The journey to managing depression is often a complex and deeply personal one. While psychotherapy and lifestyle changes play crucial roles, medication remains a cornerstone of treatment for many individuals. However, the sheer volume of information, evolving research, and individual biological variations can make understanding “what medication for depression” a daunting task. This article delves into the technological advancements and digital tools that are revolutionizing how we approach, prescribe, and monitor antidepressant medications, offering a more informed and personalized path to recovery.
The Evolving Landscape of Antidepressant Discovery and Development
The development of antidepressant medications has been a continuous process, marked by breakthroughs in our understanding of brain chemistry and neurobiology. Technology has been instrumental in accelerating this progress, moving from serendipitous discoveries to highly targeted drug design.
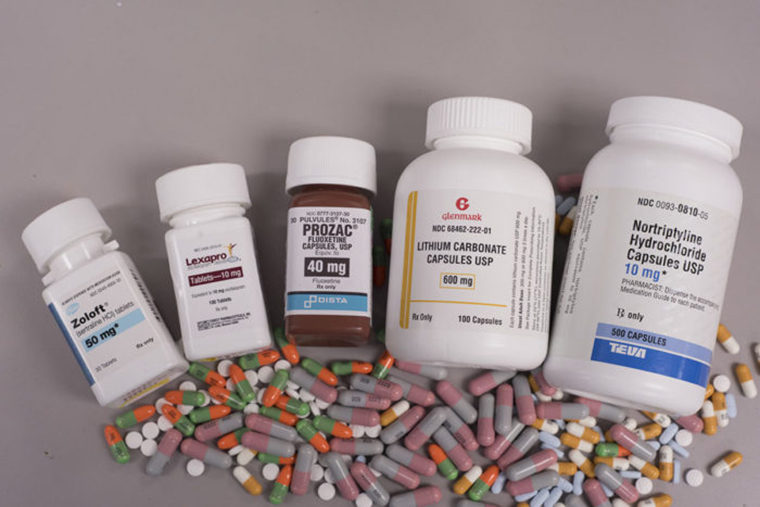
From Serendipity to Science: The Evolution of Antidepressant Classes
The early days of antidepressant development were characterized by observations made during the treatment of other conditions. For instance, iproniazid, initially developed for tuberculosis, was found to elevate mood. Similarly, imipramine, designed as an antipsychotic, demonstrated antidepressant properties. These early findings laid the groundwork for understanding the role of neurotransmitters, particularly serotonin and norepinephrine, in mood regulation.
The development of Selective Serotonin Reuptake Inhibitors (SSRIs) in the late 1980s represented a significant leap forward. Drugs like fluoxetine (Prozac) offered a more targeted approach by inhibiting the reabsorption of serotonin, thereby increasing its availability in the synaptic cleft. This was a technological advancement in drug design, allowing for greater specificity and often fewer side effects compared to older tricyclic antidepressants (TCAs) and monoamine oxidase inhibitors (MAOIs).
More recently, research has explored other neurotransmitter systems and signaling pathways. Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs), such as venlafaxine, target both serotonin and norepinephrine. Atypical antidepressants, like bupropion (which primarily affects dopamine and norepinephrine) and mirtazapine (which acts on different serotonin and noradrenergic receptors), further diversify the treatment options. The ongoing research, fueled by sophisticated imaging techniques and genetic sequencing, continues to uncover new targets and mechanisms for drug development.
The Role of Big Data and AI in Drug Discovery
The sheer volume of biological and clinical data generated today is unprecedented. Big data analytics and artificial intelligence (AI) are now indispensable tools in the pharmaceutical industry for antidepressant discovery and development. Machine learning algorithms can analyze vast datasets of genetic information, patient records, and molecular structures to identify potential drug candidates and predict their efficacy and safety profiles.
AI-powered platforms can sift through millions of compounds, simulating their interactions with target proteins in the brain. This accelerates the initial stages of drug discovery, significantly reducing the time and cost associated with identifying promising leads. Furthermore, AI can help in optimizing drug formulations and predicting potential side effects, leading to the development of safer and more effective medications. The ability to analyze complex biological pathways and identify novel therapeutic targets is a testament to the transformative power of technology in this field.
Personalized Medicine: Tailoring Antidepressant Treatment with Digital Insights
The concept of “one size fits all” is increasingly being challenged in mental health, and this is particularly true for antidepressant medication. Individual responses to medications vary due to genetic predispositions, metabolic rates, and co-existing health conditions. Technology is at the forefront of enabling a more personalized approach to antidepressant treatment.
Pharmacogenomics: Decoding Your Genetic Blueprint for Medication Response
Pharmacogenomics, the study of how genes affect a person’s response to drugs, is revolutionizing antidepressant prescribing. Genetic testing can identify variations in genes responsible for metabolizing certain medications (like the cytochrome P450 enzymes) or those involved in neurotransmitter pathways. This information can help predict whether a patient is likely to respond well to a particular antidepressant, require a higher or lower dose, or be at increased risk of adverse effects.
For example, certain genetic variations might indicate that a patient will metabolize SSRIs too quickly, rendering them less effective, or too slowly, increasing the risk of side effects. By incorporating pharmacogenomic data into the prescribing decision, clinicians can bypass the trial-and-error process for many patients, leading to faster symptom relief and improved treatment outcomes. This is a direct application of advanced bioinformatics and genetic sequencing technologies to clinical practice.
