The advent of Magnetic Resonance Imaging (MRI) has revolutionized diagnostic medicine, offering an unprecedented ability to visualize the intricate structures within the human body. Among its many applications, the cervical MRI stands out as a critical tool for understanding the health and condition of the cervical spine – the uppermost section of the vertebral column, comprising the seven vertebrae that support the head and connect it to the rest of the spine. This non-invasive imaging technique utilizes powerful magnetic fields and radio waves to generate detailed cross-sectional images, providing physicians with invaluable insights into a wide range of potential issues affecting this crucial area.
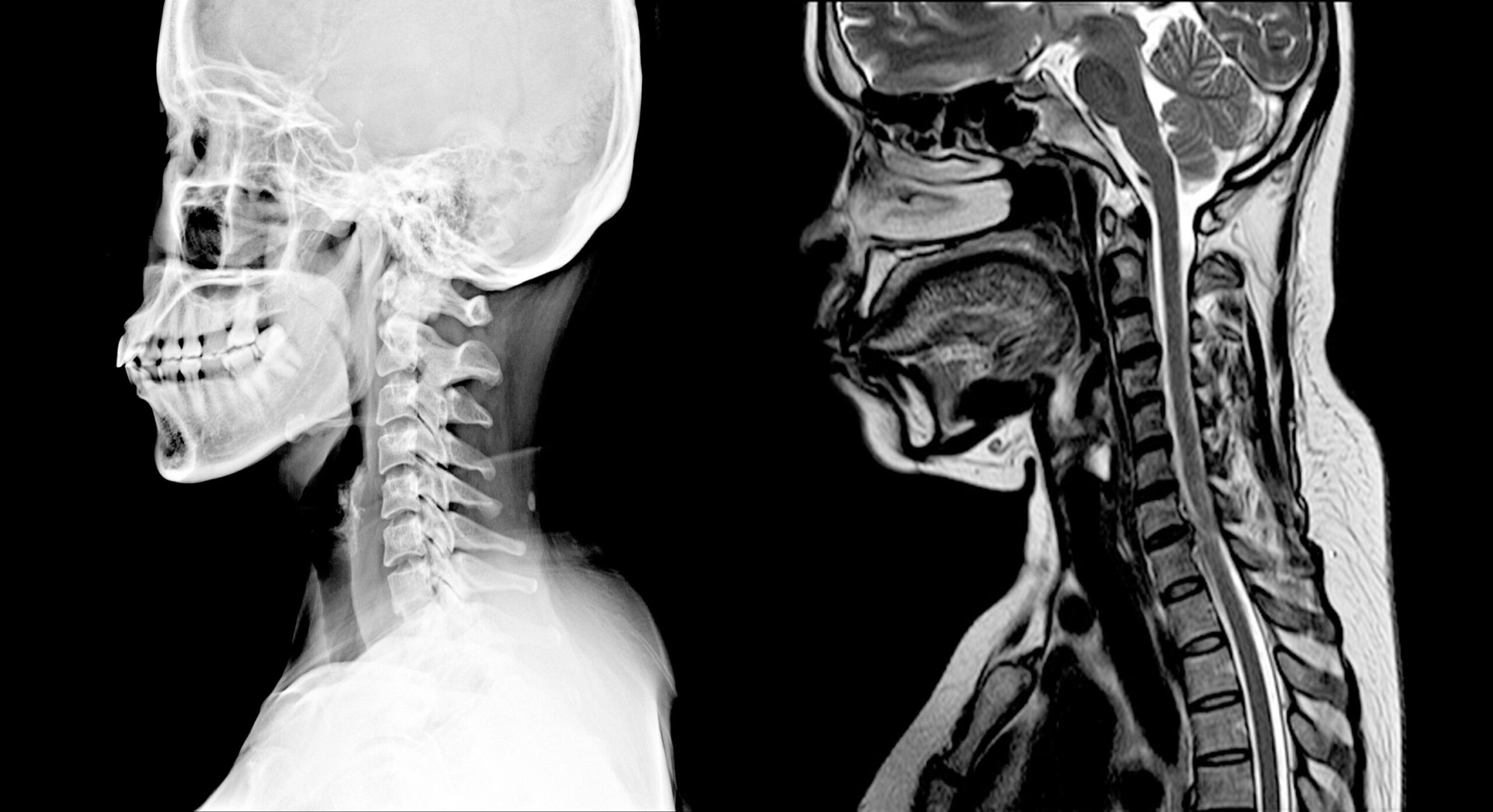
The cervical spine is a marvel of biomechanical engineering, housing the spinal cord, nerve roots, intervertebral discs, ligaments, muscles, and bones. Its flexibility allows for a remarkable range of motion, enabling us to turn our heads and maintain balance. However, this inherent mobility also makes it susceptible to injury and degenerative changes. A cervical MRI is instrumental in diagnosing and evaluating conditions that can compromise the function of this vital region, impacting everything from posture and sensation to motor control and even breathing. Understanding what a cervical MRI can reveal is key to appreciating its diagnostic power and its role in guiding effective treatment strategies.
