Assertive Community Treatment (ACT) represents a transformative model in mental healthcare delivery, fundamentally reshaping how comprehensive services are provided to individuals facing severe mental illnesses. From a business and financial perspective, understanding ACT goes beyond its clinical methodology; it delves into its operational economics, its strategic positioning within value-based care frameworks, and its profound impact on long-term fiscal sustainability within healthcare systems. At its core, ACT is a highly intensive, integrated, and community-based approach designed to prevent recurrent crises, reduce hospitalizations, and support individuals in achieving maximum independence and quality of life in their own communities. For organizations navigating the complexities of healthcare finance, ACT emerges not just as a treatment philosophy but as a critical financial strategy aimed at optimizing resource allocation and demonstrating measurable return on investment.

The Economic Rationale for Community-Based Care
The business case for ACT is compelling, primarily driven by the escalating costs associated with traditional models of mental healthcare, which often rely heavily on acute care settings. Healthcare systems are under immense pressure to deliver effective care while simultaneously containing costs, making innovative service models like ACT increasingly attractive.
High Costs of Traditional Inpatient Models
Conventional mental health treatment pathways frequently involve repeated or prolonged inpatient hospitalizations, emergency room visits for crisis management, and extensive use of institutional care. These settings are inherently expensive due to their high overheads, specialized staffing requirements, facility costs, and the intensive nature of acute interventions. The average daily cost of an inpatient psychiatric bed can be substantial, and for individuals with chronic severe mental illness, the cumulative expense of multiple admissions over years can run into hundreds of thousands of dollars. Furthermore, the downstream costs extend to lost productivity, increased reliance on social welfare programs, and engagement with the criminal justice system, all of which represent significant financial burdens on both public and private sectors. From a business finance standpoint, these traditional approaches often represent a reactive, high-cost strategy with limited long-term impact on patient functionality and community integration.
ACT as a Cost-Effective Alternative
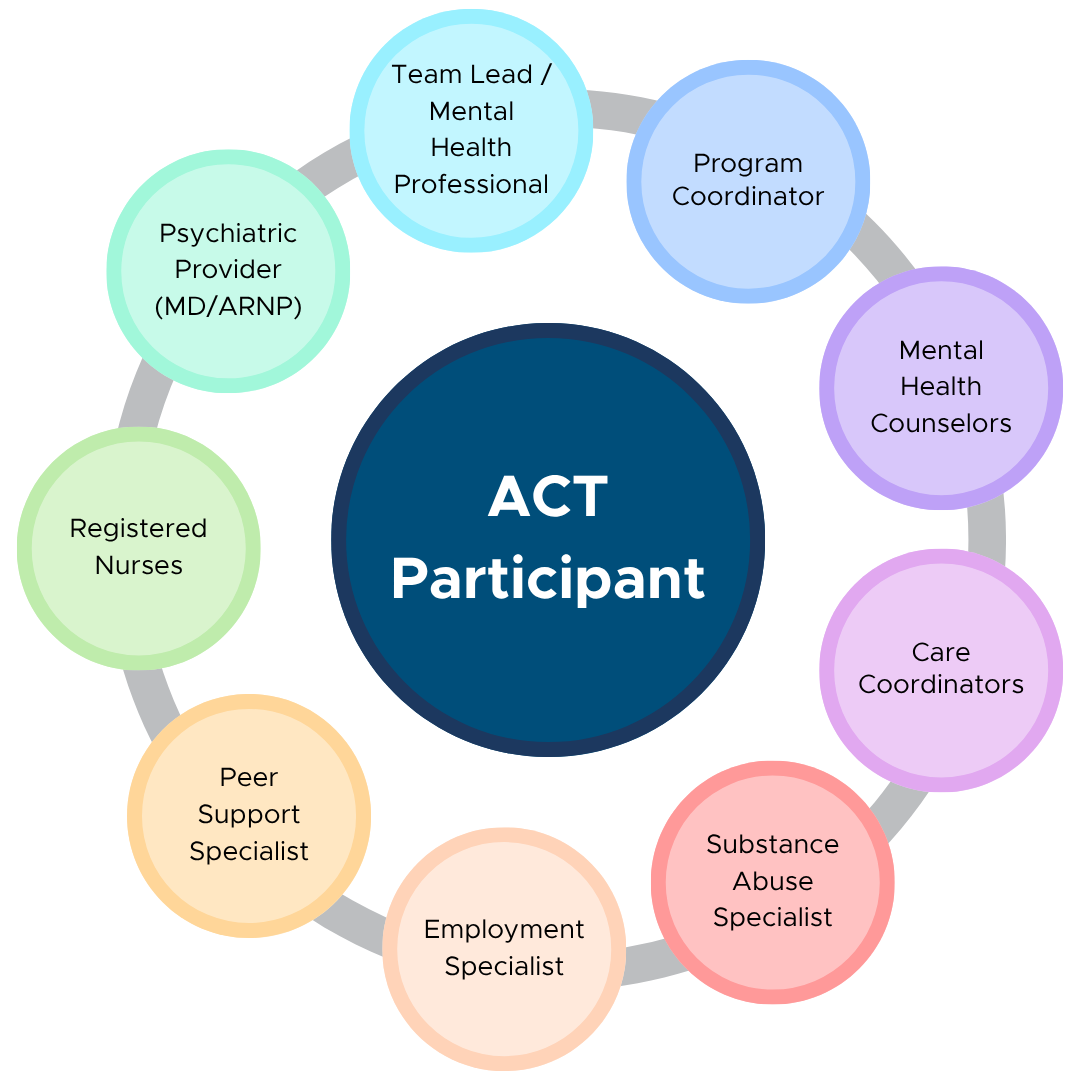
ACT directly addresses the financial inefficiencies of traditional care by shifting the locus of treatment from expensive institutional settings to the community. By providing intensive, proactive, and individualized support where individuals live, work, and socialize, ACT aims to avert crises before they necessitate costly inpatient care. The ACT model is designed to be highly accessible and responsive, with staff-to-patient ratios often more intensive than typical outpatient services, allowing for rapid intervention when early signs of distress appear. The multidisciplinary team (which often includes psychiatrists, nurses, social workers, employment specialists, and peer support specialists) works collaboratively to address a wide range of needs—clinical, social, vocational, and housing—in a holistic manner. This comprehensive, preventive approach, when effectively implemented, demonstrably reduces the frequency and duration of inpatient stays and emergency service utilization, thereby yielding substantial cost savings for payers and providers alike. The investment in an ACT team is thus seen as a strategic allocation of resources that prevents more significant expenditures down the line, repositioning mental health services from an expense to a value-generating investment.
