In an era where digital transformation permeates every sector, healthcare stands at the precipice of a profound revolution. The seemingly straightforward question of “what antibiotics are given for strep” – typically answered by a physician with specific drug names like penicillin or amoxicillin – is increasingly being influenced, optimized, and redefined by cutting-edge technology. This article delves into the technological innovations that are shaping how strep throat is diagnosed, how antibiotics are prescribed, managed, and even discovered, moving beyond a simple list of medications to a dynamic ecosystem of digital intervention.
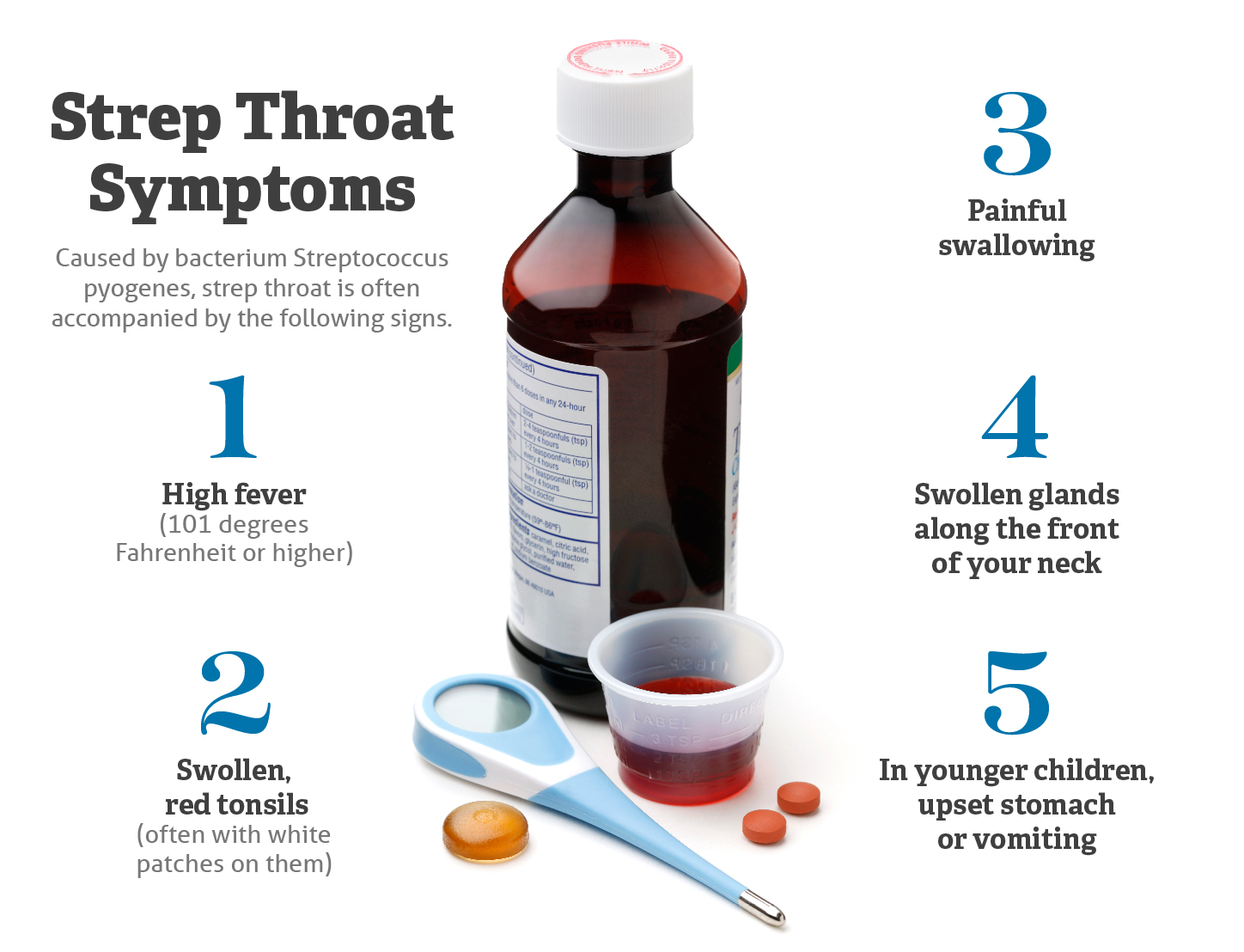
The fight against infectious diseases, including common bacterial infections like Streptococcus pyogenes (strep throat), is critically dependent on effective antibiotics. However, rising antibiotic resistance, the need for precise diagnostics, and the complexities of patient adherence pose significant challenges. Technology emerges as a powerful ally, offering solutions that enhance diagnostic accuracy, streamline treatment protocols, and ultimately preserve the efficacy of these vital drugs. By examining this question through a technological lens, we uncover a world where AI-powered diagnostics, smart prescribing platforms, and advanced research tools are transforming clinical practice and patient outcomes.