Unveiling the Anatomical Landscape: What a Cervical MRI Visualizes
At its core, a cervical MRI is designed to provide a high-resolution view of the soft tissues and bony structures of the neck. Unlike X-rays, which primarily show bone density, or CT scans, which offer detailed bone imaging and some soft tissue detail, MRIs excel at differentiating between various soft tissues. This is achieved through the manipulation of water molecules within the body’s tissues. The strong magnetic field aligns these molecules, and radio waves are then used to perturb this alignment. As the molecules realign, they emit signals that are detected and processed by a computer to create detailed images.
The Spinal Cord: A Vital Conduit
The most critical structure visualized in a cervical MRI is the spinal cord itself. This thick bundle of nerve tissue extends from the brainstem down through the vertebral canal. It serves as the primary communication highway between the brain and the rest of the body, transmitting motor commands and sensory information. An MRI can reveal a variety of abnormalities affecting the spinal cord, including:
- Compression: This can occur due to herniated discs, bone spurs (osteophytes), tumors, or thickened ligaments. Compression can lead to symptoms such as pain, numbness, tingling, weakness, and even paralysis, depending on its severity and location. The MRI can precisely pinpoint the source and extent of this compression, allowing for targeted interventions.
- Inflammation (Myelitis): Conditions like transverse myelitis or multiple sclerosis (MS) can cause inflammation of the spinal cord. An MRI can detect these inflammatory lesions, often appearing as areas of increased signal intensity, helping to diagnose and monitor these complex neurological conditions.
- Tumors: Both primary tumors originating within the spinal cord (intramedullary) and tumors pressing on the spinal cord from outside (extramedullary) can be identified. The MRI’s contrast capabilities are particularly useful in differentiating tumor tissue from surrounding healthy tissue.
- Ischemia (Lack of Blood Flow): In rare cases, a stroke affecting the spinal cord can occur. The MRI can detect areas of reduced blood flow and subsequent damage to the spinal cord tissue.
- Congenital Abnormalities: Structural defects present from birth, such as spina bifida or syringomyelia (the formation of a fluid-filled cyst within the spinal cord), can be clearly visualized.
Nerve Roots: The Pathways to the Body
Branching off from the spinal cord at each vertebral level are the nerve roots, which carry signals to and from specific parts of the body, including the arms, shoulders, and chest. The cervical MRI is excellent at visualizing these delicate structures and identifying any impingement or irritation:
- Herniated Discs: The intervertebral discs, acting as cushions between the vertebrae, can bulge or rupture, extruding their inner material and pressing on nearby nerve roots. This is a common cause of radiculopathy, characterized by pain, numbness, or weakness radiating down the arm. The MRI can show the size and location of the herniation and its direct impact on the nerve root.
- Foraminal Stenosis: The openings through which the nerve roots exit the vertebral canal (foramina) can narrow due to arthritis, bone spurs, or thickened ligaments. This narrowing, or stenosis, can compress the nerve roots, leading to similar symptoms as a herniated disc.
- Tumors: Tumors growing near the nerve roots, such as schwannomas or neurofibromas, can also be detected and characterized.
Intervertebral Discs: The Shock Absorbers
The intervertebral discs are crucial for spinal flexibility and shock absorption. A cervical MRI provides a detailed view of these structures, revealing their health and integrity:
- Degenerative Disc Disease: With age and wear, discs can lose hydration, flatten, and develop tears. The MRI can show these changes, often appearing as discs with decreased signal intensity (indicating dehydration) and reduced height.
- Disc Herniation: As mentioned earlier, disc herniations are a primary finding on cervical MRI. The scan can differentiate between disc bulges (where the disc protrudes but the outer layer remains intact) and true herniations (where the inner material breaches the outer layer).
- Disc Tears: The MRI can identify tears within the annulus fibrosus, the tough outer layer of the disc, which can be a source of neck pain.
