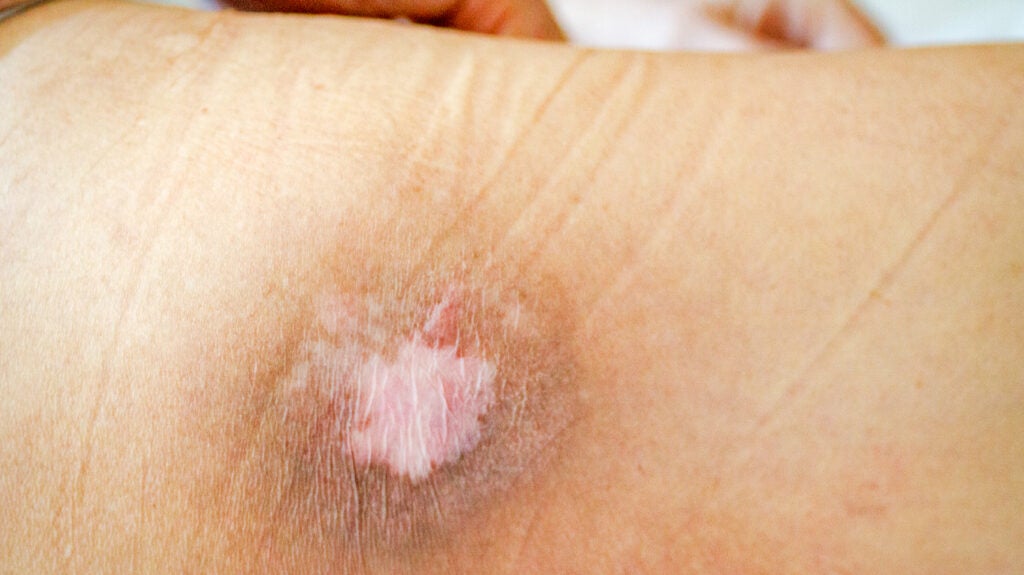
Before diving into the technological ecosystem, it is essential to understand the biomechanical complexity of pressure ulcers. Bed sores occur when pressure, friction, or shear forces disrupt blood flow to the skin, leading to cell death. In a clinical setting, managing this risk has historically relied on the “turn-clock” method—manually repositioning patients every two hours. However, this human-centric approach is prone to error and fails to account for the unique physiological nuances of individual patients.
Understanding the Biomechanics through Data
The tech industry sees bed sores not just as a wound, but as a failure of mechanical distribution. Modern research utilizes finite element analysis (FEA)—a software-based simulation technique used in engineering—to model how pressure is distributed across human tissue and bone. By digitizing the human body’s response to different surfaces, developers can create more effective preventative tools. This shift from “guessing” risk to “simulating” risk is the cornerstone of the new tech-centric approach to wound care.
The Data-Driven Approach to Identifying Risk
Digital transformation has introduced the concept of “Predictive Risk Modeling.” Instead of relying solely on the Braden Scale (a subjective clinical tool), hospitals are now integrating Electronic Health Record (EHR) data with machine learning algorithms. These algorithms analyze variables such as mobility scores, nutritional status, and moisture levels in real-time, flagging high-risk patients long before a physical sore appears.
Smart Surfaces and IoT-Enabled Pressure Management
The most significant physical intervention in the tech space involves the evolution of the hospital bed itself. No longer just a piece of furniture, the modern medical bed is an integrated IoT (Internet of Things) device designed to mitigate the physical causes of bed sores.
Active Support Surfaces and Sensor Integration
The latest “Smart Beds” are equipped with high-resolution pressure mapping systems. These systems utilize thousands of tiny capacitive sensors embedded within the mattress. These sensors generate a real-time heat map of the patient’s interface pressure. This data is then sent to a software dashboard, allowing caregivers to see exactly where the highest risk of tissue ischemia is occurring.
Real-Time Monitoring and Automated Repositioning
The pinnacle of this technology is the automated lateral rotation mattress. Managed by sophisticated software, these beds can autonomously adjust the air cells within the mattress to shift the patient’s weight without human intervention. By using AI to determine the optimal timing and angle of the shift, these systems ensure that no single area of the body remains under pressure for long enough to trigger a bed sore. This reduces the physical burden on healthcare staff and provides a level of precision that manual turning simply cannot match.
The Role of AI and Predictive Analytics in Wound Care
As with many industries, Artificial Intelligence is the “brain” behind the next generation of wound care. When we ask “what is bed sores” in a tech context, we are often talking about a problem that can be solved through computer vision and deep learning.
