Lexapro, the brand name for escitalopram, is a widely prescribed antidepressant belonging to the class of selective serotonin reuptake inhibitors (SSRIs). Its efficacy in treating conditions like major depressive disorder (MDD) and generalized anxiety disorder (GAD) has made it a cornerstone in psychiatric pharmacotherapy. However, like any potent medication, understanding its dosage, particularly the maximum recommended dose, is crucial for both patients and healthcare providers to ensure safety and optimal therapeutic outcomes. This article will delve into the intricacies of Lexapro dosage, exploring the concept of maximum dose, factors influencing it, potential risks associated with exceeding it, and strategies for managing treatment effectively.
While the question “what is the max dose of Lexapro” seems straightforward, the answer is nuanced and highly individualized. There isn’t a single, universal “maximum dose” that applies to everyone. Instead, healthcare professionals determine the appropriate dosage based on a patient’s specific condition, response to treatment, age, weight, kidney and liver function, and the presence of any other medical conditions or medications. This personalized approach is paramount in minimizing side effects and maximizing the therapeutic benefits of Lexapro.
Understanding Lexapro Dosing: From Starting Point to Titration
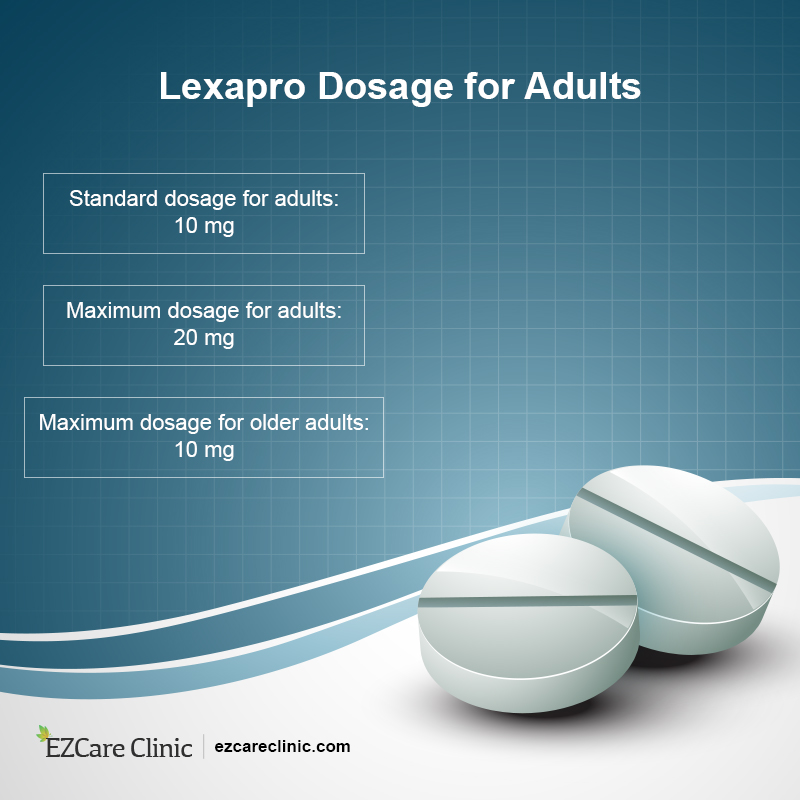
The journey with Lexapro typically begins with a low starting dose. This cautious approach allows the body to adjust to the medication and helps identify potential sensitivities or adverse reactions early on. For adults, a common starting dose for both MDD and GAD is 10 mg taken orally once a day. This dose is often maintained for at least one week before considering any adjustments.
Initial Therapeutic Response and Titration
The initial therapeutic response to Lexapro can vary significantly among individuals. Some may experience noticeable improvements in their symptoms within a few weeks, while others may require longer to feel the full effects. It’s essential for patients to communicate openly with their doctor about their progress and any symptoms they are experiencing, both positive and negative.
