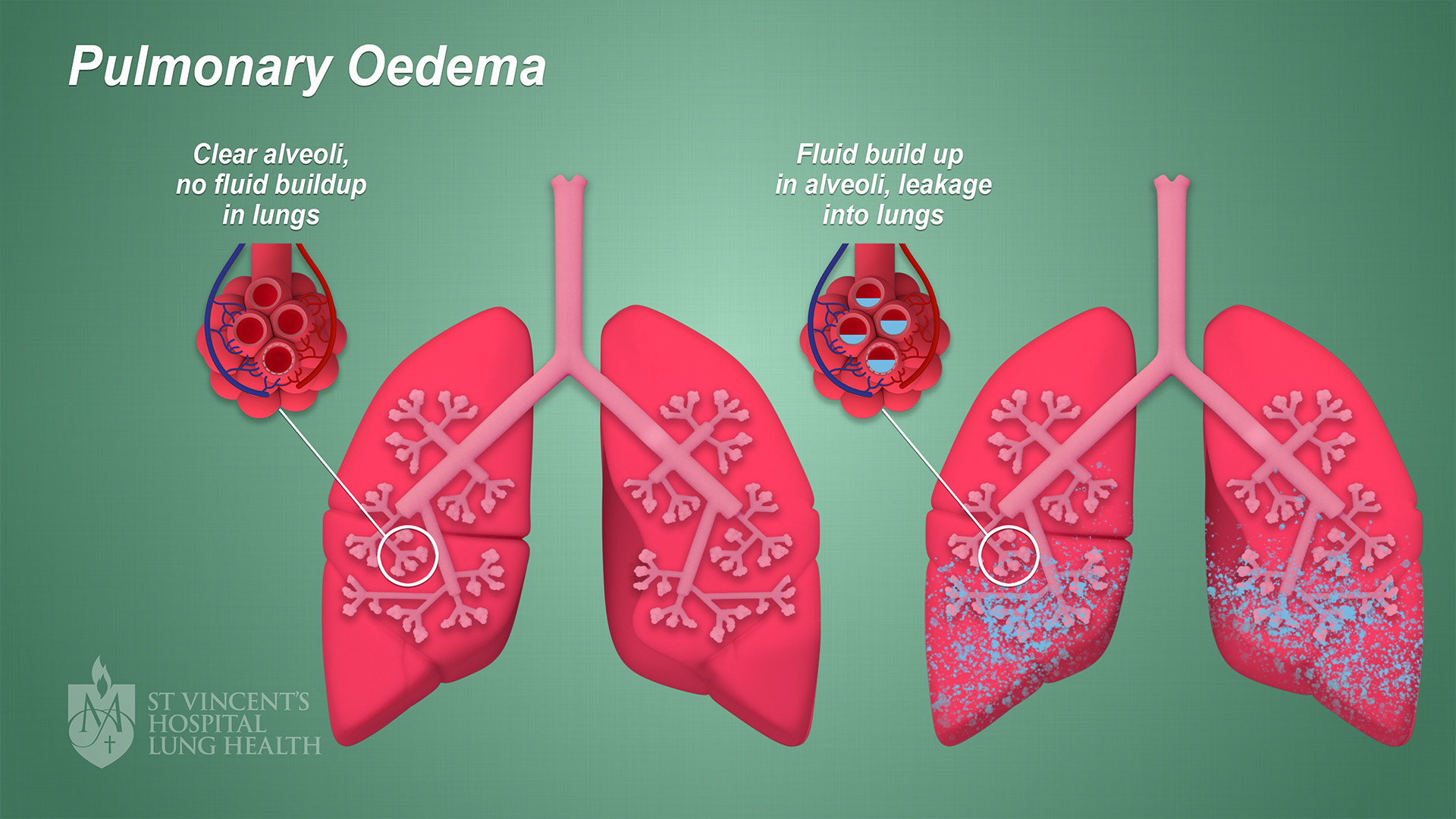
Pulmonary edema, commonly known as edema of the lungs, is a medical condition characterized by an abnormal accumulation of fluid in the air sacs (alveoli) of the lungs. This excess fluid interferes with the lungs’ ability to perform their primary function: the exchange of oxygen and carbon dioxide. When this vital process is compromised, it can lead to significant respiratory distress and, in severe cases, be life-threatening. While the term “edema” itself signifies swelling caused by fluid retention, when it specifically targets the lungs, it necessitates a detailed understanding of its causes, symptoms, diagnosis, and treatment.

The intricate structure of the lungs is designed for efficient gas exchange. Millions of tiny air sacs, the alveoli, are surrounded by a network of delicate blood vessels called capillaries. Oxygen from inhaled air passes through the thin walls of the alveoli and capillaries into the bloodstream, while carbon dioxide, a waste product, travels from the blood into the alveoli to be exhaled. In pulmonary edema, this delicate balance is disrupted as fluid leaks from the capillaries into the interstitial space between the alveoli and then into the alveoli themselves. This fluid acts as a barrier, hindering the passage of oxygen into the blood and the removal of carbon dioxide.
