The phrase “what does bicep tear feel like”, while seemingly belonging to the realm of physical health, can be surprisingly relevant when we consider the diagnostic processes and tools employed within the Tech industry. In our increasingly data-driven world, understanding the nuances of how symptoms are perceived, recorded, and analyzed is crucial. This article will explore how the experience of a bicep tear, from its initial sensation to its long-term implications, mirrors the challenges and advancements in digital health technologies, diagnostic AI, and user experience in medical applications. We will delve into how technology attempts to bridge the gap between subjective patient experience and objective medical data.
H2: The Subjective Sensation: Translating Pain into Data Points
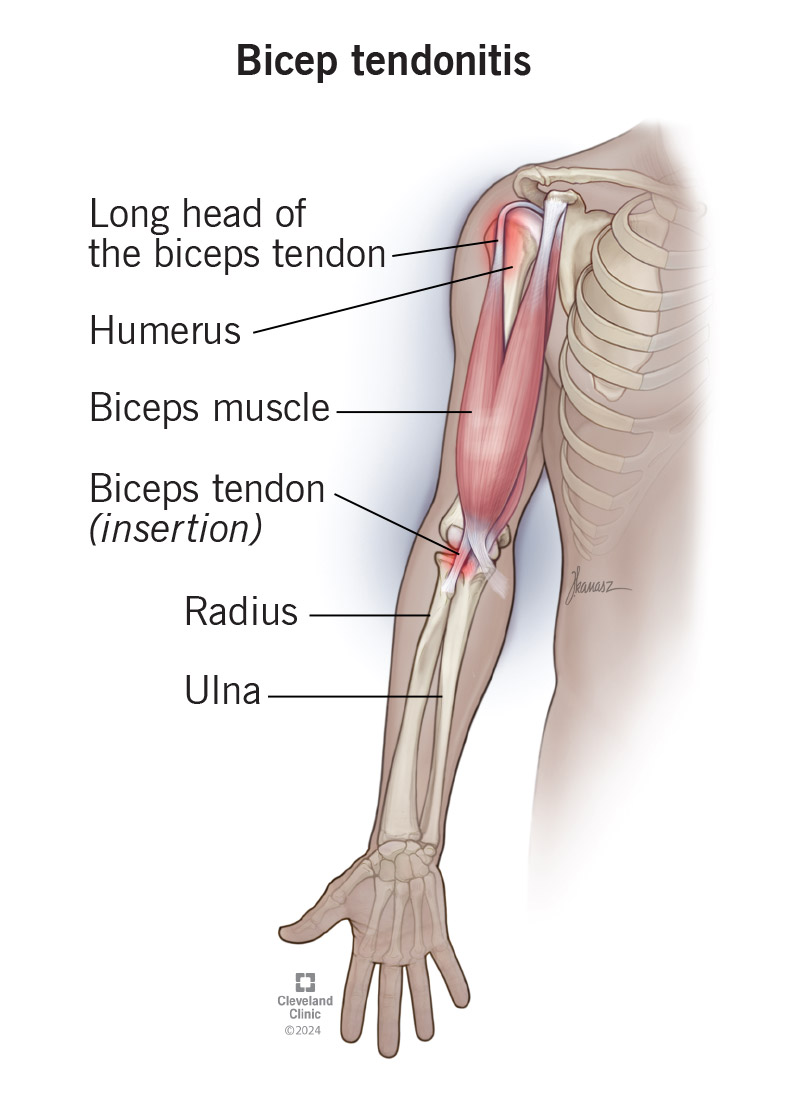
The initial feeling of a bicep tear is deeply personal and subjective. It’s a complex interplay of nerve signals, tissue damage, and psychological response. Translating this visceral, often sudden, experience into quantifiable data is a significant challenge that technology aims to address.
