The intersection of human biology and advanced engineering has produced some of the most significant breakthroughs in modern history. Among these, the “Fontan” stands out not merely as a medical procedure, but as a masterpiece of physiological re-engineering. For those operating within the spheres of MedTech, biotechnology, and digital health, understanding the Fontan circulation is essential. It represents a pivot from traditional “repair” to high-level “systemic optimization,” utilizing computational modeling, advanced materials, and data-driven monitoring to sustain life in patients born with complex heart defects.
At its core, a Fontan is the final stage of a multi-step surgical intervention for children born with single-ventricle heart defects. However, in the modern tech landscape, the Fontan is increasingly defined by the technology used to plan, execute, and monitor it. This article explores the Fontan through the lens of medical technology, examining how digital twins, surgical robotics, and wearable sensors are transforming a high-risk procedure into a manageable lifelong journey.
The Engineering Marvel of the Fontan Circulation
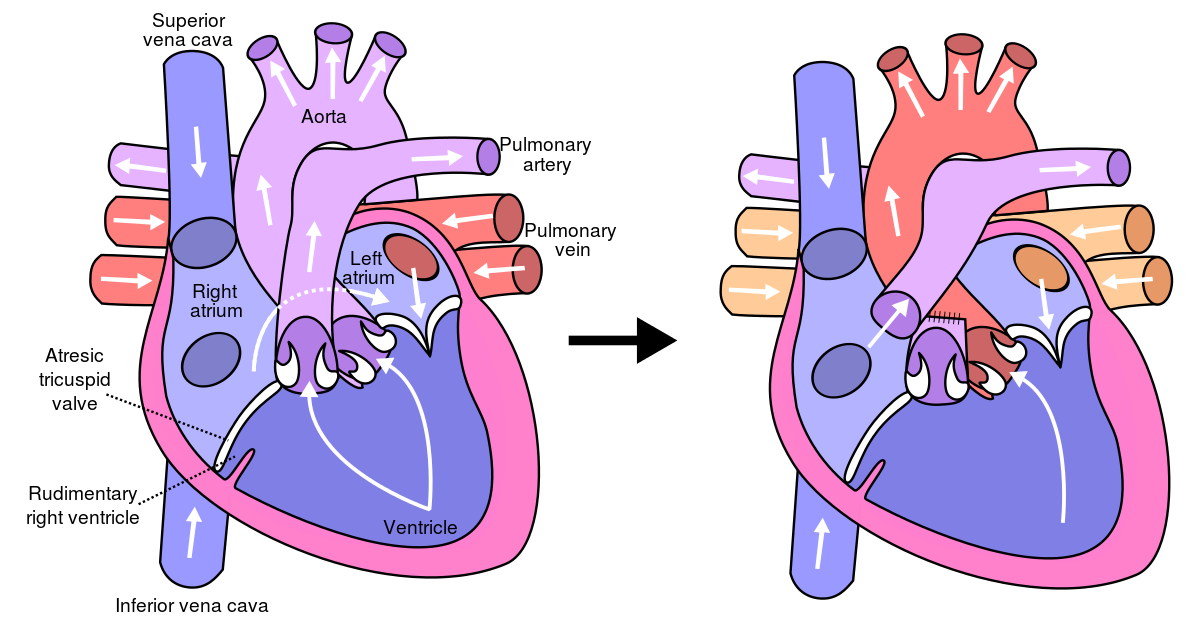
To understand the Fontan, one must first understand the mechanical “glitch” it aims to solve. In a standard human heart, there are two pumps: one for the lungs and one for the body. Some infants are born with only one functional pump (ventricle). Without intervention, the system fails due to oxygen deprivation and volume overload. The Fontan procedure is a bio-engineering workaround that reroutes the circulatory “plumbing” so that blood flows to the lungs passively, without a dedicated pump.