Operationalizing ACT: A Business Finance Perspective
Implementing and sustaining an ACT program requires careful financial planning and robust operational management. The structure of an ACT team, its resource requirements, and the various funding mechanisms present unique challenges and opportunities from a business finance standpoint.
Staffing and Resource Allocation
The ACT model mandates a highly specialized, multidisciplinary team, which represents a significant portion of an ACT program’s operational budget. Recruiting and retaining qualified professionals across various disciplines (e.g., psychiatric prescribers, registered nurses, licensed therapists, vocational specialists) is crucial but also costly. From a business finance perspective, effective salary management, benefits packages, and professional development are vital for attracting top talent and minimizing turnover, which can disrupt care continuity and incur additional recruitment expenses. Furthermore, ACT teams operate in the community, necessitating resources for transportation (fleet vehicles, mileage reimbursement), mobile technology for electronic health records and communication, and access to community-based resources. Strategic resource allocation involves optimizing team size, managing caseloads efficiently, and investing in technology that enhances operational effectiveness, all while adhering to the fidelity standards that ensure the program’s clinical and financial efficacy. Developing a detailed budget that accounts for these direct and indirect costs, and regularly reviewing variances, is essential for financial health.
Funding Models and Reimbursement Challenges
The financial viability of ACT programs heavily depends on sustainable funding and appropriate reimbursement models. Historically, funding for ACT has varied widely, often relying on a patchwork of state and federal grants, Medicaid waivers, and, less frequently, private insurance. The shift towards value-based care, where providers are reimbursed based on outcomes rather than solely on services rendered, presents both challenges and opportunities. For ACT, which demonstrates clear outcome improvements (e.g., reduced hospitalizations), this shift can be advantageous. However, navigating complex reimbursement structures—including bundled payments, capitated rates, or fee-for-service models for specific interventions—requires sophisticated billing systems, accurate documentation, and strong financial reporting capabilities. Organizations must invest in robust administrative infrastructure to track service delivery, manage claims, and demonstrate compliance with payer requirements. Advocating for payment models that recognize the comprehensive, continuous nature of ACT services, rather than discrete billable units, is a critical ongoing task for program sustainability and financial health.
