The Human Papillomavirus (HPV) jab, more commonly known as the HPV vaccine, represents one of the most significant breakthroughs in preventive medicine in recent decades. Far from being just another pharmaceutical product, its development and deployment embody a complex interplay of advanced biotechnology, molecular engineering, public health informatics, and digital communication strategies. Understanding “what is the HPV jab” requires delving into the sophisticated scientific and technological innovations that brought it from laboratory concept to a global health intervention, significantly altering the landscape of cancer prevention.
The Science Behind the Shield: Understanding HPV and Its Impact
Before appreciating the technological marvel of the HPV jab, it’s crucial to grasp the biological adversary it confronts: the Human Papillomavirus. This highly prevalent virus, often transmitted through intimate skin-to-skin contact, is responsible for a spectrum of health issues, from benign warts to several types of cancer. The very existence of such a vaccine underscores a powerful narrative of human ingenuity in the face of persistent biological threats.
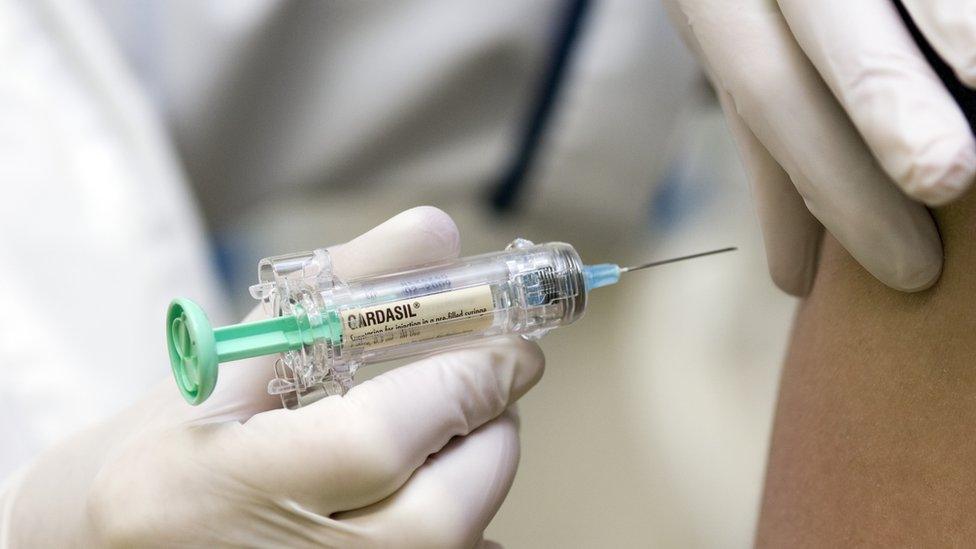
Decoding the Human Papillomavirus (HPV)
HPV is not a single entity but a diverse group of over 200 related viruses, each identified by a number. While many HPV types are harmless and resolve spontaneously, about 14 types are classified as “high-risk” due to their oncogenic potential. The most notorious among these are HPV-16 and HPV-18, which together cause approximately 70% of all cervical cancers worldwide. Beyond cervical cancer, high-risk HPV types are also implicated in cancers of the anus, vulva, vagina, penis, and oropharynx (throat, tonsils, and base of the tongue). Low-risk types, such as HPV-6 and HPV-11, are primarily responsible for genital warts, a common and often distressing condition. The ubiquitous nature of HPV infection, with most sexually active individuals acquiring at least one type at some point in their lives, posed a colossal public health challenge that demanded a comprehensive, technologically advanced solution.
The Rationale for Technological Intervention
For decades, the primary strategy for managing HPV-related cancers, particularly cervical cancer, revolved around screening programs like the Pap test. While effective at detecting precancerous lesions, these methods are reactive rather; they identify disease after it has begun to develop. They do not prevent the initial infection. This limitation highlighted a critical gap in medical technology: the need for a truly preventive measure. The sheer scale of HPV infection, its asymptomatic nature in many cases, and the devastating long-term consequences of high-risk types created an urgent demand for a technological breakthrough that could interrupt the infection pathway before disease manifestation. The vision was to create a tool that could confer immunity, thereby preventing infection and, consequently, the development of HPV-related cancers and diseases. This audacious goal spurred intense biotechnological research, ultimately leading to the development of the HPV vaccine.