H3: The “Pop” and the Immediate Aftermath
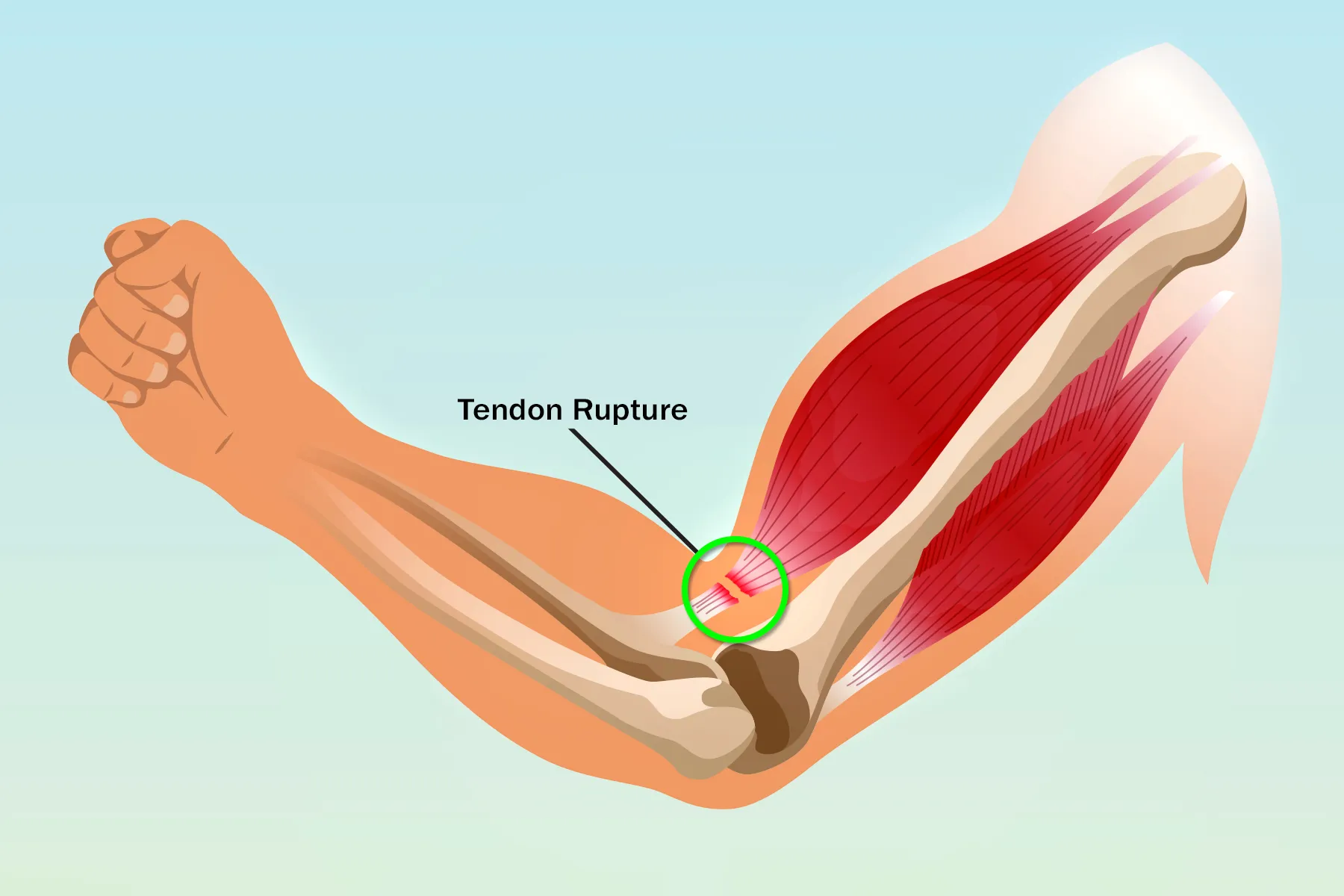
Many individuals describe a distinct “pop” or “snap” sensation at the moment of injury. This is often accompanied by immediate, intense pain. This sensation is not just a feeling; it’s a physiological event. For technology, the challenge lies in capturing the immediacy and intensity of this initial signal. Wearable sensors, for instance, are being developed to detect sudden changes in pressure, muscle tension, and even micro-vibrations that could correlate with such an event. While not directly measuring pain, these devices can provide objective data points that, when combined with user-reported information, create a more comprehensive picture.
The subjective description of pain is notoriously difficult to standardize. Scales like the Visual Analog Scale (VAS) or the Numeric Rating Scale (NRS) are attempts to quantify pain, but they rely on individual interpretation. In the context of technology, this translates to the design of intuitive user interfaces within health apps. How can a user quickly and accurately report the severity of their pain on a scale of 1 to 10? This involves careful consideration of user experience (UX) design, ensuring that the process is not cumbersome, especially for someone in acute discomfort.
H3: The Developing Ache and Functional Impairment
Following the initial acute pain, a bicep tear often develops into a persistent ache, throbbing, or soreness. The affected arm becomes weak, and certain movements, like lifting or even extending the arm, become difficult or impossible. This functional impairment is another crucial data point.
Technology can aid in tracking this functional decline. Motion-tracking sensors, integrated into smartphones or dedicated wearables, can monitor a user’s range of motion and strength. For example, an app could ask a user to perform specific arm movements and then analyze the data to detect limitations compared to their baseline or to normative data. This objective measurement of functional loss complements the subjective reporting of pain and discomfort. Furthermore, AI-powered analysis of gait and movement patterns, while more commonly associated with lower limb injuries, is increasingly being explored for upper body assessment, potentially detecting subtle changes in how an individual uses their arm even in everyday activities.
H2: Diagnostic Technologies: From Patient Report to Digital Insight
The journey from feeling a bicep tear to receiving a diagnosis heavily relies on technological advancements in medical imaging, data analysis, and communication platforms. These technologies aim to augment the physician’s ability to interpret symptoms and confirm the extent of the injury.
H3: The Role of Imaging and AI in Confirmation
While subjective feelings are the initial clue, definitive diagnosis of a bicep tear typically requires medical imaging. Ultrasound and MRI are the primary tools used to visualize the torn tendon or muscle fibers. The interpretation of these images is a complex process that involves specialized training. However, AI is rapidly emerging as a powerful assistant in this domain.
