Managing a chronic condition like Type 2 Diabetes often involves a complex interplay of medical care, lifestyle adjustments, and, critically, ongoing medication. For many, Trulicity (dulaglutide) is a cornerstone of their treatment regimen, offering significant benefits in blood sugar control and cardiovascular risk reduction. However, the efficacy of such vital medications is frequently overshadowed by the daunting question of cost, particularly in healthcare systems where prescription prices can be astronomically high. Patients are increasingly looking for tools and strategies to mitigate these expenses, and platforms like GoodRx have emerged as essential resources. This article delves into the financial realities of obtaining Trulicity, specifically examining how GoodRx can offer a lifeline to patients, and explores broader strategies for managing the significant financial burden of diabetes medication.
Understanding Trulicity: A Critical Medication for Type 2 Diabetes
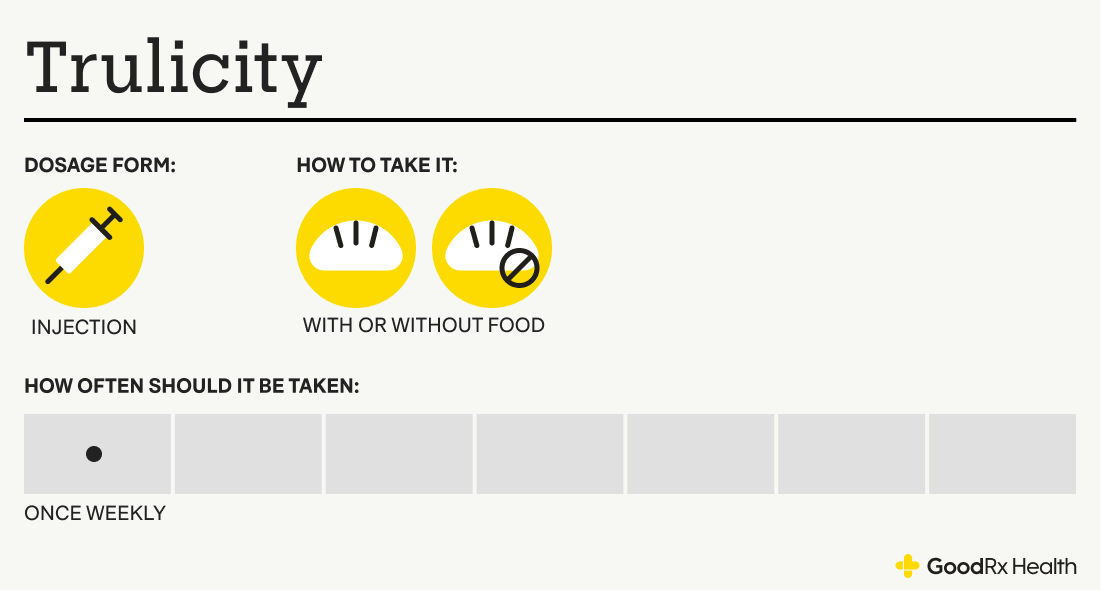
Trulicity is a glucagon-like peptide-1 (GLP-1) receptor agonist, prescribed primarily for adults with Type 2 Diabetes to improve glycemic control. It works by mimicking the natural hormone GLP-1, which helps the body release insulin in response to high blood sugar, decreases glucose production by the liver, and slows stomach emptying, promoting a feeling of fullness. Beyond its glucose-lowering effects, clinical trials have also demonstrated Trulicity’s ability to reduce the risk of major cardiovascular events in adults with Type 2 Diabetes and established cardiovascular disease or multiple cardiovascular risk factors. Administered as a once-weekly injectable, its convenience further enhances adherence for many patients.
The profound benefits of Trulicity in managing a progressive and potentially debilitating disease make it an invaluable part of modern diabetes care. However, its sophisticated mechanism of action and the research and development involved in bringing such an innovative drug to market contribute to its premium pricing. For patients, this often means confronting monthly costs that can stretch personal budgets to their breaking point, potentially leading to difficult choices between medication adherence and other essential living expenses. This financial strain is not merely an inconvenience; it can directly impact health outcomes if patients skip doses, split pills, or abandon treatment altogether due to affordability issues. The growing financial burden of chronic disease management necessitates a proactive approach to understanding and leveraging available cost-saving measures.
