The healthcare industry, a cornerstone of modern society, relies on a complex and intricate system of operations to function effectively. At the heart of this operational efficiency lies the critical role of medical billing and coding. These professionals are the bridge between patient care and financial reimbursement, translating medical services into standardized codes that facilitate insurance claims and ensure healthcare providers are compensated for their work. Consequently, understanding the salary landscape for these vital roles is of significant interest to individuals considering a career in this field, as well as for healthcare organizations looking to attract and retain talent. This article delves into the financial aspects of medical billing and coding, exploring the factors that influence earning potential and providing insights into salary expectations.
Understanding the Core Functions and Their Financial Impact
Medical billing and coding professionals are indispensable to the financial health of any healthcare organization. Their work directly impacts revenue cycles, claim accuracy, and regulatory compliance. The specialized knowledge and skills they possess are in high demand, and their compensation reflects this importance.
The Role of Medical Coders: Translating Healthcare Into Data
Medical coders are the architects of the financial narrative of patient encounters. They meticulously review patient medical records, including physician’s notes, diagnostic reports, and treatment plans, to assign standardized alphanumeric codes. These codes, governed by systems like the International Classification of Diseases (ICD) and Current Procedural Terminology (CPT), are crucial for several reasons:
- Reimbursement: Insurance companies and government payers (like Medicare and Medicaid) use these codes to determine the amount they will reimburse healthcare providers for services rendered. Accurate coding is paramount to ensure appropriate payment.
- Data Analysis: Coded data provides valuable insights into disease prevalence, treatment patterns, and healthcare utilization. This information is essential for public health initiatives, research, and quality improvement efforts.
- Compliance: Strict adherence to coding guidelines and regulations is vital for avoiding audits, penalties, and fraud accusations. Coders must stay abreast of constantly evolving coding rules and payer policies.
The complexity of medical terminology, anatomy, physiology, and diagnostic procedures demands a high level of expertise. Coders often specialize in specific areas, such as inpatient coding, outpatient coding, or specialized fields like oncology or cardiology, which can further enhance their earning potential.
The Role of Medical Billers: Navigating the Reimbursement Process
Medical billers work in tandem with coders to ensure that healthcare providers receive payment for their services. Once medical services are coded, billers take over the process of creating and submitting claims to insurance companies. Their responsibilities include:
- Claim Submission: Billers prepare and submit accurate insurance claims, ensuring all necessary information, such as patient demographics, insurance details, and medical codes, is correctly entered.
- Payment Posting: They track the status of submitted claims, post payments received from insurance companies, and identify any discrepancies or denials.
- Denial Management: A significant part of a biller’s role involves investigating and appealing denied claims. This requires understanding insurance policies, identifying the reasons for denial, and taking appropriate corrective actions to resubmit claims.
- Patient Billing: For services not covered by insurance or for co-pays and deductibles, billers may also handle the communication and collection of payments directly from patients.
- Revenue Cycle Management: Billers are integral to the broader revenue cycle management process, aiming to optimize the flow of revenue from patient service to final payment.
The skills required for medical billing extend beyond data entry; they involve strong communication, problem-solving, and analytical abilities, as well as a thorough understanding of insurance regulations and payer contracts.
Factors Influencing Billing and Coding Salaries
The salary for medical billing and coding professionals is not a fixed figure. It is influenced by a multitude of factors, ranging from individual qualifications and experience to the specific work environment and geographic location. Understanding these variables is crucial for setting realistic salary expectations and for strategizing career advancement.
Experience and Expertise: The Foundation of Earning Potential
As with most professions, experience plays a significant role in determining a medical billing and coding salary. Entry-level positions typically command lower salaries, while seasoned professionals with a proven track record of accuracy and efficiency can negotiate higher compensation.
- Entry-Level: Individuals new to the field, perhaps having recently completed a certification program, might start in roles such as billing assistant or junior coder. Their salaries will reflect the need for on-the-job training and supervision.
- Mid-Level: With a few years of experience, professionals can advance to positions with more responsibility, such as certified medical coder or billing specialist. They are expected to work more independently and handle a wider range of tasks.
- Senior-Level/Specialized Roles: Experienced professionals who have developed expertise in specific areas, such as auditing, compliance, or specialized coding (e.g., surgical coding, oncology coding), can command substantially higher salaries. Lead coder, billing supervisor, or compliance officer roles often come with increased responsibility and, therefore, higher pay.
The acquisition of specialized certifications is a powerful way to demonstrate expertise and can significantly boost earning potential. Certifications from reputable organizations like the AAPC (American Academy of Professional Coders) or AHIMA (American Health Information Management Association) are highly valued by employers.
