For decades, the conversation surrounding male sterility was confined to the sterile walls of clinical laboratories and whispered conversations in urology offices. However, as we move deeper into the 2020s, the definition of what it means when a man is sterile is being rewritten not just by biology, but by disruptive technology. In the tech sector, sterility is no longer viewed as a static dead end; it is a complex data problem being solved by AI-driven diagnostics, microfluidic engineering, and wearable tech.
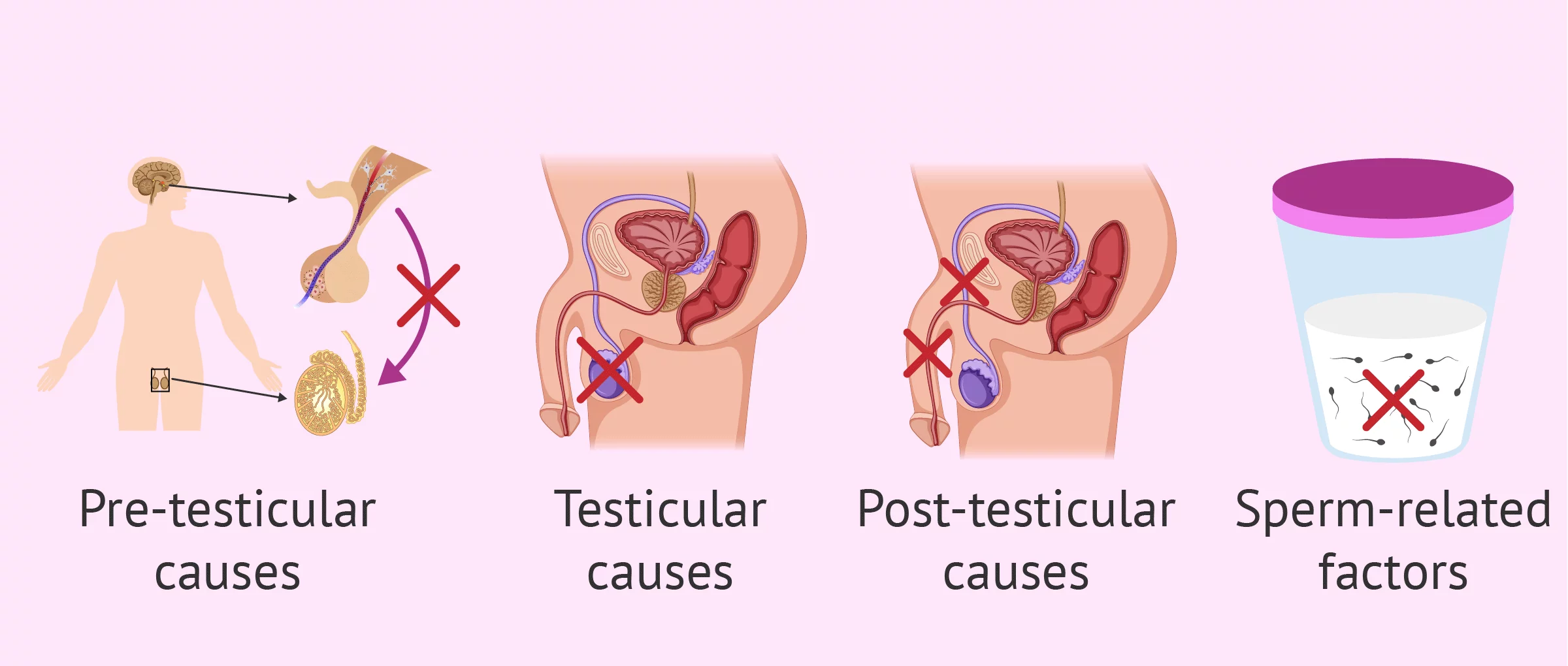
Understanding male sterility today requires a deep dive into the “MenTech” revolution—a burgeoning sub-sector of HealthTech that is bringing transparency, precision, and innovative solutions to a condition that affects millions of men globally.
Decoding Male Sterility Through Advanced Diagnostic Technology
In the traditional medical sense, sterility (or infertility) refers to the biological inability to contribute to conception. In the tech world, this is increasingly viewed through the lens of “bio-data.” For a man to be sterile, there is typically a failure in sperm production, transport, or function. Identifying which of these three pillars has failed now involves technologies that far surpass the capabilities of the manual microscope.
AI-Powered Semen Analysis (CASA)
The gold standard for diagnosing sterility is changing from human observation to Computer-Aided Sperm Analysis (CASA). Modern CASA systems utilize deep learning algorithms to track thousands of individual sperm cells in real-time. Where a human lab technician might miss subtle irregularities in morphology (shape) or motility (movement), AI models can identify patterns that indicate specific genetic or environmental causes of sterility. These AI tools provide a “fertility score” based on petabytes of comparative data, allowing for a more nuanced diagnosis than a simple “yes” or “no.”
