Mental health courts represent a groundbreaking intersection of the legal system and the imperative to address mental illness with compassion and efficacy. These specialized court dockets are not designed to replace traditional criminal justice proceedings, but rather to offer an alternative, rehabilitative pathway for individuals whose mental health conditions have intersected with the law. At their core, mental health courts aim to divert individuals with mental illness away from incarceration and towards treatment and support services, fostering recovery, reducing recidivism, and ultimately building safer communities.
The emergence of mental health courts is a direct response to a growing understanding of the profound impact mental illness has on individuals within the criminal justice system. For decades, the prevailing approach often resulted in individuals with treatable mental health conditions cycling through jails and prisons, where their conditions were frequently exacerbated rather than addressed. This not only proved detrimental to the individuals involved but also placed an enormous strain on correctional facilities and taxpayer resources. Mental health courts offer a more humane and cost-effective solution by recognizing that in many instances, mental illness, not inherent criminality, is the primary driver of an individual’s legal troubles.
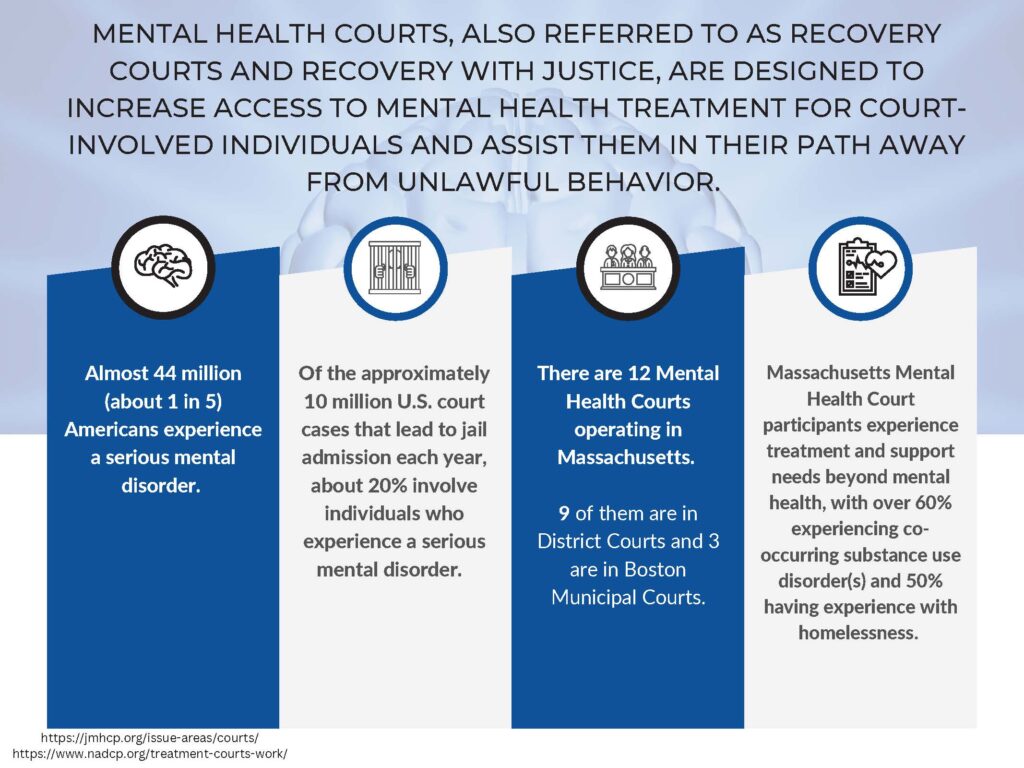
These courts operate on a collaborative model, bringing together a multidisciplinary team of professionals. This team typically includes judges, prosecutors, defense attorneys, mental health professionals (such as psychiatrists, psychologists, and social workers), probation officers, and case managers. This integrated approach allows for a comprehensive assessment of the defendant’s needs, the development of tailored treatment plans, and ongoing monitoring to ensure compliance and progress. The success of a mental health court hinges on this coordinated effort, ensuring that both the legal and therapeutic aspects of a case are addressed simultaneously.