Based on the patient’s response and tolerance, the prescribing physician may gradually increase the dose. This process, known as titration, is carefully managed to find the lowest effective dose that provides symptom relief without causing unacceptable side effects. For MDD and GAD, the dose can be increased to 20 mg per day after a minimum of one week at the initial 10 mg dose. This is generally considered the maximum recommended daily dose for most adults.
The Concept of Maximum Dose: Safety Thresholds and Clinical Considerations
When discussing the “maximum dose” of Lexapro, it’s crucial to differentiate between the generally accepted therapeutic maximum and a potentially higher, cautiously administered dose under strict medical supervision. The maximum recommended daily dose of Lexapro for adults is typically 20 mg. This threshold is established based on extensive clinical trials and post-marketing surveillance, which have identified this level as generally safe and effective for the majority of patients experiencing MDD or GAD.
Exceeding the Recommended Maximum: When and Why?
While 20 mg is the standard maximum, there might be rare instances where a healthcare provider considers a higher dose, such as 30 mg or even 40 mg, for very specific and severe cases that have not responded to lower doses. This decision is never taken lightly and involves a rigorous risk-benefit assessment.
Several factors might lead a physician to consider a dose above 20 mg:
- Treatment-Resistant Depression: In individuals with major depressive disorder who have failed to respond to multiple antidepressant trials, including Lexapro at the standard maximum dose, a physician might cautiously explore higher dosages. The rationale here is that some individuals may have a higher threshold for serotonin reuptake inhibition required to achieve a therapeutic effect.
- Severity of Symptoms: In exceptionally severe cases of depression or anxiety where symptoms are debilitating and pose a significant risk to the patient’s well-being, a physician might consider dose escalation.
- Individualized Pharmacokinetics: While less common, certain individuals may metabolize Lexapro differently, potentially requiring higher doses to achieve therapeutic blood levels. This is often determined through genetic testing or careful monitoring of drug levels, though the latter is not routine for SSRIs.
It is imperative to stress that doses exceeding 20 mg per day are not standard practice and carry a significantly increased risk of adverse effects. Such adjustments are typically made in an inpatient setting or under very close outpatient monitoring by an experienced psychiatrist.
Risks Associated with Exceeding the Maximum Dose
Increasing the dose of Lexapro beyond the recommended 20 mg per day can elevate the risk and severity of several adverse effects. The potential for these side effects often escalates with higher doses, making careful monitoring and risk assessment paramount.
Common side effects that may become more pronounced or frequent at higher doses include:
- Gastrointestinal Disturbances: Nausea, diarrhea, dry mouth, and constipation are common SSRI side effects that can worsen with dose escalation.
- Central Nervous System Effects: Dizziness, drowsiness, insomnia, headache, and tremors can become more problematic.
- Sexual Dysfunction: Decreased libido, difficulty achieving orgasm, and erectile dysfunction are well-known SSRI side effects that can be dose-dependent.
- Serotonin Syndrome: This is a potentially life-threatening condition that occurs when there is too much serotonin in the body. Symptoms can range from mild (agitation, confusion, rapid heart rate, sweating) to severe (high fever, seizures, muscle rigidity, loss of consciousness). The risk of serotonin syndrome increases with higher doses of SSRIs, especially when combined with other serotonergic agents.
- Hyponatremia: Low sodium levels in the blood can occur, particularly in older adults, and can lead to symptoms like headache, confusion, fatigue, and even seizures. Higher doses may increase this risk.
- Increased Risk of Bleeding: SSRIs can interfere with platelet aggregation, potentially increasing the risk of bleeding, especially when combined with NSAIDs or anticoagulants. This risk may be amplified at higher doses.
- QTc Prolongation: In rare cases, Lexapro can prolong the QTc interval on an electrocardiogram, which can increase the risk of serious heart rhythm abnormalities. While this is a concern even at therapeutic doses, higher doses might exacerbate this risk in susceptible individuals.