Bony Structures and Ligaments: The Spinal Framework
While MRIs are primarily known for soft tissue imaging, they also provide excellent detail of the bony structures of the cervical spine and the surrounding ligaments:
- Vertebrae: The MRI can reveal fractures, dislocations, and alignment issues within the vertebral bodies. It can also show signs of infection (osteomyelitis) or tumors affecting the bone.
- Facet Joints: These small joints between the vertebrae allow for movement and can be affected by arthritis (spondylosis). The MRI can visualize inflammation and cartilage loss in the facet joints.
- Ligaments: The spinal ligaments provide stability to the cervical spine. The MRI can detect tears or inflammation of these ligaments, which can occur after traumatic injuries.
- Bone Marrow: Abnormalities within the bone marrow, such as edema (swelling) due to injury or inflammation, or infiltration by tumors, can also be identified.
Clinical Applications: Diagnosing and Managing Cervical Spine Conditions
The detailed information provided by a cervical MRI translates directly into effective clinical decision-making. Physicians rely on these images to diagnose a wide spectrum of conditions, from common ailments to rare and serious pathologies.
Degenerative Changes and Arthritis
As individuals age, the structures of the cervical spine naturally undergo degenerative changes. This “wear and tear” can lead to conditions like:
- Cervical Spondylosis: This is a general term for age-related wear and tear affecting the spinal discs and joints. MRI is invaluable in identifying the extent of disc degeneration, the formation of bone spurs (osteophytes) that can encroach on the spinal canal and nerve roots, and narrowing of the foramina.
- Osteophytes: These bony outgrowths are a hallmark of arthritis and can significantly contribute to spinal canal stenosis and nerve root compression. The MRI can precisely show their size, location, and impact on surrounding structures.
Traumatic Injuries
The cervical spine is particularly vulnerable to trauma, especially during car accidents, falls, or sports-related incidents. A cervical MRI is crucial in assessing the extent of damage:
- Fractures and Dislocations: While X-rays and CT scans are often the first line of imaging for acute trauma to assess bone integrity, an MRI is vital for evaluating associated soft tissue injuries, such as ligamentous tears, spinal cord contusion (bruising), or hemorrhage (bleeding) within the spinal cord or surrounding tissues. These soft tissue injuries can have significant long-term consequences, even if the bone fracture appears stable on initial imaging.
- Whiplash: This common injury, resulting from sudden forceful extension and flexion of the neck, can cause damage to muscles, ligaments, and discs. MRI can help identify the extent of soft tissue injury and rule out more serious conditions.
Tumors and Infections
While less common, tumors and infections affecting the cervical spine require prompt diagnosis and treatment, and MRI plays a pivotal role:
- Spinal Tumors: Both benign and malignant tumors can arise in the cervical spine. These can originate from the spinal cord itself, the nerve roots, the meninges (the protective membranes surrounding the spinal cord), or spread from other parts of the body (metastasis). MRI’s ability to differentiate between different tissue types and its use of contrast agents are essential for characterizing tumors, determining their extent, and guiding surgical or radiation therapy.
- Spinal Infections (e.g., Discitis, Osteomyelitis, Epidural Abscess): Infections in the cervical spine can be devastating. MRI is highly sensitive in detecting these infections, which often appear as areas of inflammation and fluid collection. Early detection is critical to prevent permanent neurological damage.
Congenital and Other Conditions
Beyond degenerative changes, trauma, and tumors, cervical MRIs can also diagnose other conditions:
- Syringomyelia: As mentioned, this condition involves the formation of a fluid-filled cyst (syrinx) within the spinal cord. MRI is the gold standard for visualizing syrinxes, determining their size and extent, and identifying any underlying causes such as Chiari malformations.
- Arteriovenous Malformations (AVMs) and Vascular Lesions: While specialized vascular imaging techniques like MRA (Magnetic Resonance Angiography) are often used, standard MRI can sometimes reveal abnormalities in the blood vessels supplying the spinal cord.
- Rheumatoid Arthritis and Other Inflammatory Conditions: These conditions can affect the cervical spine, causing inflammation and damage to the facet joints and ligaments. MRI can detect these inflammatory changes.
The MRI Process: What to Expect During a Cervical Scan
Understanding the process of undergoing a cervical MRI can help alleviate patient anxiety and ensure a smoother experience. The procedure itself is non-invasive and painless, though it does require stillness and can sometimes feel claustrophobic.