Revolutionizing Diagnosis and Prescription: The Tech-Driven Approach to Strep
The journey from a patient presenting with symptoms to receiving an antibiotic prescription for strep throat is being dramatically accelerated and refined by technological advancements. Gone are the days of solely relying on traditional lab cultures or the subjective assessment of symptoms. Digital tools are ushering in an era of precision and speed.
AI and Machine Learning in Rapid Strep Identification
Artificial intelligence (AI) and machine learning (ML) are at the forefront of transforming diagnostic capabilities for strep throat. Historically, rapid strep tests (RSTs) offered quick results but sometimes lacked sensitivity, necessitating follow-up cultures. AI-driven diagnostic platforms are changing this landscape. These systems can analyze digital images of throat swabs or even interpret raw data from novel biosensors with unprecedented speed and accuracy.
For instance, machine vision algorithms can be trained on vast datasets of throat images from both infected and non-infected individuals, learning to identify subtle visual cues of strep infection that might be missed by the human eye or even conventional rapid tests. Furthermore, AI can process complex immunological data from advanced point-of-care devices, providing a highly accurate diagnosis in minutes. This speed is crucial, as early and accurate diagnosis prevents unnecessary antibiotic prescriptions (for viral infections) and ensures timely treatment for bacterial strep, reducing symptom duration and preventing complications like rheumatic fever. By minimizing false positives and false negatives, AI optimizes the decision-making process for clinicians, guiding them toward the correct antibiotic prescription more efficiently.
Telemedicine and Remote Consultations for Timely Antibiotic Access
The advent of telemedicine has dramatically expanded access to healthcare, particularly for common conditions like strep throat. For individuals in remote areas, those with mobility issues, or simply during times when in-person visits are challenging (e.g., pandemics), virtual consultations have become invaluable. Through secure video conferencing platforms, patients can connect with healthcare providers from the comfort of their homes.
While a definitive strep diagnosis often requires a throat swab, telemedicine services are evolving. Some platforms integrate at-home rapid strep test kits, where patients can perform the swab and share results digitally, or even utilize specialized peripheral devices that allow remote visualization of the throat by the clinician. AI-powered symptom checkers can also triage patients, guiding them on whether a virtual consultation is appropriate. Once strep is confirmed or highly suspected based on clinical criteria (e.g., Centor score, if a rapid test is unavailable or not feasible remotely), the physician can electronically send a prescription directly to the patient’s pharmacy. This tech-enabled pathway significantly reduces barriers to care, ensuring that individuals who need antibiotics for strep can get them quickly, minimizing delays that could exacerbate symptoms or lead to spread.
Smart Stewardship: Enhancing Antibiotic Efficacy Through Digital Tools
Prescribing the correct antibiotic is only half the battle. Ensuring its effective use, monitoring for resistance, and educating patients are equally critical. Technology plays a pivotal role in antibiotic stewardship, a coordinated program promoting the appropriate use of antimicrobials.
Mobile Applications for Medication Adherence and Patient Education
Patient adherence to antibiotic regimens is a persistent challenge. Incomplete courses of antibiotics can lead to treatment failure and contribute to antibiotic resistance. Mobile health (mHealth) applications are emerging as powerful tools to address this. These apps can send personalized reminders for medication times, provide clear instructions on dosage and duration, and offer educational content about strep throat and the importance of completing the full course of antibiotics, even if symptoms improve.
Beyond simple reminders, advanced apps can track patient progress, allow for symptom logging, and provide a direct communication channel with healthcare providers for questions or concerns. Some even incorporate gamification elements to encourage adherence, making the process more engaging. By empowering patients with information and tools to manage their treatment, these digital solutions significantly improve adherence rates, ensuring the prescribed antibiotics effectively eradicate the Streptococcus infection and reduce the likelihood of recurrence or the development of resistance.
Electronic Health Records (EHRs) and Data Analytics for Resistance Monitoring
Electronic Health Records (EHRs) are the backbone of modern healthcare data management. Beyond individual patient care, the aggregated data within EHR systems offers an invaluable resource for antibiotic stewardship and public health surveillance. When a patient is prescribed an antibiotic for strep, this information, along with diagnostic results and patient demographics, is meticulously recorded.

Data analytics, powered by sophisticated algorithms, can then process this vast amount of anonymized data. By analyzing patterns of antibiotic prescriptions, treatment outcomes, and resistance profiles across patient populations and geographic regions, healthcare systems can identify emerging trends in antibiotic resistance specific to Streptococcus pyogenes. For example, an increase in treatment failures with a commonly prescribed antibiotic for strep in a particular area could signal developing resistance, prompting a re-evaluation of first-line treatments. Furthermore, EHRs can integrate clinical decision support systems that alert prescribers to local resistance patterns, recommend preferred antibiotics based on current guidelines, and flag potential drug interactions or allergies. This real-time, data-driven approach allows for proactive adjustments to prescribing practices, safeguarding the effectiveness of current antibiotics against strep and other bacterial infections.