The High Cost of Prescription Medications in the U.S.
The United States has some of the highest prescription drug prices globally, a reality that deeply impacts millions of Americans. While innovative medications like Trulicity offer life-changing benefits, their price tags can be staggering. Before discounts or insurance, a single month’s supply of Trulicity can often range from $800 to over $1,200. This steep cost is a multifaceted issue driven by several interconnected factors.
One primary factor is the robust patent system, which grants pharmaceutical companies exclusive rights to market a drug for a specific period, allowing them to set prices without direct competition. The high costs of research and development (R&D) are frequently cited as justifications, with companies investing billions to bring a new drug from concept to market, enduring numerous failures along the way. Additionally, the U.S. healthcare system lacks centralized price negotiation for prescription drugs, unlike many other developed nations. This allows pharmaceutical manufacturers significant leeway in setting list prices. The complex role of pharmacy benefit managers (PBMs) – intermediaries that negotiate drug prices between manufacturers, pharmacies, and insurance companies – also contributes to the opacity and inflation of drug costs, with rebates and fees often complicating the true net price.
The impact of these high drug prices on patient adherence and financial well-being is profound. Patients with chronic conditions like Type 2 Diabetes often face a lifetime of medication expenses. When faced with exorbitant out-of-pocket costs, many are forced to make difficult decisions. Some may ration their medication, taking less than prescribed or skipping doses, which can lead to poorer health outcomes, hospitalizations, and increased healthcare costs in the long run. Others may accrue significant medical debt, impacting their credit scores, limiting their financial freedom, and adding immense stress to their lives. The financial toxicity of prescription drugs is a recognized public health crisis, compelling patients to seek out every possible avenue for savings, with tools like GoodRx becoming indispensable for financial survival in the current healthcare landscape.
GoodRx: A Powerful Tool for Prescription Savings
In an environment where prescription drug prices can vary wildly even within the same zip code, GoodRx has emerged as a critical financial tool for consumers seeking to reduce their healthcare expenditures. GoodRx is a digital platform that aggregates drug prices and discounts from thousands of pharmacies across the United States, providing a comparative shopping experience for medications. Its fundamental value proposition lies in its ability to offer transparency and access to lower prices that might otherwise be unavailable or unknown to the average patient.
The mechanism behind GoodRx’s effectiveness is relatively straightforward yet powerful. The platform collects current prices and discounts (including manufacturer coupons, pharmacy coupons, and PBM negotiated rates) from virtually all U.S. pharmacies, including major chains like CVS, Walgreens, Rite Aid, and independent pharmacies. When a user searches for a medication, GoodRx instantly displays the prices at various local pharmacies and provides free discount coupons. These coupons can be used by anyone, regardless of insurance status, and often offer prices lower than an individual’s insurance co-pay, especially for high-deductible plans or medications not covered by their formulary. By presenting these options side-by-side, GoodRx empowers consumers to choose the most affordable option, transforming what was once an opaque pricing landscape into a navigable marketplace.
For a medication like Trulicity, using GoodRx can result in substantial savings. While Trulicity typically remains expensive due to its brand-name status and lack of generic alternatives, GoodRx can significantly reduce its cash price. A step-by-step approach to using GoodRx for Trulicity involves simply visiting the GoodRx website or using its mobile app, typing “Trulicity” into the search bar, and entering your zip code. The platform will then display a list of pharmacies in your area, along with their prices for Trulicity using GoodRx coupons. Patients can select the best price, print or electronically send the coupon to their phone, and present it to the pharmacist when filling their prescription. It’s crucial to compare the GoodRx price with your insurance co-pay, as the GoodRx coupon often provides a better deal, particularly if you have not met your deductible.
While GoodRx offers considerable advantages, it’s also important to understand its business model and limitations. GoodRx makes money primarily through advertising and referral fees from PBMs and pharmacies when users fill prescriptions using their discounts. This model allows GoodRx to provide its services to consumers for free. A limitation is that GoodRx coupons cannot be combined with insurance; it’s an either/or situation. Furthermore, while GoodRx can significantly lower costs, it may not make extremely expensive medications like Trulicity “cheap” in absolute terms. For those with extremely high costs, GoodRx serves as a vital first line of defense, but it often needs to be complemented by other financial strategies.