Special Populations and Dosage Adjustments
The standard dosing guidelines for Lexapro are primarily for adult populations. Special considerations are necessary for children, adolescents, and older adults, as well as individuals with impaired organ function.
Pediatric and Adolescent Dosing
The use of Lexapro in children and adolescents is approved for major depressive disorder and generalized anxiety disorder. However, dosing recommendations differ from adults. For individuals aged 12 to 17 years, the starting dose is typically 10 mg per day. After at least one week, the dose can be increased to 20 mg per day if tolerated and clinically indicated. The maximum recommended dose for adolescents aged 12 to 17 is also 20 mg per day.
It’s important to note that there is a black box warning for antidepressants regarding an increased risk of suicidal thoughts and behaviors in children, adolescents, and young adults. Close monitoring for any worsening of depression or emergence of suicidal ideation is essential during the initial phases of treatment and any dose adjustments.
Geriatric Considerations
For older adults (typically those over 65 years of age), a lower starting dose may be recommended, often 5 mg per day. This is due to potential age-related changes in metabolism and increased sensitivity to medication side effects. While the maximum dose for older adults is generally still considered 20 mg per day, a physician might opt for a lower dose even at the upper end of the therapeutic range if it effectively manages symptoms and is well-tolerated.
Patients with Hepatic or Renal Impairment
Individuals with moderate to severe liver or kidney impairment may require dose adjustments. The liver metabolizes Lexapro, and impaired liver function can lead to higher drug concentrations in the body, increasing the risk of side effects. Similarly, impaired kidney function can affect the elimination of the drug. In such cases, a healthcare provider might recommend a lower starting dose and a slower titration schedule, with careful monitoring of both symptom response and potential adverse reactions. The maximum dose for these individuals might be lower than the standard 20 mg, determined on a case-by-case basis.
Managing Lexapro Treatment: Beyond the Maximum Dose
The question of “what is the max dose of Lexapro” highlights an important aspect of pharmacotherapy: the goal is to find the optimal dose, not necessarily the highest possible dose. Effective Lexapro treatment involves a holistic approach that extends beyond simply determining a numerical dosage limit.
The Importance of Ongoing Monitoring and Communication
The cornerstone of safe and effective Lexapro treatment is consistent monitoring and open communication between the patient and their healthcare provider. This includes:
- Regular Follow-Up Appointments: Scheduled visits allow the doctor to assess symptom improvement, identify and manage side effects, and make necessary dose adjustments.
- Reporting Side Effects Promptly: Patients should be encouraged to report any new or worsening side effects immediately, no matter how minor they may seem.
- Adherence to Prescribed Dosage: It is crucial for patients to take Lexapro exactly as prescribed and not to alter their dosage or stop the medication without consulting their doctor. Abruptly stopping Lexapro can lead to withdrawal symptoms, which can be unpleasant and mimic a relapse of the original condition.