Understanding pulmonary edema is crucial for both individuals experiencing symptoms and for the broader healthcare landscape. While this article focuses on the medical aspects, it’s worth noting how advancements in technology and data analysis are revolutionizing diagnostic capabilities and treatment strategies. From sophisticated imaging techniques to AI-powered predictive models, the tech sector plays an increasingly vital role in managing complex medical conditions like edema of the lungs. Furthermore, the financial implications, both for individuals facing medical expenses and for the healthcare industry, highlight the importance of accessible and effective care.
Causes of Pulmonary Edema: A Multifaceted Origin
The accumulation of fluid in the lungs isn’t a disease in itself but rather a symptom or complication of an underlying issue. These underlying causes can be broadly categorized into two main groups: cardiogenic and non-cardiogenic.
Cardiogenic Pulmonary Edema: When the Heart is the Culprit
Cardiogenic pulmonary edema arises from problems with the heart. The most common cause is heart failure, particularly left-sided heart failure. In this scenario, the left ventricle of the heart, responsible for pumping oxygenated blood to the rest of the body, weakens and cannot effectively pump blood. This leads to a backup of blood in the left atrium and then into the pulmonary veins. The increased pressure within the pulmonary capillaries forces fluid to leak into the lung tissues.
Several conditions can lead to heart failure and, consequently, cardiogenic pulmonary edema:
- Coronary Artery Disease (CAD): Blockages in the arteries supplying blood to the heart muscle can weaken it, impairing its pumping ability.
- Hypertension (High Blood Pressure): Chronically high blood pressure forces the heart to work harder, eventually leading to its enlargement and weakening.
- Valvular Heart Disease: Malfunctioning heart valves can impede blood flow, increasing pressure within the heart chambers and lungs.
- Cardiomyopathy: Diseases of the heart muscle itself, whether inherited or acquired, can reduce its ability to pump blood efficiently.
- Arrhythmias: Irregular heart rhythms can disrupt the heart’s pumping action and contribute to fluid buildup.
In essence, when the heart fails to pump blood effectively, the pressure in the lungs increases, pushing fluid out of the blood vessels and into the air sacs.
Non-Cardiogenic Pulmonary Edema: Beyond Heart Problems
Non-cardiogenic pulmonary edema, also known as Acute Respiratory Distress Syndrome (ARDS) when severe, stems from direct injury to the lung tissues or the capillaries within them. Unlike cardiogenic edema, the heart’s pumping function is typically not the primary issue.
Common causes of non-cardiogenic pulmonary edema include:
- Pneumonia: Severe lung infections can inflame the lung tissue and damage the capillaries, leading to fluid leakage.
- Sepsis: A life-threatening response to infection, sepsis can cause widespread inflammation throughout the body, including the lungs, damaging their delicate structures.
- Inhalation Injury: Breathing in toxic fumes, smoke, or chemicals can directly damage the lung lining and capillaries. This is often seen in individuals who have experienced fires.
- Near Drowning: When water enters the lungs, it can trigger an inflammatory response and disrupt gas exchange, leading to pulmonary edema.
- Trauma: Severe chest injuries or other forms of trauma can cause damage to the lungs and surrounding blood vessels.
- Kidney Failure: In certain cases of severe kidney dysfunction, the body may retain excess fluid, which can contribute to pulmonary edema.
- High Altitude Pulmonary Edema (HAPE): Rapid ascent to high altitudes can cause a person’s blood vessels in the lungs to constrict, increasing pressure and leading to fluid leakage. This is a specific form of non-cardiogenic edema.
- Certain Medications and Toxins: Some drugs and poisons can directly injure the lungs or cause an inflammatory reaction that leads to fluid buildup.
The distinction between cardiogenic and non-cardiogenic edema is critical as it dictates the appropriate diagnostic approach and treatment strategy.
Recognizing the Symptoms: A Cry for Help from the Lungs
The symptoms of pulmonary edema can vary in severity, depending on the underlying cause and how quickly the fluid is accumulating. When fluid builds up in the lungs, it directly impedes breathing, leading to a range of distressing signs.
Acute Symptoms: The Immediate Distress
In cases of sudden onset, such as with acute heart failure or ARDS, the symptoms can be dramatic and require immediate medical attention. These include:
- Severe Shortness of Breath (Dyspnea): This is often the hallmark symptom. The individual feels as though they cannot get enough air, and the sensation can be intense and frightening. It is often worse when lying down (orthopnea) and may wake the person from sleep (paroxysmal nocturnal dyspnea).
- Coughing: The cough may be dry initially but often becomes productive, bringing up frothy or pink-tinged sputum. This is a sign of blood mixing with the accumulated fluid.
- Chest Pain: While not always present, some individuals may experience chest tightness or pain, especially if the underlying cause is cardiac in nature.
- Rapid Heartbeat (Tachycardia): The heart may beat faster in an attempt to compensate for the reduced oxygen in the blood.
- Rapid Breathing (Tachypnea): The respiratory rate increases significantly as the body tries to take in more oxygen.
- Bluish Discoloration of the Skin and Lips (Cyanosis): This is a serious sign indicating dangerously low oxygen levels in the blood.
- Sweating: Profuse sweating can occur due to the body’s stress response.