Understanding the Single Ventricle Challenge
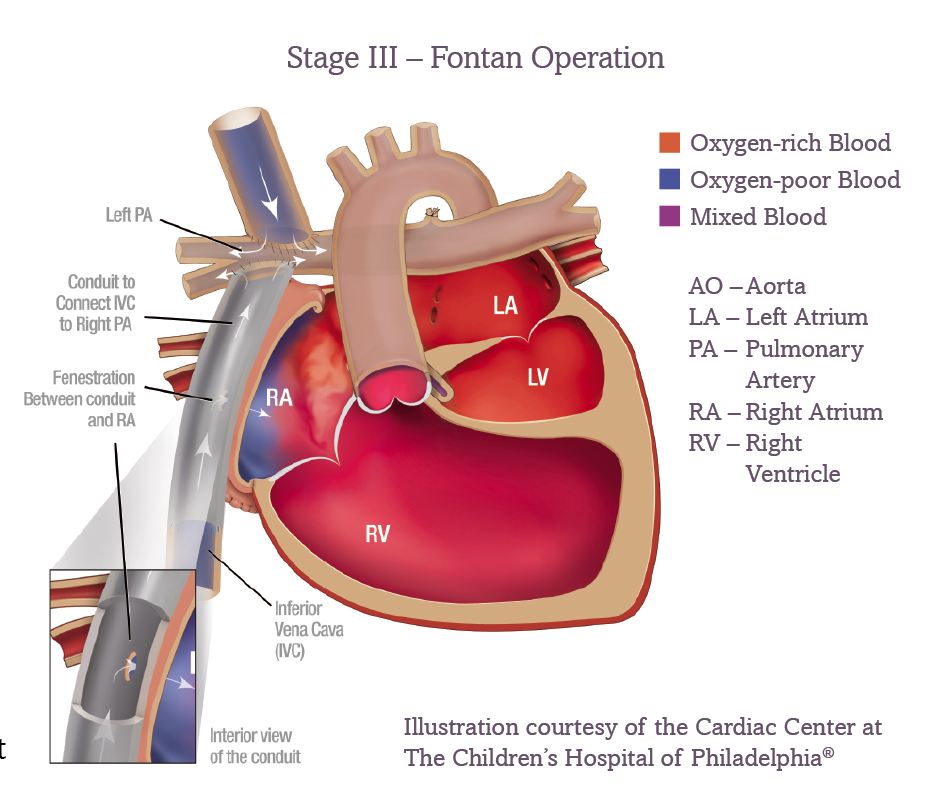
From a systems architecture perspective, a single-ventricle heart is an inefficient circuit. The Fontan procedure seeks to reorganize this architecture. By connecting the inferior vena cava directly to the pulmonary artery, surgeons create a “Total Cavopulmonary Connection” (TCPC). This allows the single functional ventricle to focus exclusively on pumping oxygenated blood to the rest of the body, while the lungs receive blood via pressure gradients rather than active pulses.
The Technological Evolution of the TCPC
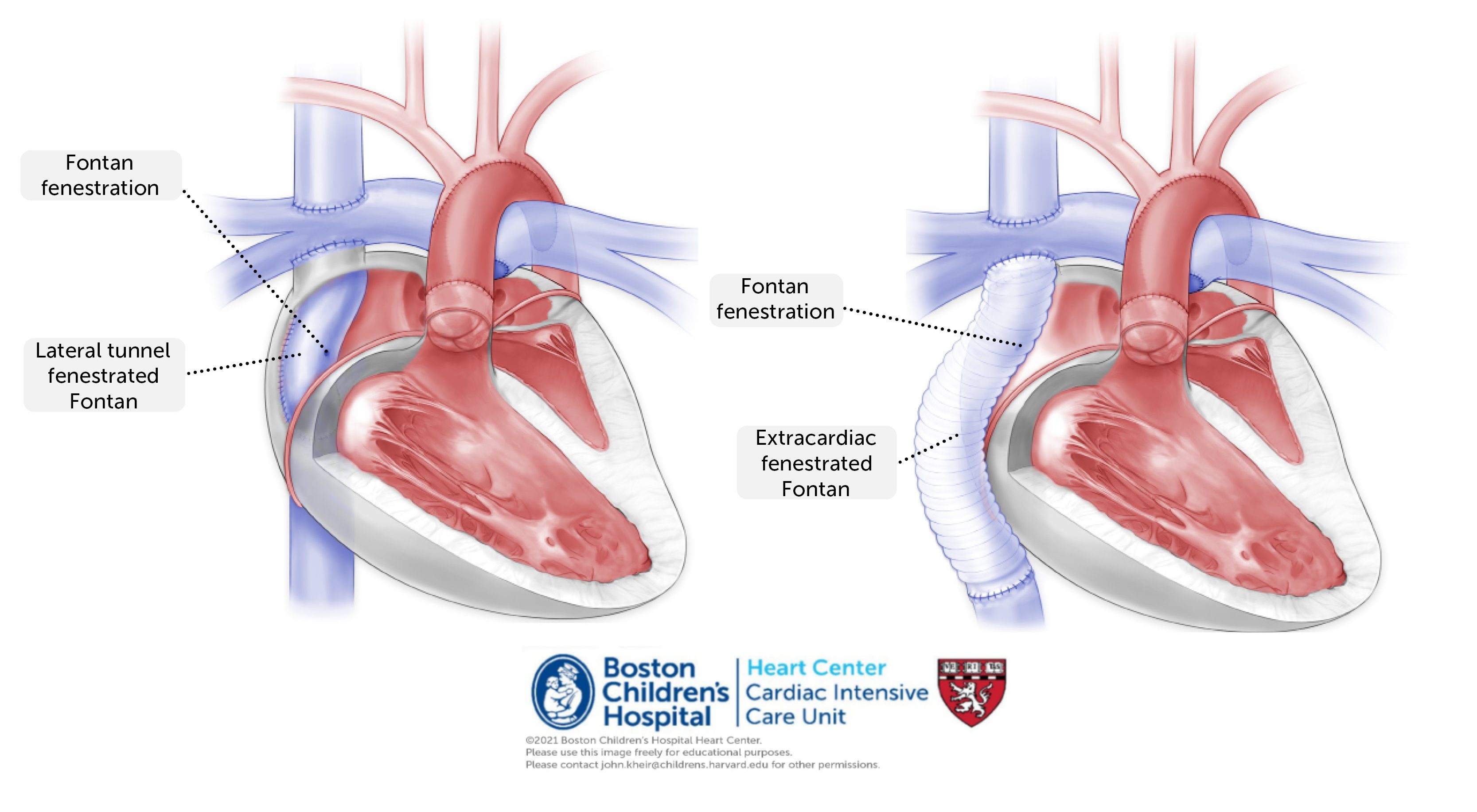
Early Fontan procedures in the 1970s were rudimentary and prone to high failure rates. Today, the evolution of biocompatible materials has changed the game. Modern Fontan circuits utilize Gore-Tex tubes and high-grade synthetic conduits that are designed to resist thrombosis (clotting) and integrate with human tissue. These materials are the product of decades of materials science research, ensuring that the “hardware” implanted into a child can withstand the mechanical stress of millions of heartbeats.
From Scalpel to Precision: The Role of Surgical Robotics
The execution of a Fontan has transitioned from traditional open-heart surgery to increasingly minimally invasive techniques. Surgical robotics, such as the da Vinci system, allow surgeons to perform complex suturing with a level of precision that exceeds the human hand. These robotic platforms provide high-definition 3D visualization, allowing for the micro-calibration of the Fontan conduit, which is crucial for optimizing the flow dynamics of the new circulatory system.
Digital Twins and 3D Modeling in Fontan Planning
One of the most exciting trends in the Tech sector is the use of “Digital Twins”—virtual replicas of physical systems. In the context of the Fontan, this technology is life-saving. No two Fontan patients have the same anatomy, making a “one-size-fits-all” approach impossible. Tech-driven customization is now the gold standard.
Computational Fluid Dynamics (CFD) in Patient Mapping
Before a surgeon ever makes an incision, engineers use Computational Fluid Dynamics (CFD) software—the same tech used to design aircraft wings—to simulate how blood will move through a proposed Fontan circuit. By analyzing the “power loss” and shear stress within a virtual model of the patient’s heart, surgeons can determine the exact angle and placement of the conduit. This predictive modeling minimizes the risk of turbulence, which can lead to energy loss and long-term heart failure.
3D Printing: Physical Prototypes for Complex Anatomies
Building on the digital model, 3D printing technology allows medical teams to hold a physical replica of a patient’s unique heart. Using high-resolution MRI and CT data, 3D printers create multi-material models that mimic the texture of cardiac tissue and vessels. This allows the surgical team to perform “dry runs,” testing different sizes of synthetic conduits to ensure a perfect fit. This marriage of imaging software and additive manufacturing significantly reduces time spent in the operating room.