Wearable Tech and Thermal Regulation
One of the leading causes of reversible male sterility is heat stress. The tech industry has responded with specialized wearables designed to monitor and regulate scrotal temperature. Advanced sensors integrated into smart fabrics can track temperature fluctuations throughout the day, syncing the data to a smartphone app. This provides men with actionable insights into how their lifestyle—such as sitting at a desk for long hours or using a laptop—directly impacts their reproductive health. By converting physiological heat into data points, tech is allowing men to mitigate “functional sterility” before it becomes a permanent condition.
The Rise of “MenTech”: Apps and Home Testing Ecosystems
The stigma surrounding male sterility often prevents men from seeking clinical help. This has paved the way for a massive influx of “At-Home Tech” that bridges the gap between the privacy of one’s home and the precision of a laboratory.
Smartphone-Integrated Microfluidics
The evolution of microfluidics—the manipulation of fluids at a sub-millimeter scale—has led to the creation of smartphone-based testing kits. These gadgets involve a small disposable slide that interacts with a clip-on optical attachment for a phone’s camera. The app then utilizes the phone’s processing power to perform a mini-semen analysis. For a man wondering if he is sterile, these tools offer a 95% to 99% accuracy rate compared to laboratory standards. This democratization of diagnostic tech is fundamentally changing the “patient journey,” moving the first point of contact from the doctor’s office to the digital interface.
Telehealth and Integrated Fertility Platforms
Being “sterile” in the modern era also means navigating a vast digital ecosystem of telehealth. Platforms specifically designed for male reproductive health are integrating EMR (Electronic Medical Records) with specialized consulting. If a home test indicates a low sperm count, the software immediately triggers a consultation with a specialist. This seamless integration of hardware (the test kit) and software (the telehealth platform) ensures that the diagnosis of sterility is followed by an immediate, tech-enabled roadmap for treatment.
Cutting-Edge Interventions: From Robotics to CRISPR

When sterility is confirmed, the tech industry’s role shifts from diagnosis to intervention. The “meaning” of sterility is being challenged by high-tech procedures that can extract viable genetic material even from men who were previously considered “hopeless” cases.
Robotic-Assisted Microsurgery
For men whose sterility is caused by physical blockages or varicoceles (swollen veins), robotic-assisted surgery is the new frontier. Systems like the Da Vinci surgical robot allow urologists to operate with a level of precision that is impossible for the human hand alone. These robots utilize 3D high-definition visualization and “EndoWrist” technology, which allows for microscopic suturing. This level of technological precision has significantly increased the success rates of reversing certain types of sterility, effectively “debugging” the male reproductive system.
The Future of Genetic Editing and IVG
Perhaps the most futuristic tech-solution to sterility lies in CRISPR-Cas9 and In-Vitro Gametogenesis (IVG). While still largely in the research and development phase, IVG technology aims to turn any cell in the body (such as a skin cell) into a sperm cell. In this context, being biologically sterile becomes a temporary hardware limitation that can be bypassed by “reprogramming” the body’s cells. Furthermore, CRISPR gene-editing technology holds the potential to fix the specific genetic mutations that cause azoospermia (the total absence of sperm). In the tech-driven future, sterility may be viewed as a “fixable code error” in the human genome.
Data Security and the Ethics of Bio-Information
As reproductive health becomes increasingly digitized, the definition of sterility expands into the realm of digital privacy and ethics. When a man uses an app to test his fertility, he is not just generating a medical result; he is creating highly sensitive “bio-information.”
Protecting Reproductive Data in the Cloud
The tech industry faces a significant challenge in securing fertility data. Because sterility can be a point of vulnerability or social stigma, the encryption of this data is paramount. Leading MenTech companies are now employing blockchain technology to ensure that fertility records are immutable and private. For a man navigating sterility, the “meaning” of his condition now includes his digital footprint and the security protocols used to protect his most intimate health data from breaches or third-party exploitation.
AI Bias in Fertility Algorithms
A growing concern in the tech community is the potential for AI bias in fertility diagnostics. If the datasets used to train fertility AI are not diverse, the software may provide inaccurate results for men of different ethnicities or ages. As we rely more on algorithms to tell us if a man is sterile, the “tech” must be scrutinized for its inclusivity. The industry is currently pushing for “Algorithmic Transparency,” ensuring that the code determining a man’s reproductive future is as unbiased and accurate as possible.