- Anxiety and Restlessness: The difficulty breathing can lead to significant anxiety and a feeling of panic.
Chronic or Gradual Symptoms: A Slow Decline
In some cases, particularly with chronic heart failure, pulmonary edema may develop more gradually. The symptoms might be less dramatic but can still significantly impact quality of life. These can include:
- Increasing Fatigue: The body’s reduced oxygen supply can lead to persistent tiredness.
- Swelling in the Legs and Ankles (Peripheral Edema): While the primary issue is in the lungs, fluid retention can also manifest elsewhere in the body.
- Shortness of Breath with Exertion: Activities that were once easy may become difficult due to breathlessness.
- Weight Gain: This can be due to fluid retention.
- Reduced Ability to Exercise: The physical limitations imposed by breathlessness can lead to a sedentary lifestyle.
It is crucial to recognize that these symptoms can be indicative of a serious underlying medical condition. Prompt medical evaluation is essential for accurate diagnosis and timely intervention.
Diagnosis and Management: A Collaborative Approach
Diagnosing pulmonary edema involves a combination of medical history, physical examination, and various diagnostic tests. Once diagnosed, the management aims to address the underlying cause, remove excess fluid, and support respiratory function. This is where the synergy between medical expertise and technological innovation becomes most apparent.
Diagnostic Tools: Unveiling the Fluid
Healthcare professionals will gather a detailed medical history, asking about symptoms, pre-existing conditions, and any recent events that might be relevant. A physical examination will focus on listening to the lungs for abnormal sounds (crackles, wheezes), checking heart rate and rhythm, and assessing for signs of fluid retention elsewhere.
Key diagnostic tools may include:
- Chest X-ray: This is a fundamental imaging technique that can reveal the presence of fluid in the lungs, the pattern of distribution, and any signs of underlying heart enlargement or lung disease.
- Echocardiogram (Echo): This ultrasound of the heart assesses its structure and function, helping to determine if heart problems are the cause of the edema. It can measure the heart’s pumping strength and evaluate the valves.
- Electrocardiogram (ECG/EKG): This test records the electrical activity of the heart and can detect arrhythmias or evidence of a heart attack.
- Blood Tests: These can help identify markers of heart strain, infection, kidney function, and oxygen levels in the blood (arterial blood gas analysis).
- Pulmonary Artery Catheterization (Swan-Ganz Catheter): In critical care settings, this invasive procedure can directly measure pressures within the heart and pulmonary artery, providing detailed information about the severity of heart failure and fluid status.
- CT Scan of the Chest: While a chest X-ray is often sufficient, a CT scan can provide more detailed images of the lungs and surrounding structures, which may be helpful in diagnosing specific causes of non-cardiogenic edema.
The application of advanced imaging analysis software and AI algorithms can assist radiologists in interpreting complex scans more accurately and efficiently, potentially speeding up the diagnostic process.
Treatment Strategies: Restoring Balance
The treatment for pulmonary edema is highly individualized and depends on the underlying cause. The primary goals are to:
-
Improve Breathing and Oxygenation:
- Oxygen Therapy: Administering supplemental oxygen is a cornerstone of treatment to improve blood oxygen levels. This can be delivered via nasal prongs, a face mask, or in more severe cases, through mechanical ventilation.
- Positive Pressure Ventilation (CPAP/BiPAP): These non-invasive ventilation methods help keep the airways open and reduce the work of breathing.
- Mechanical Ventilation: In severe cases, a breathing tube may be inserted into the trachea, and a machine will assist or control breathing.
-
Remove Excess Fluid:
- Diuretics (Water Pills): These medications help the kidneys excrete excess fluid from the body, reducing the fluid in the lungs and the rest of the circulatory system.
- Reducing Fluid and Sodium Intake: For individuals with underlying heart failure, dietary modifications are crucial to prevent further fluid overload.
-
Address the Underlying Cause:
- For Cardiogenic Edema: Medications to improve heart function (e.g., ACE inhibitors, beta-blockers, digoxin), manage blood pressure, and treat arrhythmias are essential. In some cases, surgical interventions like angioplasty or valve repair may be necessary.
- For Non-Cardiogenic Edema: Treatment focuses on managing the specific cause, such as antibiotics for pneumonia, supportive care for sepsis, or removal of irritants for inhalation injuries.
The management of pulmonary edema is often an intensive process requiring close monitoring. Mobile health (mHealth) apps and wearable devices are increasingly being used to monitor vital signs remotely, allowing for earlier detection of potential issues and better management of chronic conditions. The financial aspect of managing such a condition can be substantial, involving hospital stays, medications, and ongoing medical care, underscoring the importance of health insurance and accessible healthcare systems.
In conclusion, edema of the lungs is a serious condition that demands prompt recognition and expert medical management. By understanding its diverse causes, recognizing its often-distressing symptoms, and appreciating the role of advanced diagnostics and personalized treatment strategies, we can improve outcomes for individuals affected by this potentially devastating respiratory ailment. The ongoing evolution of technology and its integration into healthcare promises even more effective ways to diagnose, monitor, and manage pulmonary edema in the future.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.