Machine Learning Models for Early Stage Detection
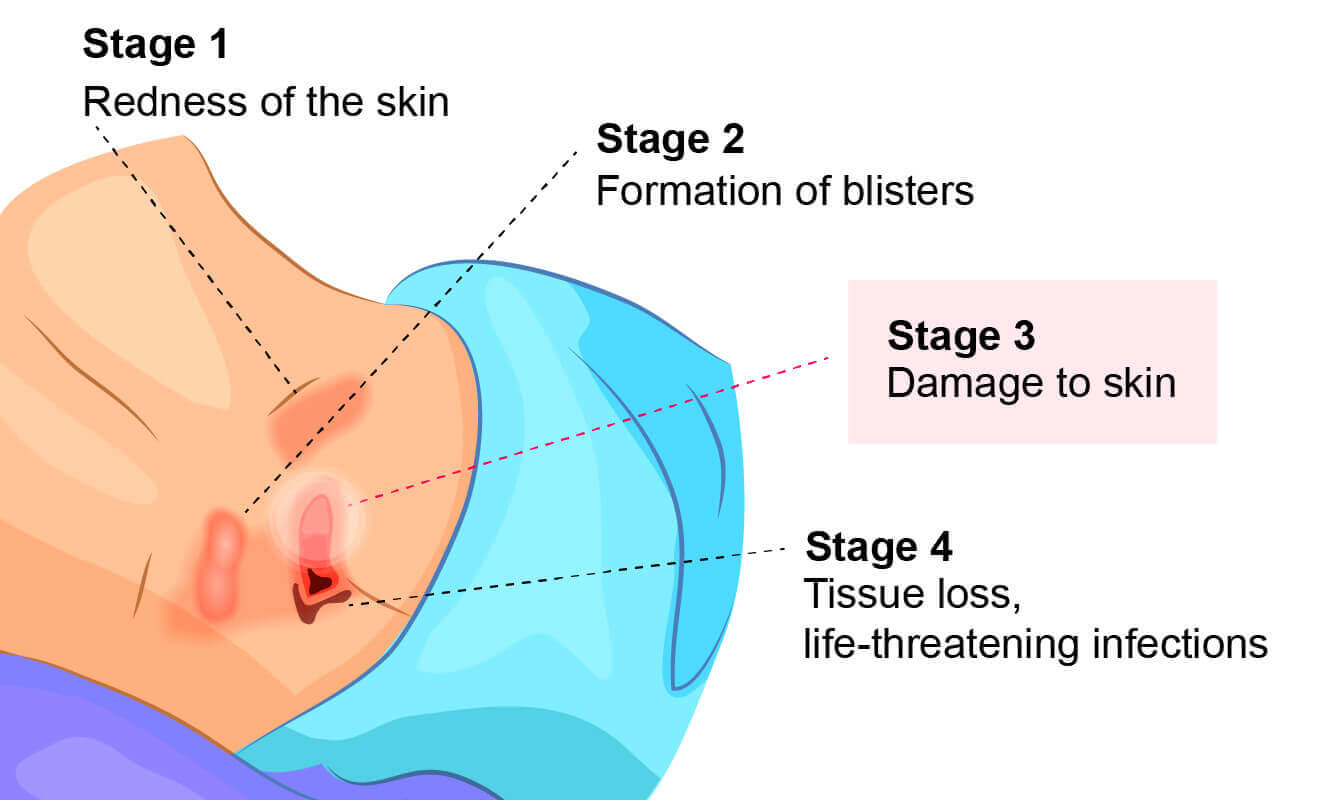
Early-stage bed sores (Stage 1) are notoriously difficult to detect with the naked eye, especially on patients with darker skin tones. Tech companies are now developing AI-powered handheld devices that use sub-epidermal moisture (SEM) sensors. These devices measure the “biocapacitance” of the tissue—detecting internal swelling and cell damage days before it becomes visible on the surface. The software interprets this data to provide a “risk score,” allowing for prophylactic treatment that prevents the sore from ever forming.
Computer Vision: Analyzing Tissue Health via Imaging
Once a bed sore has developed, managing it requires precise measurement and tracking. Traditional methods involve using a ruler and a camera, which are highly subjective. Enter AI-driven wound imaging apps. Using computer vision, these apps can take a 3D scan of a wound using a smartphone camera. The software automatically calculates the wound’s length, width, depth, and—most importantly—the percentage of different tissue types (necrotic, granulation, or epithelial). This data is stored in a cloud-based platform, allowing for longitudinal tracking that ensures the treatment plan is actually working.
Wearable Tech and Remote Patient Monitoring (RPM)
The challenge of bed sores extends far beyond the hospital. As “Hospital at Home” models become more popular, technology must bridge the gap between clinical oversight and home-based care.
Biosensors and Micro-Climate Regulation
Wearable biosensors are now being applied directly to the skin or integrated into “smart” clothing. These thin, flexible patches monitor the “micro-climate”—the specific temperature and humidity levels at the skin-surface interface. Excessive heat and moisture are primary catalysts for skin breakdown. When the software detects a spike in these metrics, it can trigger an alert on a caregiver’s smartphone, prompting immediate intervention.
Telehealth and the Future of Collaborative Wound Care
The integration of Remote Patient Monitoring (RPM) software allows wound care specialists to consult on cases from anywhere in the world. By utilizing high-definition video feeds and the aforementioned 3D imaging data, specialists can provide expert guidance to home-health nurses or family members. This democratization of expertise ensures that bed sore management is no longer limited by geographical location or the availability of in-house specialists.
