Non-invasive ventilation (NIV) represents one of the most significant leaps in medical technology over the last four decades. Historically, mechanical ventilation required the insertion of an endotracheal tube—a highly invasive procedure that necessitates sedation and carries risks of infection and lung trauma. However, the emergence of NIV has shifted the paradigm of respiratory care from invasive mechanical intervention to sophisticated, software-driven support that works externally. At its core, NIV is a masterpiece of modern engineering, combining advanced fluid dynamics, real-time sensor processing, and ergonomic hardware design to support patients without the need for surgery.
In the contemporary MedTech landscape, NIV is no longer just a “breathing machine.” It is an integrated digital health platform. Whether utilized in acute clinical settings for respiratory failure or in home environments for chronic conditions like sleep apnea or COPD, the technology behind NIV has become increasingly intelligent, portable, and connected. To understand what non-invasive ventilation is, one must look beyond the mask and explore the complex interplay of hardware and software that keeps millions of people breathing.
The Engineering Architecture of NIV Systems
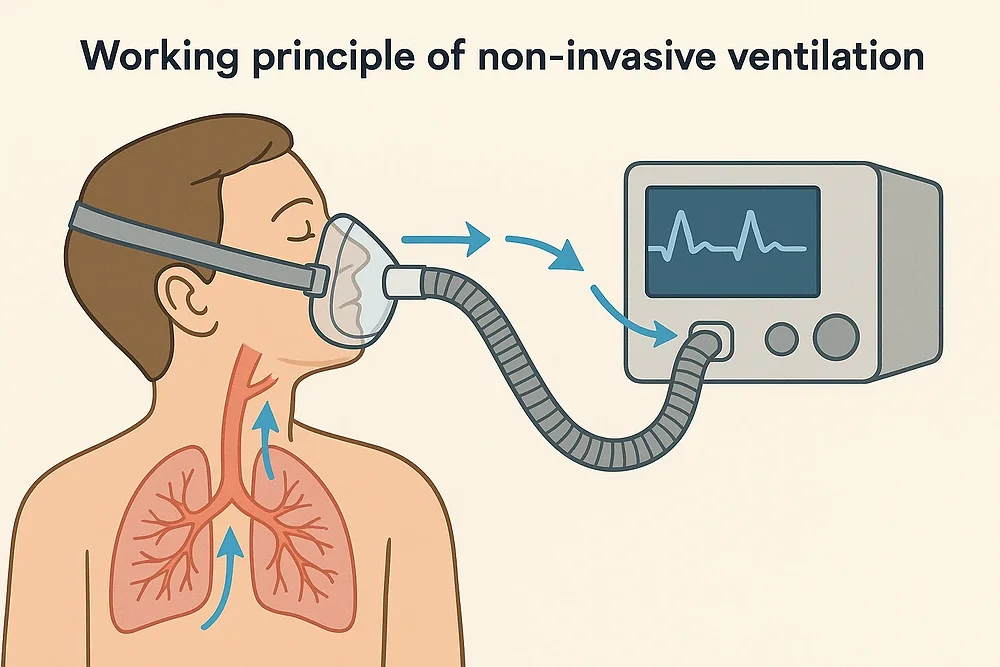
The fundamental objective of any NIV system is to deliver a controlled flow of pressurized air to the lungs through a nasal or oral interface. Unlike simple oxygen therapy, which merely increases the concentration of oxygen, NIV provides “pressure support,” which physically assists the muscles of respiration. This requires a high degree of technical precision in how the machine handles pressure cycles.
Positive Airway Pressure and the Mechanics of Airflow
The technical backbone of NIV is Positive Airway Pressure (PAP). Engineers design these systems to create a pressure gradient that keeps the airways open and reduces the “work of breathing.” There are two primary modalities: Continuous Positive Airway Pressure (CPAP) and Bilevel Positive Airway Pressure (BiPAP).
From a technical standpoint, CPAP provides a constant stream of pressure, acting as a “pneumatic splint.” BiPAP, however, is significantly more complex. It requires the device to oscillate between an Inspiratory Positive Airway Pressure (IPAP) and an Expiratory Positive Airway Pressure (EPAP). This transition must be seamless; if the machine’s sensors do not detect the patient’s intent to inhale within milliseconds, the “asynchrony” can lead to patient discomfort or respiratory distress.
Sensor Integration and Real-Time Triggering
Modern NIV devices are packed with high-sensitivity flow and pressure sensors. These sensors monitor the patient’s breathing pattern at a granular level, often sampling data hundreds of times per second. The “triggering” and “cycling” algorithms are the software brains of the device.
In a tech-heavy NIV unit, the software must distinguish between a patient’s actual breath and a “leak” in the mask. Advanced algorithms use flow-wave analysis to compensate for these leaks in real-time, adjusting the turbine speed to maintain the prescribed pressure. This level of responsiveness is what separates professional-grade MedTech from basic air-moving gadgets.