Engineering Immunity: How the HPV Jab Works
The HPV jab is not merely a dose of inactivated virus; it is a sophisticated product of molecular engineering and immunology. Its efficacy lies in its ability to harness the body’s own immune system, teaching it to recognize and neutralize HPV without ever exposing the individual to the live virus. This approach is a cornerstone of modern vaccinology, leveraging advanced biotechnology to create safe yet potent immunogens.
Vaccine Development: A Biotechnological Marvel
The core technological innovation behind the HPV vaccine is the use of Virus-Like Particles (VLPs). Researchers discovered that the major capsid protein (L1) of HPV, when expressed in a host cell (like yeast or insect cells through recombinant DNA technology), can self-assemble into structures that look almost identical to the outer shell of the actual HPV virus. Crucially, these VLPs contain no viral genetic material (DNA), meaning they are non-infectious and cannot replicate or cause disease.
The development of VLPs was a triumph of genetic engineering and protein biochemistry. Scientists identified the specific genes coding for the L1 protein, isolated them, and then introduced them into production systems where these proteins could be synthesized in large quantities. The subsequent self-assembly of these proteins into VLPs is a remarkable example of nanoscale engineering, mimicking nature’s design to create a perfect decoy. This VLP technology is central to the safety and effectiveness of the vaccine, allowing for a strong immune response without any risk of viral infection. The precision required to consistently produce these complex protein structures at scale, ensuring their stability and immunogenicity, underscores the high level of technological mastery involved.
Mechanism of Action: Training the Immune System
Once injected, these carefully engineered VLPs enter the body and are recognized by the immune system as foreign invaders. Because the VLPs closely resemble the real virus, they effectively “trick” the immune system into mounting a robust response. Specialized immune cells, such as antigen-presenting cells, process the VLPs and display fragments of their protein on their surface. This presentation activates T-helper cells and B cells. The B cells, in particular, are stimulated to produce large quantities of antibodies specifically tailored to bind to the L1 protein on the surface of HPV.
This process is a form of advanced biological programming. The immune system develops a “memory” of these VLPs. Should the vaccinated individual encounter the actual HPV virus in the future, their immune system is primed and ready. The pre-existing antibodies can rapidly bind to the incoming viral particles, preventing them from attaching to and infecting human cells. This neutralization process effectively blocks the initial stages of infection, thereby preventing the entire cascade of events that could lead to persistent infection and ultimately cancer. The sustained and high levels of antibodies generated by the HPV vaccine are a testament to the powerful immunogenic properties of the VLP platform, making it one highly effective preventive intervention.
Deployment and Digital Integration: Accessing and Monitoring Impact
The journey of the HPV jab from laboratory to widespread public health tool also showcases significant advancements in logistical technology and digital health infrastructure. The efficacy of the vaccine is only fully realized when it reaches the populations it is intended to protect, a process heavily reliant on sophisticated deployment strategies and continuous monitoring through data-driven approaches.
Vaccine Delivery Systems and Public Health Infrastructure
Distributing a vaccine globally involves overcoming immense logistical challenges, particularly maintaining the “cold chain” – a temperature-controlled supply chain that ensures vaccines remain potent from the manufacturing plant to the point of administration. This requires specialized refrigeration technology, insulated transport containers, and meticulous temperature monitoring devices across vast distances. Digital sensors and IoT (Internet of Things) devices play a crucial role in real-time tracking of vaccine shipments and temperature excursions, alerting health officials to potential issues before vaccine integrity is compromised.