Certifications and Education: Demonstrating Proficiency and Knowledge
The educational background and professional certifications held by billing and coding professionals are critical determinants of their salary. While a high school diploma or GED is often the minimum requirement, formal education and specialized training can lead to better job opportunities and higher pay.
- Certificate Programs: Many community colleges and vocational schools offer certificate programs in medical billing and coding. These programs typically provide comprehensive training in coding systems, medical terminology, and billing procedures. Graduates of these programs are generally well-prepared for entry-level positions.
- Associate’s or Bachelor’s Degrees: Some employers prefer candidates with an associate’s or even a bachelor’s degree in health information management or a related field. These degrees provide a more in-depth understanding of healthcare systems, data management, and regulatory compliance.
- Professional Certifications: The most impactful factor in salary potential for billing and coding professionals is often their certification. Key certifications include:
- Certified Professional Coder (CPC) from AAPC: This is one of the most widely recognized and sought-after certifications for outpatient coders.
- Certified Coding Specialist (CCS) from AHIMA: This certification is highly respected for inpatient coding.
- Certified Outpatient Coder (COC) from AAPC: Focuses on outpatient facility coding.
- Certified Professional Biller (CPB) from AAPC: Specifically for billing professionals.
Holding one or more of these certifications not only validates a professional’s skills but also signals to employers a commitment to the profession and a higher level of competency, often translating directly into a more competitive salary. Continuing education and maintaining certifications through professional development are essential for staying current and for maximizing long-term earning potential.

Work Setting and Industry: Diverse Environments, Diverse Pay
The specific healthcare setting where a medical biller or coder works can have a notable impact on their salary. Different environments have varying revenue models, patient volumes, and reimbursement complexities, which influence compensation.
- Hospitals: Large hospital systems often have complex billing and coding departments. Coders and billers in hospitals may specialize in inpatient or outpatient services, with inpatient coding often requiring a deeper understanding of complex medical conditions and procedures, potentially leading to higher salaries.
- Physician Offices and Clinics: Smaller physician practices and clinics generally have more streamlined billing and coding operations. Salaries in these settings might be slightly lower compared to large hospital systems but can offer a more integrated role within a smaller team.
- Third-Party Billing Companies: These companies specialize in providing billing and coding services to multiple healthcare providers. They often employ a large number of professionals and may offer competitive salaries due to their efficiency and focus on revenue optimization.
- Government Agencies and Insurance Companies: Roles within government health programs (e.g., Medicare, Medicaid) or private insurance companies that involve claims review, auditing, or policy development can also offer attractive salary ranges, often with benefits packages that reflect the stability of these organizations.
- Urgent Care Centers and Ambulatory Surgery Centers: These facilities have specific coding needs related to their service offerings, and the demand for skilled professionals in these niche areas can lead to competitive compensation.
The complexity of the services provided, the payer mix (e.g., a high proportion of private insurance vs. government payers), and the administrative structure of the organization all contribute to the salary offered for billing and coding positions.
Geographic Location: The Cost of Living and Market Demand
Location is a perennial factor influencing salary across all professions, and medical billing and coding is no exception. The cost of living in a particular metropolitan area or region, coupled with the demand for skilled professionals in that market, directly affects earning potential.
- High Cost of Living Areas: Major metropolitan areas with a high cost of living, such as New York City, Los Angeles, or San Francisco, typically offer higher salaries for medical billing and coding professionals to offset the increased expenses for employees.
- Areas with High Healthcare Demand: Regions with a robust healthcare infrastructure, a large population base, and a high volume of medical services being rendered often experience a greater demand for skilled billing and coding staff. This demand can drive up salaries as employers compete for talent.
- Rural vs. Urban: Generally, urban areas tend to offer higher salaries than rural areas. However, in some rural areas with a shortage of healthcare professionals, specialized skills might command a premium.
- Remote Work Opportunities: The rise of remote work has also introduced new dynamics. While remote positions can offer flexibility and access to jobs nationwide, salaries might be benchmarked against regional averages or national averages, depending on the employer’s compensation strategy.
It is essential for individuals to research salary benchmarks for their specific location and experience level to understand their earning potential accurately. Resources like the Bureau of Labor Statistics, professional association salary surveys, and online job boards can provide valuable insights into regional salary variations.