Alternative and Adjunctive Treatments
For individuals who do not achieve adequate symptom relief with Lexapro at the maximum recommended dose, or who experience intolerable side effects, healthcare providers may consider alternative treatment strategies. These can include:
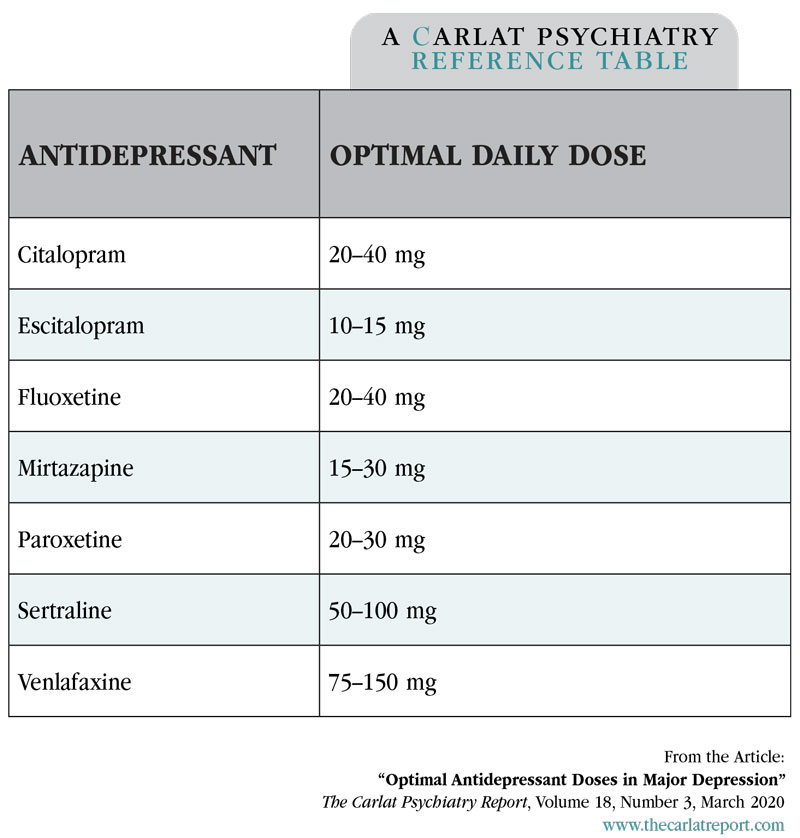
- Switching to a Different Antidepressant: Other classes of antidepressants, such as SNRIs (serotonin-norepinephrine reuptake inhibitors), tricyclic antidepressants (TCAs), or atypical antidepressants, may be more effective or better tolerated by some individuals.
- Augmentation Therapy: This involves adding another medication to Lexapro to enhance its effectiveness. Common augmentation strategies include lithium, atypical antipsychotics (e.g., aripiprazole, quetiapine), or thyroid hormone.
- Psychotherapy: Cognitive Behavioral Therapy (CBT), Interpersonal Therapy (IPT), and other forms of psychotherapy can be highly effective in treating depression and anxiety, either alone or in conjunction with medication.
- Lifestyle Modifications: Engaging in regular exercise, maintaining a healthy diet, ensuring adequate sleep, and practicing stress-management techniques can significantly contribute to overall mental well-being and complement pharmacological treatments.
The Role of Technology and Data in Personalized Medicine
In the evolving landscape of healthcare, technology plays an increasingly vital role in personalizing treatment. While not yet standard practice for SSRIs like Lexapro, future advancements may involve:
- Pharmacogenomic Testing: Genetic testing can identify variations in enzymes that metabolize certain medications, potentially predicting how an individual will respond to and tolerate Lexapro. This could help guide initial dosing and minimize trial-and-error.
- Wearable Devices and Digital Health Platforms: These technologies can passively collect data on sleep patterns, activity levels, and mood fluctuations, providing clinicians with a more comprehensive picture of a patient’s condition and response to treatment, potentially allowing for earlier detection of issues or effectiveness.
- AI-Powered Predictive Analytics: As more data becomes available, artificial intelligence could potentially be used to predict which patients are most likely to benefit from higher doses or specific augmentation strategies, leading to more tailored treatment plans.
Conclusion: A Balanced Approach to Lexapro Dosing
The question of “what is the max dose of Lexapro” is best answered by understanding that the maximum recommended daily dose for most adults is 20 mg. This threshold is established to balance therapeutic efficacy with safety. While exceptions may exist for very specific and severe treatment-resistant cases under strict medical supervision, exceeding this dose significantly amplifies the risk of adverse effects, including the potentially dangerous serotonin syndrome.
Ultimately, effective Lexapro treatment is a collaborative effort between patient and physician, characterized by careful titration, ongoing monitoring, open communication, and a willingness to explore alternative or adjunctive treatments when necessary. By adhering to these principles, individuals can navigate their treatment journey with Lexapro safely and effectively, striving for optimal mental health and well-being.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.