Digital Phenotyping and Wearable Technology for Treatment Monitoring
Beyond genetics, real-time behavioral data is emerging as a powerful tool for understanding and monitoring depression. Digital phenotyping involves collecting data from smartphones and other wearable devices to identify patterns of behavior that may indicate changes in mood or mental state. This can include tracking sleep patterns, physical activity levels, social interactions (e.g., frequency of calls or texts), and even typing speed.
Wearable devices, such as smartwatches and fitness trackers, can continuously collect physiological data like heart rate variability and sleep quality. AI algorithms can then analyze this data to detect subtle shifts that might precede a relapse or indicate that a current medication is not fully effective. This passive data collection provides a more objective and continuous assessment of a patient’s well-being than traditional, episodic clinic visits. This technology allows for a more dynamic understanding of how medications are impacting daily life and mood, enabling timely adjustments to treatment plans.
The Digital Ecosystem of Mental Health Support and Medication Management

The technological advancements in understanding and prescribing antidepressants are complemented by a growing ecosystem of digital tools designed to support patients throughout their treatment journey. These platforms aim to improve adherence, provide accessible resources, and foster communication between patients and their healthcare providers.
Telehealth and Virtual Care Platforms for Accessible Psychiatry
The COVID-19 pandemic accelerated the adoption of telehealth, making mental health services more accessible than ever before. Virtual care platforms allow individuals to consult with psychiatrists and therapists remotely, overcoming geographical barriers and reducing the stigma associated with seeking help. These platforms often integrate secure messaging, video conferencing, and appointment scheduling, streamlining the process of receiving mental healthcare.
For individuals prescribed antidepressant medication, telehealth offers a convenient way to have follow-up appointments, discuss side effects, and have their prescriptions adjusted without needing to travel to a clinic. This increased accessibility can significantly improve treatment adherence, a critical factor in the successful management of depression.
Digital Therapeutics (DTx) and AI-Powered Companion Apps
Beyond direct medical consultations, a new category of digital interventions, known as Digital Therapeutics (DTx), is emerging. These are clinically validated software-based interventions designed to prevent, manage, or treat a medical disorder or disease. Some DTx applications are specifically designed to complement antidepressant medication by providing evidence-based therapeutic exercises, mood tracking tools, and educational content.
AI-powered companion apps can offer personalized support, providing coping strategies, mindfulness exercises, and even chatbot interactions to help users navigate challenging emotions. These tools can act as a constant source of support, reinforcing therapeutic principles learned in therapy and encouraging consistent medication adherence. The integration of these apps with electronic health records is a future frontier, allowing for a more holistic view of patient care.
Secure Data Management and Patient Portals for Enhanced Information Flow
The responsible use of technology in mental health necessitates robust data security and privacy measures. Electronic health records (EHRs) and secure patient portals are crucial for managing sensitive medical information, including prescription details, treatment history, and genetic data. These systems ensure that patient information is stored securely and can be accessed by authorized healthcare providers, facilitating coordinated care.
Patient portals empower individuals to access their health records, communicate with their care team, and request prescription refills. This increased transparency and control can foster a greater sense of agency in managing their mental health. Furthermore, the anonymized and aggregated data collected through these systems can contribute to ongoing research and the development of more effective treatment strategies.
Navigating the Future: Ethical Considerations and Technological Advancements
As technology continues to integrate into mental health treatment, it’s essential to consider the ethical implications and anticipate future advancements. The goal is to leverage technology responsibly to improve outcomes for individuals struggling with depression.
The Ethics of AI in Diagnosis and Treatment Recommendation
The increasing reliance on AI in healthcare raises important ethical questions. Ensuring algorithmic transparency, mitigating bias in AI models, and maintaining human oversight are critical. While AI can assist in identifying patterns and recommending potential treatments, the final clinical decision must always rest with a qualified healthcare professional. The focus should be on AI as a powerful assistant, not a replacement for human judgment and empathy.
Data Privacy, Security, and the Digital Divide
Protecting patient data is paramount. Robust cybersecurity measures are needed to prevent breaches and ensure that sensitive mental health information remains confidential. Additionally, addressing the digital divide is crucial. Not everyone has equal access to smartphones, reliable internet, or the digital literacy required to benefit from these technologies. Efforts must be made to ensure equitable access to digital mental health resources for all populations.

The Promise of Neurotechnology and Biofeedback for Antidepressant Augmentation
Looking ahead, emerging neurotechnologies hold significant promise for augmenting antidepressant treatment. Techniques like transcranial magnetic stimulation (TMS) and transcranial direct current stimulation (tDCN) are non-invasive brain stimulation methods that are showing efficacy in treating depression. While not medications themselves, they represent technological interventions that can be used alongside or in place of pharmacotherapy.
Biofeedback, which allows individuals to learn to control physiological functions like heart rate and muscle tension, is also being explored as a complementary approach to managing stress and anxiety, which often co-occur with depression. The integration of these advanced technological interventions with medication management offers a glimpse into a future of highly personalized and multi-modal approaches to treating depression.
In conclusion, while the question of “what medication for depression” is fundamentally a clinical one, the landscape of answering it is rapidly being reshaped by technology. From the AI-driven discovery of new drugs to pharmacogenomic tailoring of prescriptions and the supportive ecosystem of digital health tools, technology is empowering individuals and clinicians with more precise, personalized, and accessible pathways to managing depression. As these advancements continue to unfold, a future where mental well-being is more effectively and compassionately supported by technological innovation appears increasingly within reach.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.