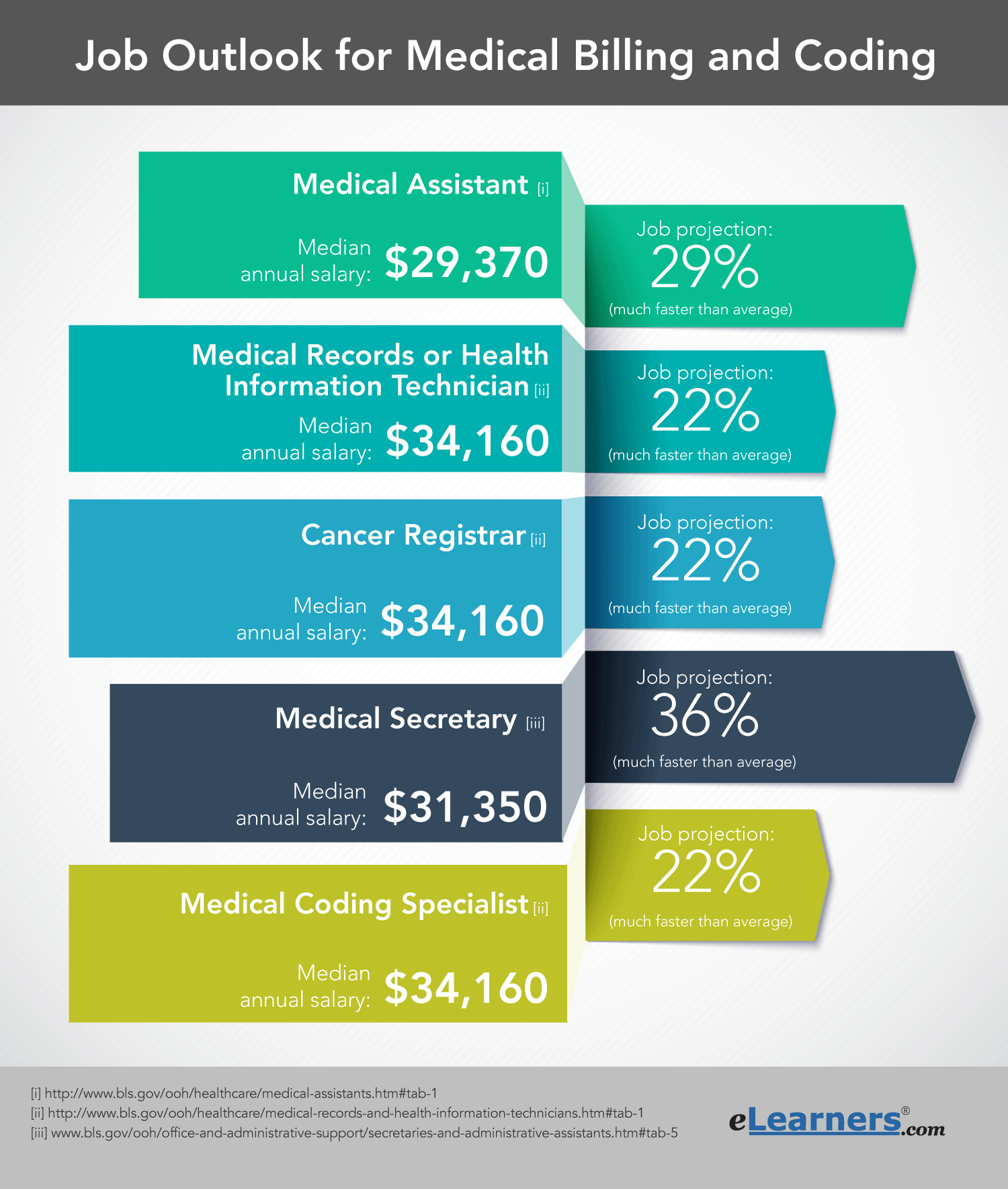
Career Outlook and Salary Projections
The outlook for medical billing and coding professionals remains strong, driven by the continued growth of the healthcare industry and the increasing complexity of healthcare regulations and reimbursement models. As the demand for healthcare services expands, so does the need for professionals who can efficiently and accurately manage the financial aspects of patient care.
Growth in the Healthcare Sector
The healthcare industry is projected to continue its robust growth trajectory. Factors such as an aging population, advancements in medical technology, and increased access to healthcare services contribute to a consistent need for medical professionals, including those in administrative and financial support roles. This sustained growth directly translates into ongoing demand for skilled medical billers and coders.
Increasing Complexity of Regulations and Reimbursement
Healthcare regulations, particularly those related to billing and coding, are constantly evolving. Changes in payer policies, the implementation of new coding systems, and a greater emphasis on data accuracy and compliance require professionals to possess up-to-date knowledge and specialized skills. This complexity often necessitates the employment of dedicated billing and coding experts, rather than relying on general administrative staff. The intricacies of navigating Medicare, Medicaid, and private insurance plans require a deep understanding that certified professionals possess.