Preparation and Pre-Scan Procedures
Before the MRI, patients will be screened for any metallic implants or foreign objects that could interfere with the magnetic field or pose a safety risk. This includes pacemakers, cochlear implants, certain types of surgical clips, and shrapnel. Patients will be asked to change into a hospital gown to avoid any clothing with metal components. If contrast dye is to be used, which is common for better visualization of tumors, inflammation, or vascular structures, an intravenous (IV) line will be inserted. Patients are advised to inform the technologist of any allergies, especially to iodine-based contrast agents.
During the Scan: Imaging Techniques and Patient Comfort
Once in the MRI scanner, which is a large, tube-like machine, the patient will be positioned on a comfortable table. For a cervical MRI, the head and neck will be carefully positioned and a special coil, a device that helps improve signal quality, will be placed around the neck. The technologist will then move the table into the scanner.
The MRI scanner produces loud knocking or banging noises as it operates. Patients are usually provided with earplugs or headphones to help mitigate the noise. It is crucial for the patient to remain as still as possible throughout the scan, as any movement can blur the images and reduce their diagnostic quality. The technologist will communicate with the patient through an intercom system and can see them through a camera. The duration of a cervical MRI typically ranges from 30 to 60 minutes, depending on the number of sequences and the complexity of the examination.
Post-Scan Procedures and Results
After the scan is complete, the table will slide out of the scanner, and the IV line, if used, will be removed. Patients are usually free to resume their normal activities immediately. The images are then reviewed by a radiologist, a physician specializing in interpreting medical images. The radiologist will generate a detailed report of their findings, which will be sent to the referring physician. This report, along with the MRI images, will be used by the physician to make a diagnosis and develop an appropriate treatment plan. The time it takes to receive results can vary, but generally, the referring physician will discuss the findings with the patient within a few days to a week.
The Significance of Accurate Imaging in Cervical Spine Management
The insights provided by a cervical MRI are not merely diagnostic; they are fundamental to effective patient care. By offering a detailed, non-invasive view of the cervical spine’s complex anatomy, these scans empower clinicians to make informed decisions, leading to better patient outcomes.
Guiding Treatment Strategies
The precise anatomical information gleaned from a cervical MRI is indispensable for tailoring treatment plans. For instance, knowing the exact size, location, and extent of a herniated disc can help determine whether conservative management (e.g., physical therapy, medication) is appropriate or if surgical intervention is necessary. Similarly, identifying the specific level and degree of spinal cord compression due to bone spurs or other degenerative changes guides decisions about surgical decompression. For tumors, the MRI’s ability to delineate the tumor’s boundaries and its relationship to vital structures is paramount for surgical planning and for determining the effectiveness of oncological treatments.
Monitoring Disease Progression and Treatment Efficacy
In cases of chronic conditions like multiple sclerosis or degenerative disc disease, serial cervical MRIs can be used to monitor disease progression or the effectiveness of treatment interventions. Changes in the size or appearance of lesions, or the degree of spinal canal narrowing, can indicate whether a particular therapy is working or if adjustments are needed. This dynamic assessment capability is a significant advantage of MRI.
Differentiating Between Conditions
The ability of MRI to distinguish between various soft tissues is crucial for differentiating between conditions that may present with similar symptoms. For example, neck pain radiating down the arm could be caused by a herniated disc, a nerve root tumor, or inflammatory changes. The MRI’s detailed visualization helps pinpoint the exact etiology, preventing misdiagnosis and ensuring that the correct treatment is administered. This is particularly important when considering the risks and benefits associated with different therapeutic approaches.
Enhancing Surgical Precision
For neurosurgeons and orthopedic surgeons specializing in spinal surgery, cervical MRI images are like a roadmap. They provide detailed anatomical context, highlighting critical structures such as the spinal cord, nerve roots, and major blood vessels. This allows surgeons to plan their approach with greater precision, minimizing the risk of accidental injury to these vital structures and optimizing the chances of a successful surgical outcome. Intraoperative MRI, where available, can further enhance surgical guidance in real-time.
In conclusion, a cervical MRI is a powerful diagnostic tool that provides a comprehensive and detailed examination of the cervical spine. Its ability to visualize the spinal cord, nerve roots, intervertebral discs, and bony structures in high resolution allows for the accurate diagnosis and effective management of a wide array of conditions. From the everyday discomfort of degenerative changes to the critical urgency of spinal cord compression or tumors, the insights provided by a cervical MRI are essential for guiding treatment, monitoring progress, and ultimately, for preserving the vital function of the cervical spine and the overall health and well-being of patients.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.