The Core Principles and Functioning of Mental Health Courts
At the heart of any mental health court lies a commitment to a rehabilitative rather than purely punitive approach. While accountability for actions remains a fundamental aspect, the focus shifts towards understanding the underlying causes of criminal behavior, particularly when those causes are rooted in mental illness. This paradigm shift is crucial for breaking cycles of recidivism and enabling individuals to reintegrate into society as productive citizens.
Understanding the Referral and Eligibility Process
The journey into a mental health court typically begins with a referral. This can originate from various points within the legal system, including law enforcement officers at the scene of an alleged offense, prosecutors during the charging phase, defense attorneys advocating for their clients, or even judges observing a defendant’s presentation in court. Not every individual with a mental health diagnosis automatically qualifies for mental health court. Eligibility criteria are rigorously defined and vary across jurisdictions, but generally revolve around demonstrating that the defendant’s mental illness played a significant role in the alleged offense and that they are willing and able to participate in the court’s program.
Crucially, mental health courts are not a loophole for serious or violent crimes where mental illness may be a contributing factor but not the sole or primary cause of the offense. The offenses typically addressed are often less severe, such as minor drug possession, theft, public intoxication, or other offenses where a direct link to untreated or undertreated mental illness can be established. The defendant must typically plead guilty or acknowledge their involvement in the offense to be admitted into the program, signifying a willingness to engage with the process.
The Intensive Supervision and Treatment Model
Once deemed eligible and admitted, participants in a mental health court enter a period of intensive supervision and mandatory treatment. This is the cornerstone of the program and is highly individualized. Upon entry, a comprehensive diagnostic assessment is conducted by mental health professionals. This assessment evaluates the individual’s mental health diagnosis, the severity of their symptoms, their risk of harm to themselves or others, their substance use history, their support systems, and their immediate needs.
Based on this assessment, a personalized treatment plan is developed. This plan can encompass a wide array of services, including:
- Psychiatric medication management: Ensuring individuals have access to necessary prescriptions and are adhering to their medication regimens.
- Therapy and counseling: This can include individual therapy, group therapy, cognitive behavioral therapy (CBT), dialectical behavior therapy (DBT), and other evidence-based interventions tailored to the individual’s specific diagnosis and challenges.
- Substance use disorder treatment: Many individuals with mental illness also struggle with co-occurring substance use disorders, requiring integrated treatment approaches.
- Case management: Connecting individuals with essential support services such as housing assistance, employment services, vocational training, and educational opportunities.
- Life skills training: Developing crucial skills for independent living, such as budgeting, cooking, and social interaction.
- Support groups: Facilitating connections with peer support networks that can offer encouragement and understanding.
Participants are regularly monitored for compliance with their treatment plans and court requirements. This monitoring involves frequent court appearances, drug and alcohol testing, meetings with probation officers and case managers, and communication with treatment providers. The frequency and intensity of these check-ins are typically determined by the participant’s progress and risk level, with more frequent contact for those who are struggling and less frequent for those who are demonstrating consistent progress.
Graduated Sanctions and Incentives for Progress
A key element that distinguishes mental health courts from traditional judicial processes is their use of graduated sanctions and incentives. This system recognizes that recovery is not always linear and that individuals may experience setbacks.
- Sanctions: When a participant fails to comply with their treatment plan or court orders, a system of graduated sanctions is implemented. These sanctions are designed to be corrective rather than purely punitive. They might include increased frequency of court appearances, mandatory attendance at additional therapy sessions, short-term jail or detention, community service, or loss of privileges. The goal is to address the non-compliance promptly and steer the individual back towards their recovery path.
- Incentives: Conversely, significant emphasis is placed on recognizing and rewarding positive progress. When participants successfully meet their treatment goals, demonstrate consistent sobriety, maintain stable housing, and achieve other milestones, they are acknowledged and rewarded. Incentives can range from praise and encouragement in court to reduced supervision, increased autonomy in their treatment, or early graduation from the program. This positive reinforcement is vital for motivation and sustained engagement in the recovery process.

The judge plays a pivotal role in this dynamic process, acting as a central figure who oversees the participant’s progress, imposes sanctions when necessary, and celebrates successes. The court appearances themselves are often less formal than traditional court proceedings, fostering a more therapeutic and encouraging environment.
The Multifaceted Benefits of Mental Health Courts
The impact of mental health courts extends far beyond the individuals directly participating in them. These innovative judicial mechanisms offer a spectrum of benefits for individuals, the justice system, and the broader community.