The Economic Integration of Fertility Tech
The final layer of what it means to be sterile in the tech era is the sheer scale of the “Fertility Tech” economy. Investors are pouring billions into startups that address male-factor infertility, recognizing that this is an underserved market compared to female-focused “FemTech.”
The “SaaS-ification” of Reproductive Care
We are seeing a shift toward “Fertility-as-a-Service” (FaaS). Companies are offering subscription-based models where men can store their genetic material in high-tech cryopreservation facilities (automated bio-banks) and monitor its viability through an app. This shift treats reproductive health as a long-term asset to be managed via a dashboard. For the modern man, sterility is no longer a static diagnosis but a variable that can be managed through a suite of technological services and cloud-based monitoring.
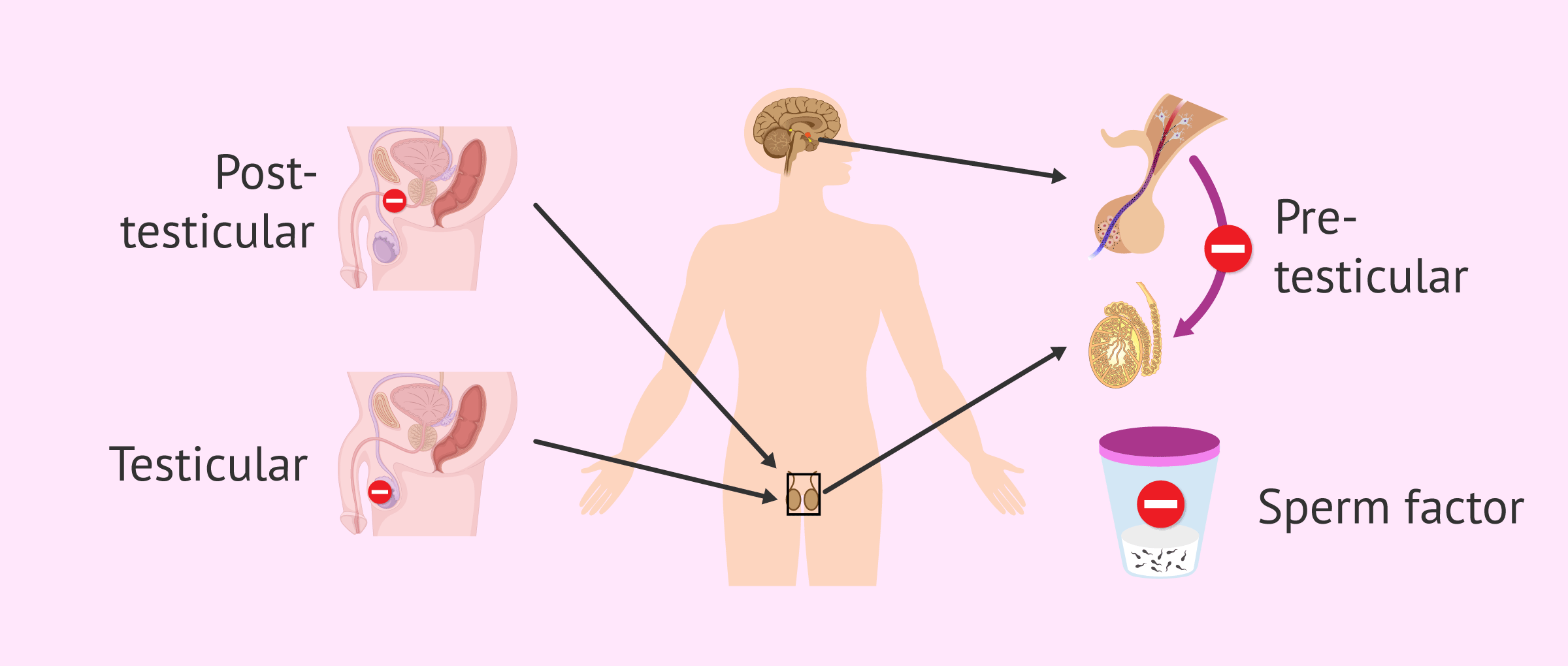
Conclusion: From Biology to Technology
To ask “what does it mean when a man is sterile” in the modern context is to ask a question about the limits of current technology. While the biological definition remains a challenge to conception, the technological definition is a “complex problem awaiting an innovative solution.”
Through the lens of AI, robotics, and microfluidics, sterility is being transformed from a permanent state of being into a data-driven challenge. As MenTech continues to evolve, the gap between “sterile” and “fertile” is being bridged by lines of code, precision sensors, and the relentless march of digital innovation. For the man of the future, a diagnosis of sterility is not the end of a story, but the beginning of a high-tech journey toward resolution.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.