Strategies Beyond GoodRx for Managing Trulicity Costs
While GoodRx is an excellent starting point for reducing the cost of Trulicity, it’s just one tool in a comprehensive financial toolkit for managing prescription expenses. Patients facing high out-of-pocket costs for Trulicity should explore several other avenues to ensure affordability and adherence.
One of the most effective strategies involves manufacturer savings programs and patient assistance programs (PAPs). Eli Lilly, the manufacturer of Trulicity, often offers programs designed to help patients afford their medication. These programs can include co-pay cards, which significantly reduce the out-of-pocket cost for commercially insured patients, and PAPs, which provide free or low-cost medication to eligible uninsured or underinsured individuals. Eligibility for PAPs is typically based on income and insurance status. It is advisable to visit the manufacturer’s official website or speak with a healthcare provider or pharmacist for details on current programs and application processes.
Navigating insurance coverage and formulary limitations is another critical step. Patients should thoroughly understand their health insurance plan’s formulary (the list of covered drugs) and how Trulicity is classified within it. Some plans may require prior authorization or step therapy before covering Trulicity, while others may place it in a higher tier with greater co-pay requirements. If Trulicity is not covered or is too expensive, patients should discuss appealing the insurance decision with their doctor or exploring whether a therapeutic alternative is covered more favorably. While Trulicity has specific benefits, sometimes a similar medication in the same class (another GLP-1 agonist) might be on a lower tier on the formulary, offering a cost-effective alternative in consultation with a physician.
Additionally, exploring alternative medications and generics, when applicable, can lead to substantial savings. While Trulicity currently does not have a generic equivalent, discussing with your doctor whether other GLP-1 agonists or different classes of diabetes medications could be appropriate for your condition is worthwhile. Sometimes, an older, equally effective drug with a generic version might be suitable, drastically reducing costs. However, any change in medication must be a collaborative decision with your healthcare provider, weighing efficacy, side effects, and cost.
Finally, leveraging health savings accounts (HSAs) and flexible spending accounts (FSAs) can provide tax-advantaged ways to pay for Trulicity and other qualified medical expenses. HSAs are available to those with high-deductible health plans and allow pre-tax contributions to be used for healthcare costs, growing tax-free and tax-free withdrawals for medical expenses. FSAs, offered through employers, allow employees to set aside pre-tax money for healthcare costs within a plan year. Utilizing these accounts effectively can reduce the overall financial impact of prescription drug costs by saving on taxes.
Empowering Patients: Taking Control of Your Healthcare Finances
The journey to effectively manage Trulicity costs, or any high-priced medication, is ultimately about empowerment. It requires patients to be proactive, informed, and willing to advocate for their financial well-being within the complex healthcare system. Taking control of your healthcare finances involves a combination of smart shopping, understanding your benefits, and open communication with your medical team.
Advocating for yourself with healthcare providers is paramount. Many physicians are aware of drug costs but may not always proactively discuss them. Patients should feel comfortable initiating conversations about medication affordability, asking if less expensive alternatives exist, or if manufacturer programs could help. A doctor can often help navigate prior authorizations or provide necessary documentation for patient assistance programs. Building a trusting relationship with your healthcare team that includes financial transparency can lead to better outcomes, both medically and financially.
Furthermore, the importance of financial literacy in healthcare cannot be overstated. Understanding your insurance policy, knowing what a formulary is, how deductibles and co-pays work, and the difference between brand-name and generic drugs are fundamental. Resources like GoodRx, the manufacturer’s websites, and even patient advocacy groups offer a wealth of information that can demystify healthcare billing and pricing. Long-term financial planning for chronic conditions should also be considered, perhaps incorporating expected medication costs into an annual budget and exploring financial counseling if medical debt becomes unmanageable.
In conclusion, while the question “how much is Trulicity with GoodRx?” often signifies a starting point for cost concerns, the answer reveals a broader landscape of financial navigation. GoodRx provides a vital immediate discount, but a holistic approach combining manufacturer programs, insurance savvy, physician collaboration, and financial planning offers the most robust strategy for managing the significant costs associated with essential medications like Trulicity. By actively engaging with these tools and strategies, patients can mitigate financial stress and ensure consistent access to the treatment they need for a healthier future.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.