The Future Landscape: Advanced Technologies in Antibiotic Development and Delivery
While technology currently optimizes the use of existing antibiotics, its most profound impact may lie in the future – in the discovery of new antimicrobial agents and innovative ways to deliver them. The threat of superbugs and the plateau in novel antibiotic development necessitate a radical shift, and advanced technologies are poised to deliver it.
Gene Editing and Synthetic Biology for Novel Antibiotic Discovery
The traditional method of antibiotic discovery, often relying on natural products, has become less fruitful. However, synthetic biology and gene editing technologies like CRISPR are opening unprecedented avenues. Researchers are now using these tools to engineer bacteria or other microorganisms to produce novel antimicrobial compounds that might not exist in nature. By precisely manipulating genetic pathways, scientists can design microorganisms to synthesize complex molecules with potent antibacterial properties, specifically targeting bacterial weaknesses.
Furthermore, gene editing can be used to modify existing antibiotics to overcome resistance mechanisms or to develop highly specific “smart drugs” that only target pathogenic bacteria, leaving beneficial microbiome untouched. For conditions like strep, this could mean developing next-generation antibiotics that are less prone to resistance and have fewer side effects, offering a long-term solution to the ongoing challenge posed by Streptococcus pyogenes. The ability to rapidly screen thousands of potential compounds and engineer biological systems for drug production drastically accelerates the discovery pipeline.
Nanotechnology and Targeted Drug Delivery Systems
A significant challenge in antibiotic therapy is ensuring the drug reaches the site of infection in sufficient concentration without causing widespread systemic side effects. Nanotechnology offers a revolutionary approach to targeted drug delivery. Nanoparticles can be engineered to encapsulate antibiotics, protecting them from degradation and allowing for their controlled release.
Crucially, these nanoparticles can be designed to specifically target infected cells or bacteria, ignoring healthy tissues. For strep throat, this could involve nanoparticles coated with molecules that bind selectively to Streptococcus pyogenes cells, delivering a concentrated dose of antibiotic directly where it’s needed most in the throat. This targeted approach minimizes the amount of antibiotic required, reduces systemic exposure and potential side effects, and potentially lowers the risk of resistance development in commensal bacteria. Imagine a future where a highly potent, targeted nano-antibiotic could effectively clear a strep infection with minimal impact on the patient’s overall microbiome, representing a significant leap forward in precision medicine.
Addressing Challenges: Cybersecurity and Data Privacy in Digital Healthcare
While technology offers immense promise, its integration into antibiotic management and healthcare at large is not without challenges. The digital nature of these solutions necessitates robust measures to protect patient data and ensure the integrity of clinical processes.
Protecting Sensitive Patient Information
The extensive use of EHRs, telemedicine platforms, and mHealth apps generates vast amounts of highly sensitive patient data, including diagnoses, prescriptions, and adherence patterns. Ensuring the privacy and security of this information is paramount. Cyberattacks on healthcare systems are a growing threat, and breaches can compromise patient confidentiality, lead to identity theft, and erode trust in digital health solutions. Robust encryption protocols, multi-factor authentication, regular security audits, and adherence to strict regulatory frameworks (like HIPAA) are essential. As technology helps determine “what antibiotics are given for strep,” it must simultaneously guarantee that all associated personal health information remains secure and inaccessible to unauthorized parties.
Ensuring Algorithm Transparency and Bias Mitigation
AI and ML algorithms, while powerful, are only as good as the data they are trained on. Biases present in training data (e.g., disproportionate representation of certain demographics) can lead to biased diagnostic or prescriptive recommendations, potentially exacerbating health disparities. For example, an AI designed to aid in strep diagnosis might perform less accurately for certain ethnic groups if the training data was not sufficiently diverse.
Therefore, ensuring algorithm transparency and actively mitigating bias are critical ethical considerations. Developers must rigorously test AI systems across diverse populations, articulate how their algorithms arrive at conclusions, and provide mechanisms for human oversight and intervention. As technology increasingly guides decisions about “what antibiotics are given for strep,” it is crucial that these tools serve all patients equitably and transparently, augmenting human expertise rather than replacing critical thinking.
Conclusion
The question “what antibiotics are given for strep” has evolved beyond a simple medical query; it has become a gateway to understanding the profound impact of technology on modern medicine. From AI-driven diagnostics that deliver rapid, accurate results to mobile apps that empower patients with adherence tools, and from synthetic biology that promises novel drug discoveries to nanotechnology for precision delivery, technology is reshaping every facet of antibiotic management. While the challenges of cybersecurity and algorithmic bias demand vigilant attention, the digital revolution offers an unparalleled opportunity to enhance the efficacy of antibiotics, combat resistance, and ultimately improve global health outcomes. The future of treating strep, and indeed all bacterial infections, is undeniably a future driven by innovation and smart technological integration.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.