Hardware Innovation: The Human-Machine Interface
While the internal software manages the air, the external hardware dictates the success of the therapy. In the world of MedTech, “compliance” (the patient actually using the device) is the most critical metric. If the hardware is bulky, loud, or uncomfortable, the technology fails its purpose.
Materials Science in Mask Design
The mask is the primary interface between the machine’s output and the human user. Engineers have turned to advanced materials science to solve the “seal vs. comfort” dilemma. Modern interfaces use liquid silicone or memory foam cushions designed to provide a hermetic seal without causing pressure sores.
Furthermore, the “exhaust ports” or vents in these masks are precision-engineered. They must allow for the “washout” of CO2 so the patient doesn’t re-breathe their own waste gas, but they must do so silently. This involves complex acoustic engineering to minimize the sound of rushing air, ensuring the device can be used during sleep without disturbing the user or their partner.
Turbine Technology and Miniaturization
A decade ago, NIV machines were large, noisy units confined to hospital carts. Today, the “blower” or turbine technology has undergone massive miniaturization. High-speed, brushless DC motors can now spin at upwards of 30,000 RPM while remaining virtually silent.
These turbines are designed for extreme durability and responsiveness. They must be able to ramp up speed instantly to meet an inspiratory demand and decelerate just as quickly during exhalation. This mechanical agility is supported by sophisticated power management systems, allowing portable NIV units to run on lithium-ion batteries for several hours, providing mobility to patients who were previously tethered to a wall outlet.
The Digital Transformation: AI, Cloud, and Connectivity
The most significant trend in NIV technology today is the integration of Digital Health and the Internet of Medical Things (IoMT). NIV devices are no longer standalone tools; they are data-generating nodes in a global healthcare network.
Remote Patient Monitoring (RPM) and Data Telemetry
Most modern NIV and CPAP devices come equipped with cellular or Wi-Fi connectivity. Every breath the patient takes is recorded, analyzed, and uploaded to a cloud-based server. For healthcare providers, this is a revolutionary shift.
Instead of waiting for a follow-up appointment, a doctor can log into a dashboard to see a patient’s “AHI” (Apnea-Hypopnea Index), leak rates, and usage hours in real-time. This data telemetry allows for proactive intervention. If the software detects a sudden change in breathing patterns—which could indicate a worsening of a chronic condition—it can trigger an alert for the clinical team to adjust the machine’s settings remotely.
AI-Driven Auto-Titration
Artificial Intelligence is now being used to manage the delivery of pressure. “Auto-titrating” NIV devices use machine learning algorithms to analyze the patient’s upper airway stability on a breath-by-breath basis.
If the algorithm detects a partial collapse of the airway, it automatically increments the pressure to the minimum level required to resolve the obstruction. This “intelligent” approach ensures the patient receives the most effective therapy with the least amount of pressure, significantly increasing comfort. These AI models are trained on millions of nights of sleep data, making them incredibly proficient at identifying different types of respiratory events (such as obstructive vs. central apneas) that require different technical responses.
Future Frontiers in NIV Technology
As we look toward the future of MedTech, the trajectory of non-invasive ventilation is moving toward even greater personalization and integration with other wearable technologies.
Wearable Integration and Biofeedback
The next generation of NIV systems will likely be “aware” of the patient’s overall physiological state. By syncing with smartwatches or chest straps that monitor heart rate, blood oxygen levels (SpO2), and even sleep stages, the NIV device can adjust its performance based on the body’s total demand. For instance, if a wearable detects a drop in blood oxygen, the NIV unit could theoretically increase its pressure support to compensate before the patient even realizes they are struggling.
Overcoming the Interoperability Challenge
One of the major hurdles in the MedTech space is interoperability—the ability of different devices and platforms to share data seamlessly. Future NIV innovations are focusing on open API structures that allow respiratory data to flow directly into Electronic Health Records (EHRs).
This tech-forward approach ensures that a patient’s respiratory data isn’t siloed in a proprietary app but is instead a core part of their comprehensive medical profile. As 5G technology becomes more ubiquitous, the latency in remote monitoring will vanish, potentially allowing for real-time remote “ventilation-as-a-service” where respiratory therapists can adjust settings from across the world as if they were standing at the bedside.

Conclusion
Non-invasive ventilation is a quintessential example of how technology can transform human life. By moving away from the “iron lung” models of the past and embracing high-speed processing, smart materials, and cloud-based analytics, NIV has become a cornerstone of modern medicine. It is a field where software engineering meets human biology, creating a life-sustaining harmony through the power of pressurized air and intelligent data. As AI and connectivity continue to evolve, the “what” of non-invasive ventilation will continue to expand, moving from a reactive medical tool to a proactive, personalized health companion.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.