Virtual Reality (VR) Training for Cardiac Surgeons
Beyond planning, Virtual Reality (VR) is being utilized to train the next generation of pediatric heart surgeons. Specialized VR modules allow trainees to navigate the complex venous structures of a Fontan candidate in a fully immersive digital environment. By practicing the procedure in a high-fidelity simulation, surgeons can anticipate complications and refine their technique, leveraging the same haptic feedback technology found in high-end gaming and flight simulators.
Monitoring the “Fontan Circulation” via Wearable Tech and IoT
A Fontan is not a “cure,” but a lifelong physiological state that requires constant management. This is where the Internet of Things (IoT) and wearable technology play a critical role. The long-term success of a Fontan patient depends on the early detection of subtle changes in venous pressure and oxygen saturation.
Remote Patient Monitoring (RPM) and Post-Operative Safety
The weeks following a Fontan procedure are critical. Modern hospitals are now deploying Remote Patient Monitoring (RPM) platforms that allow patients to recover at home while remaining under a “digital watch.” Smart pulse oximeters and blood pressure cuffs sync via Bluetooth to a centralized cloud platform. If a patient’s oxygen levels dip below a pre-set threshold, AI-driven alerts notify the cardiology team in real-time, preventing emergency readmissions through proactive intervention.
AI-Driven Analytics for Predicting Liver and Renal Complications
Because Fontan circulation relies on high venous pressure, organs like the liver and kidneys are often under chronic stress. Software developers are now building AI algorithms capable of analyzing longitudinal patient data—including lab results, imaging, and activity levels—to predict the onset of “Fontan-Associated Liver Disease” (FALD). These machine learning models can identify patterns invisible to the human eye, allowing for early pharmaceutical or lifestyle adjustments.
The Rise of Smart Stents and Implantable Biosensors
The future of Fontan monitoring lies inside the body. “Smart stents” are currently in development, equipped with micro-sensors that can measure blood flow velocity and pressure from within the Fontan conduit itself. These devices transmit data wirelessly to a smartphone app, providing a continuous stream of “telemetry” for the human heart. This shift from intermittent clinical check-ups to continuous data streams represents the ultimate integration of tech and biology.
The Future of Fontan: Bio-Synthetic Hearts and Genetic Tech
As we look toward the next decade, the “Tech” behind the Fontan is moving toward the molecular and the fully synthetic. The goal is to move beyond a passive “plumbing” fix and toward a solution that restores a two-pump system.
Tissue Engineering and Decellularized Scaffolds
One of the limitations of current Fontan conduits is that they are made of synthetic plastic, which cannot grow with the child. Biotechnology firms are working on “tissue-engineered” grafts. These involve taking a biological scaffold (often from a donor or a 3D-printed collagen structure) and seeding it with the patient’s own stem cells. The result is a “living” conduit that can grow, repair itself, and integrate seamlessly into the body’s endocrine system.
CRISPR and the Potential for In-Utero Genetic Intervention
While the Fontan addresses the physical defect, the next frontier is preventing the defect at the genetic level. Using CRISPR-Cas9 gene-editing technology, researchers are investigating the specific genetic markers that lead to single-ventricle defects. While still in the experimental phase, the long-term tech roadmap includes in-utero genetic therapies that could potentially guide the heart to develop four chambers, rendering the Fontan procedure obsolete.
Machine Learning and the Global Fontan Registry
Data is the fuel of modern technology. The Global Fontan Registry is a massive database that aggregates anonymized data from thousands of Fontan patients worldwide. By applying Big Data analytics to this registry, researchers can identify which surgical techniques and technological interventions lead to the best 30-year outcomes. This global network of data ensures that a technological breakthrough in a lab in Tokyo can be applied to a patient in New York within months, not years.
In conclusion, a Fontan is much more than a surgery; it is a complex technological ecosystem. From the CFD software used in planning to the AI algorithms used in long-term monitoring, the Fontan represents the pinnacle of what is possible when we treat the human body as a system that can be optimized through innovation. For the tech-conscious observer, the evolution of the Fontan serves as a powerful case study in how hardware, software, and biology are merging to redefine the limits of human life.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.