The Future Roadmap: Robotics and Advanced Material Science
As we look toward the future, the technology surrounding bed sores is moving into the realm of soft robotics and advanced bio-materials.
Soft Robotics in Patient Handling
One of the leading causes of “shear”—a major contributor to bed sores—is the manual sliding of a patient up in bed. Tech firms are currently developing robotic “assistive devices” that use soft-robotics technology to gently glide patients into position. These robots use tactile sensors to ensure that the force applied never exceeds the threshold of skin integrity, effectively eliminating human error from the repositioning process.
Bio-printed Tissues and Synthetic Skins
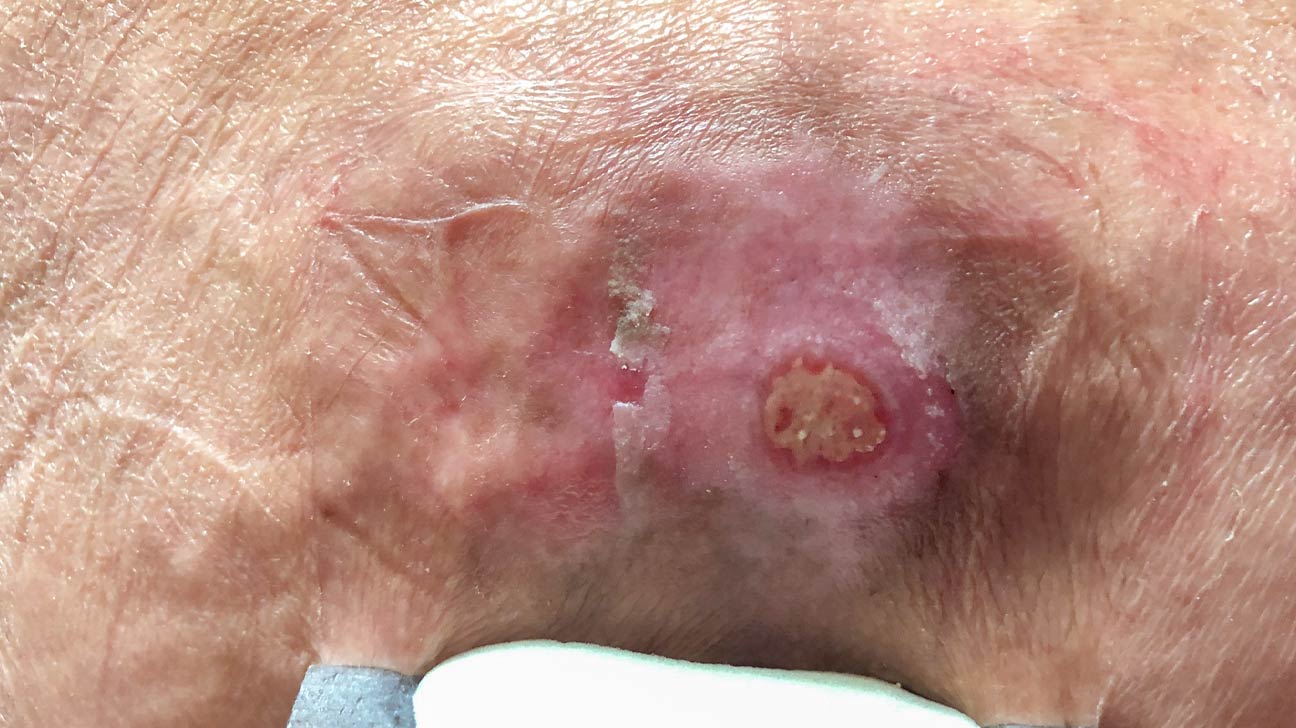
In cases where bed sores have reached advanced stages (Stage 3 or 4), the tech focus shifts to regenerative medicine. Scientists are experimenting with 3D bio-printing to create “skin patches” tailored to the specific dimensions of a patient’s wound. Furthermore, advanced “smart dressings” are being developed; these are bandages embedded with micro-chips that can release antibiotics or growth factors in response to specific chemical signals from the wound, such as a change in pH levels indicating infection.
Conclusion: A Proactive Tech Ecosystem
When we re-examine the question “what is bed sores?” through the lens of technology, it becomes clear that we are no longer looking at an inevitable complication of immobility. Instead, bed sores are becoming a “preventable data event.”
The convergence of IoT hardware, AI-driven diagnostics, and remote monitoring software is creating a safety net that protects the most vulnerable patients. While the physical reality of a pressure ulcer remains a serious medical concern, the tech industry has provided the tools to move from a reactive stance—treating wounds after they appear—to a proactive, predictive model of care. As these technologies become more accessible and integrated into standard medical practice, the “bed sore” may eventually become a relic of a pre-digital healthcare era.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.