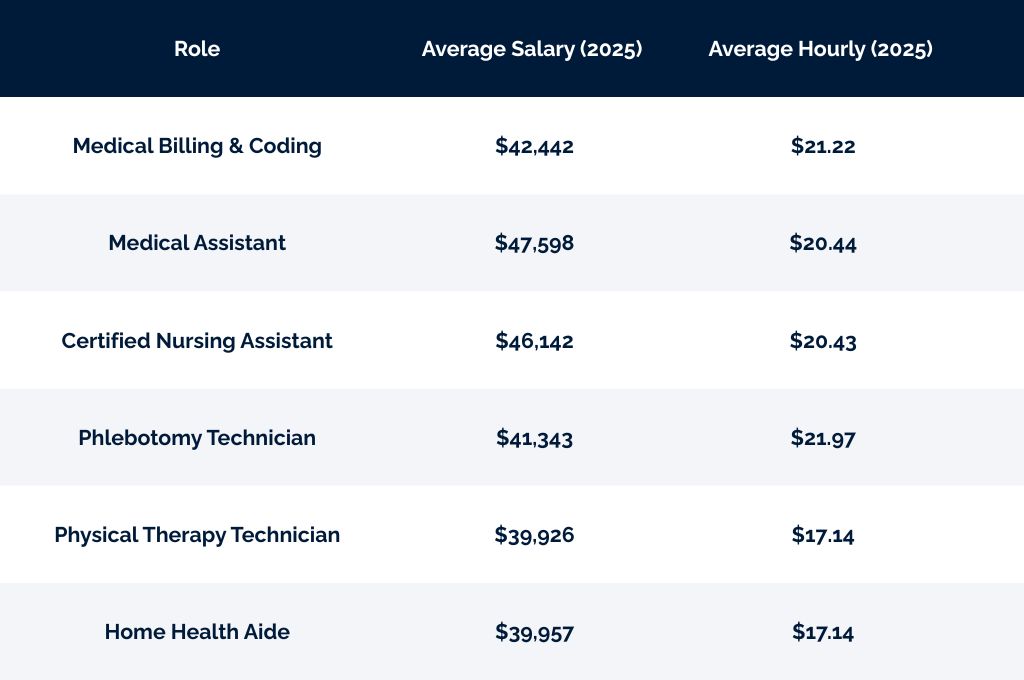
Salary Trends and Future Expectations
While precise salary figures can vary widely, national averages for medical billers and coders generally fall within a competitive range, often starting from the mid-$30,000s for entry-level positions and rising to $50,000 to $70,000 or more for experienced and certified professionals, particularly those in specialized roles or leadership positions. Some highly specialized coders or auditors in high-demand areas or with extensive experience can earn six-figure salaries.
The future of billing and coding salaries is likely to see continued upward pressure due to:
- Demand for Specialization: As the healthcare landscape becomes more fragmented, with an increasing number of specialized medical fields, there will be a growing demand for coders with expertise in specific areas like cardiology, oncology, or behavioral health.
- Technological Integration: While technology is automating some aspects of billing and coding, it also creates a need for professionals who can manage and interpret the data generated by these systems, as well as oversee the accuracy of automated processes. This may lead to new roles focused on revenue cycle technology management.
- Auditing and Compliance: With increased scrutiny from government agencies and payers, the demand for skilled auditors and compliance specialists in billing and coding will remain high.
For individuals considering a career in medical billing and coding, the prospect of a stable and financially rewarding career path is promising. Continuous professional development, pursuit of relevant certifications, and strategic career planning are key to maximizing earning potential and ensuring long-term success in this dynamic and essential field.
Conclusion: A Rewarding Career Path in Healthcare Finance
Medical billing and coding professionals occupy a crucial intersection of healthcare delivery and financial management. Their expertise ensures that healthcare providers can operate effectively, receive fair compensation for their services, and that accurate data is collected for various analytical and public health purposes. The salary for these roles is a reflection of the specialized knowledge, meticulous attention to detail, and the ever-evolving landscape of healthcare regulations they must navigate.
Factors such as experience, the attainment of industry-recognized certifications, the specific work environment, and geographic location all play significant roles in determining earning potential. As the healthcare industry continues to grow and evolve, the demand for skilled medical billers and coders is projected to remain strong, offering a stable and rewarding career path. By understanding the factors that influence their salaries and by committing to continuous professional development, individuals entering or advancing within this field can position themselves for financial success and make a valuable contribution to the healthcare system.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.