Return on Investment: Beyond Clinical Outcomes

While ACT’s primary goal is to improve the lives of individuals with severe mental illness, its robust outcomes translate directly into tangible financial benefits, making it an attractive proposition for payers, providers, and public health systems seeking a strong return on investment (ROI).
Reduced Hospitalizations and Emergency Room Visits
Perhaps the most direct and significant financial ROI of ACT is its documented effectiveness in dramatically reducing the need for costly inpatient psychiatric hospitalizations and emergency room visits. By proactively managing symptoms, providing crisis intervention in the community, and ensuring consistent medication adherence and support, ACT teams mitigate the drivers of acute care utilization. Each avoided hospitalization or ER visit represents substantial savings. For instance, preventing even a few 10-day inpatient stays at several thousand dollars per day can quickly offset a significant portion of an ACT team’s operational costs. Organizations that can quantify these avoided costs through rigorous data collection and analysis are better positioned to demonstrate the financial value of their ACT programs to payers and funding bodies.
Improved Social and Vocational Functioning
Beyond immediate healthcare cost avoidance, ACT contributes to broader economic benefits by fostering greater independence and community integration among its clients. Through vocational support, housing assistance, and life skills training, ACT helps individuals secure and maintain employment, reducing their reliance on disability benefits and increasing their contributions to the local economy. Improved housing stability lessens the burden on homeless services and shelters. These outcomes represent a long-term societal ROI, transforming individuals from recipients of extensive public assistance into contributing members of their communities. While harder to quantify in immediate balance sheets, these benefits translate into reduced public expenditures across multiple sectors and enhanced civic participation, bolstering the overall economic health of a community.
Long-Term Fiscal Sustainability
From a strategic business finance perspective, investing in ACT is an investment in the long-term fiscal sustainability of the entire healthcare system. By preventing chronic relapses, reducing institutionalization, and promoting self-sufficiency, ACT programs contribute to a healthier, more productive population. This approach lessens the strain on acute care resources, frees up valuable hospital beds, and potentially reduces the overall per capita healthcare expenditure for individuals with severe mental illness over their lifetime. Organizations that prioritize ACT are not just delivering better care; they are adopting a financially responsible strategy that aligns with broader public health goals of cost containment and value-based care delivery, positioning themselves as forward-thinking leaders in mental health service provision.
Navigating Financial Complexities and Future Outlook
The evolving landscape of healthcare finance demands a proactive and data-driven approach to manage and expand ACT programs effectively. Navigating financial complexities will be key to their continued success and growth.
Data-Driven Decision Making
For ACT programs to thrive financially, robust data collection and analytical capabilities are indispensable. Programs must meticulously track not only clinical outcomes but also operational costs, service utilization patterns, and, critically, averted costs of higher levels of care. Financial dashboards that integrate clinical and financial data allow administrators to monitor key performance indicators, identify areas for efficiency improvement, and demonstrate the program’s value proposition to stakeholders. Implementing advanced analytics to conduct cost-benefit analyses, measure ROI, and project future savings provides compelling evidence for continued investment. This data-driven approach empowers program leaders to make informed financial decisions, secure new funding, and continuously optimize operations.
Advocacy for Sustainable Funding
The long-term success of ACT relies heavily on securing stable and adequate funding streams that acknowledge its comprehensive nature and proven outcomes. This necessitates ongoing advocacy with state and federal policymakers, managed care organizations, and private insurers. Business leaders in the mental health sector must articulate the strong financial case for ACT, emphasizing its capacity to reduce overall healthcare expenditures while improving lives. This advocacy includes pushing for payment models that incentivize preventive, community-based care and support the full scope of ACT services, rather than fragmenting reimbursement. Demonstrating financial transparency and consistently delivering measurable value are powerful tools in this advocacy effort, building trust and garnering support for sustainable investment in ACT programs.
Innovation in Payment Models
The future of ACT’s financial sustainability will likely involve innovative payment models that move beyond traditional fee-for-service. Exploring opportunities such as population health management contracts, risk-sharing agreements, or social impact bonds could provide new avenues for funding and incentivize even greater efficiency and outcome achievement. For instance, payment models that reward providers for keeping individuals out of the hospital could directly benefit ACT programs, aligning financial incentives with the core mission of community integration and crisis prevention. Organizations that are agile in adapting to and even shaping these new financial landscapes will be best positioned to lead in the delivery of effective and financially sound assertive community treatment.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.