Furthermore, national immunization programs leverage sophisticated databases and software systems for registration, scheduling, and tracking vaccination records. Digital health records ensure that individuals receive the complete recommended series of doses and facilitate follow-up. In many regions, mobile applications and digital portals are being developed to empower individuals to access their vaccination history, receive reminders, and find nearby vaccination centers, making the entire process more accessible and user-friendly. These technological underpinnings are critical for the efficient and equitable distribution of the HPV jab.
Leveraging Data and AI for Surveillance and Outreach
Beyond delivery, technology plays a pivotal role in monitoring the long-term impact and safety of the HPV vaccine. Large-scale epidemiological studies, facilitated by robust health information systems and big data analytics, continuously track vaccine efficacy rates, the reduction in HPV infection prevalence, and the decline in rates of HPV-related diseases and cancers. Artificial intelligence (AI) and machine learning algorithms are increasingly employed to analyze vast datasets from population registries, electronic health records, and surveillance systems. These tools can identify trends, predict potential outbreaks, and evaluate the effectiveness of vaccination campaigns with unprecedented speed and accuracy.
Moreover, digital communication platforms and social media analytics are vital for public health outreach. AI-powered tools can analyze public sentiment surrounding vaccines, identify misinformation hotspots, and help tailor targeted educational campaigns to address specific concerns. By understanding audience engagement and information consumption patterns, health authorities can design more effective messaging strategies to promote vaccine uptake and reinforce public trust. The digital ecosystem is thus integral to ensuring the sustained success and public acceptance of the HPV jab.
The Future of Vaccine Technology: Beyond the Current HPV Jab
The success of the current HPV jab, underpinned by VLP technology, also paves the way for the next generation of vaccine innovations. The field of vaccinology is rapidly evolving, driven by new scientific discoveries and advanced technological platforms that promise even more effective, broader-spectrum, and potentially personalized immunizations.
Next-Generation Vaccine Platforms
While VLP technology remains highly effective, ongoing research explores alternative and potentially more versatile vaccine platforms. Messenger RNA (mRNA) vaccines, famously brought to the forefront by COVID-19, offer unparalleled speed in development and manufacturing. Future HPV vaccines could potentially leverage mRNA technology to induce immunity against a wider array of HPV types, or even incorporate antigens from other pathogens. Viral vector vaccines, another advanced platform, use modified viruses to deliver genetic material encoding HPV antigens, offering robust immune responses and potentially single-dose efficacy. These next-generation technologies represent a paradigm shift, enabling faster responses to emerging threats and the development of vaccines that are both highly specific and broadly protective. The modular nature of these platforms also holds promise for combination vaccines, reducing the number of injections required and improving vaccine coverage.

Personalized Medicine and Immunotherapy Synergies
The horizon of medical technology also includes the integration of personalized medicine with vaccinology. Advanced genomic sequencing and bioinformatics could allow for the identification of individual genetic predispositions to HPV infection or disease progression, potentially guiding more tailored vaccination strategies or risk assessments. Furthermore, the convergence of preventive vaccines with therapeutic immunotherapies is an exciting area. While the current HPV jab is prophylactic, future advancements could explore therapeutic HPV vaccines designed to treat existing HPV infections or even early-stage HPV-related cancers by boosting the body’s immune response against infected cells. This synergistic approach, combining prevention with targeted treatment, represents the pinnacle of biomedical technology, offering comprehensive strategies for disease control. Diagnostic technologies will also continue to evolve, with non-invasive and highly sensitive tests further refining our ability to monitor HPV exposure and vaccine effectiveness, creating a feedback loop that continually refines public health strategies.
In conclusion, the HPV jab is far more than a simple injection; it is a profound testament to the power of biomedical technology. From the intricate molecular engineering of Virus-Like Particles to the sophisticated digital infrastructure supporting its global deployment and monitoring, every aspect of the HPV vaccine’s journey is steeped in scientific and technological innovation. It stands as a beacon of what can be achieved when cutting-edge research converges with public health imperatives, offering a tangible pathway to prevent cancer and improve global health outcomes through a meticulously engineered solution.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.