For Individuals: Recovery, Rehabilitation, and Reintegration
The most profound benefit of mental health courts is the opportunity for individuals to receive the treatment and support they need to manage their mental health conditions effectively. For many, this is the first time they have accessed such services in a structured and supportive environment.
- Improved Mental Health Outcomes: By connecting individuals with appropriate mental healthcare, mental health courts facilitate symptom reduction, improved functioning, and a better quality of life.
- Reduced Recidivism: When mental health needs are addressed, the likelihood of an individual re-offending due to their illness is significantly diminished. Studies have consistently shown lower rates of re-arrest and re-incarceration among mental health court graduates compared to those who pass through traditional courts.
- Empowerment and Agency: The program encourages participants to take an active role in their recovery, fostering a sense of agency and self-efficacy.
- Stable Housing and Employment: The comprehensive case management services provided can help individuals secure stable housing and employment, which are critical factors in long-term recovery and reducing the risk of homelessness and criminal activity.
- Strengthened Family Relationships: By promoting stability and well-being, mental health courts can help repair strained family relationships and reintegrate individuals into their communities.
For the Justice System: Efficiency, Cost-Effectiveness, and Reduced Strain
Mental health courts offer tangible advantages for the efficiency and effectiveness of the criminal justice system.
- Reduced Jail and Prison Overcrowding: By diverting individuals with mental illness from correctional facilities, these courts alleviate pressure on already overburdened systems.
- Cost Savings: While initial investments in treatment services are required, the long-term costs associated with incarceration, repeated arrests, and repeated trials are significantly reduced. The cost of providing community-based treatment is generally far less than the cost of incarceration.
- More Focused Judicial Resources: By handling cases involving mental illness in a specialized setting, traditional courts can dedicate their resources to other types of cases, leading to greater efficiency.
- Improved Public Safety: By addressing the root causes of criminal behavior in individuals with mental illness, these courts contribute to safer communities by reducing the likelihood of future offenses.
For the Community: Compassion, Public Health, and Reduced Stigma
The establishment of mental health courts reflects a growing societal understanding and commitment to addressing mental illness with compassion and evidence-based practices.
- Enhanced Public Health: By improving the mental and physical well-being of individuals, mental health courts contribute to the overall public health of the community.
- Reduced Stigma: The success of mental health courts helps to de-stigmatize mental illness by demonstrating that individuals with these conditions can recover and live productive lives when provided with appropriate support.
- Model for Future Interventions: The positive outcomes of mental health courts serve as a compelling model for developing other specialized court dockets and justice-involved diversion programs.
Challenges and the Future of Mental Health Courts
Despite their proven success, mental health courts are not without their challenges. Ensuring their widespread accessibility, adequate funding, and ongoing effectiveness requires continuous effort and adaptation.
One significant challenge is the variability in funding and resources across different jurisdictions. The success of a mental health court is directly tied to the availability of robust mental health services, qualified personnel, and consistent court support. Inadequate funding can lead to long waiting lists for treatment, insufficient staffing, and ultimately, compromised outcomes. Advocates emphasize the need for sustainable funding models that recognize mental health courts as a critical investment in public health and safety.
Another ongoing consideration is the development and refinement of evidence-based practices. As our understanding of mental illness and effective treatments evolves, so too must the programs offered within mental health courts. This includes staying abreast of advancements in therapeutic interventions, medication management, and recovery-oriented care. The integration of technology, such as telehealth for remote therapy sessions or digital platforms for case management, also presents opportunities and challenges for enhancing accessibility and efficiency.
Furthermore, building and maintaining strong collaborative partnerships among all stakeholders is paramount. This includes fostering effective communication between the courts, mental health providers, law enforcement, and community organizations. Overcoming inter-agency silos and ensuring a shared understanding of goals and responsibilities is crucial for seamless operation.
The future of mental health courts looks promising, with an increasing recognition of their value and a growing number of jurisdictions implementing these specialized dockets. As the legal system continues to grapple with the complexities of mental illness, mental health courts offer a beacon of hope, demonstrating that a more just, compassionate, and effective approach is not only possible but achievable. Their continued expansion and evolution are essential steps towards a society that truly supports the well-being and recovery of all its members.
aViewFromTheCave is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.