AI algorithms can be trained on vast datasets of medical images to identify patterns indicative of tears, their size, and location. This can help radiologists detect subtle abnormalities that might be missed by the human eye, especially in high-volume settings. Furthermore, AI can automate parts of the image analysis process, potentially speeding up diagnosis and reducing costs. For example, an AI could pre-screen images, highlighting areas of concern for the radiologist to review more closely.
The “feel” of the injury—the subjective experience—is what prompts the patient to seek imaging in the first place. Technology, through patient portals and secure messaging, facilitates the sharing of these subjective descriptions with the medical team, allowing them to correlate the patient’s reported sensations with the objective findings from the imaging.
H3: Wearable Sensors and Remote Monitoring
The evolution of wearable technology is opening new avenues for remote monitoring and data collection related to musculoskeletal injuries. Beyond simple activity tracking, advanced wearables are incorporating sensors that can measure muscle activation, force, and even subtle changes in body temperature that might indicate inflammation.
For someone recovering from a bicep tear, these sensors could provide invaluable data to their healthcare provider. Imagine a patient at home, reporting that their pain is worsening. A wearable sensor could simultaneously transmit data indicating increased muscle tension in the bicep or a change in movement patterns that suggests overexertion. This real-time, objective data stream can help physicians adjust treatment plans more effectively and proactively, rather than relying solely on scheduled appointments and self-reported updates. This is a significant leap from simply describing “what it feels like” to providing continuous, quantifiable physiological feedback.
H2: The Patient Experience in the Digital Age: Apps and Platforms
The way individuals interact with healthcare providers and manage their recovery has been profoundly impacted by technology. Health applications and digital platforms are becoming integral to understanding and addressing conditions like bicep tears.
H3: Mobile Health Apps for Symptom Tracking and Management
Numerous mobile health applications are designed to help users track their symptoms, manage pain, and monitor their recovery progress. These apps often incorporate features for logging pain levels, recording the types of activities that aggravate or alleviate pain, and tracking medication intake. The “feel” of a bicep tear is directly translated into data entries within these apps.
The design of these apps is crucial. They need to be user-friendly, accessible even for individuals experiencing significant discomfort, and offer clear visualizations of their progress. For instance, a graph showing a gradual decrease in reported pain levels over time can be a powerful motivator and provide reassurance. Some advanced apps may even use AI to analyze the logged data and offer personalized advice, such as suggesting specific exercises or recommending rest, based on the user’s reported “feelings” and activity patterns.
H3: Telemedicine and Virtual Consultations
Telemedicine has revolutionized access to healthcare, allowing patients to consult with doctors remotely. For someone experiencing the symptoms of a potential bicep tear, a virtual consultation can be the first step towards diagnosis. During a video call, a physician can observe the patient’s range of motion, ask detailed questions about the sensation and onset of the injury, and guide them on initial self-care measures.
While a virtual consultation cannot replace a physical examination or imaging, it can be highly effective in initial assessments and triage. The patient’s ability to articulate “what it feels like” is paramount in these consultations. Technology, through high-definition video and secure communication channels, facilitates this crucial communication, allowing the physician to gather as much information as possible to determine the next steps, such as recommending an in-person visit or scheduling an ultrasound.
H2: Future Directions: Predictive Analytics and Personalized Recovery
The ongoing advancements in technology promise even more sophisticated ways to understand and manage conditions like bicep tears, moving beyond simply describing the sensation to actively predicting and preventing future issues.
H3: AI-Driven Injury Prediction and Prevention
The dream of truly predictive healthcare is becoming more attainable with the increasing power of AI and the vast amounts of data being collected. By analyzing historical data from individuals with similar profiles and injury histories, AI algorithms could potentially identify individuals at higher risk of developing bicep tears. This might involve looking at factors like occupational demands, exercise routines, past injuries, and even genetic predispositions, all of which can influence how an injury “feels” when it occurs.
Furthermore, as wearable technology becomes more sophisticated, it could monitor physiological markers that precede an injury, such as subtle changes in muscle biomechanics or fatigue patterns. Early detection through AI analysis of this data could lead to proactive interventions, preventing the “pop” and the subsequent pain from ever occurring.
H3: Personalized Rehabilitation Protocols
Once a bicep tear is diagnosed, the recovery process is crucial. Technology is enabling the development of highly personalized rehabilitation protocols. Instead of a generic set of exercises, AI can analyze an individual’s specific tear, their pain tolerance, their rate of healing, and their functional progress to create a dynamic and adaptive rehabilitation plan.
The “feel” of the injury, as reported by the patient and measured by sensors, would be a critical input into this AI-driven system. If a particular exercise consistently causes the patient to report increased pain or shows a negative impact on muscle activation via sensors, the AI can automatically adjust the intensity, duration, or type of exercise. This ensures that the rehabilitation process is optimized for individual recovery, minimizing the risk of re-injury and accelerating the return to full function. The ultimate goal is to move beyond simply understanding “what it feels like” to actively shaping the recovery journey based on a continuous feedback loop of data and intelligent analysis.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.